Successful Transcatheter Stent Intervention of Peripheral Pulmonary Artery Stenosis in Williams-Beuren Syndrome
© 2025 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of the Journal of Invasive Cardiology or HMP Global, their employees, and affiliates.
A 15-year-old girl presented with increasing chest tightness and worsening shortness of breath for 2 weeks. She was diagnosed with Williams-Beuren syndrome (WBS) after genetic testing 6 months earlier.
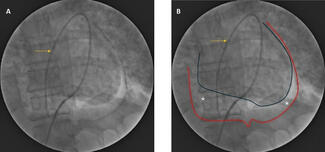
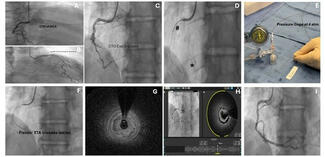
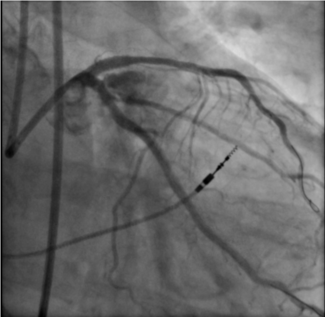
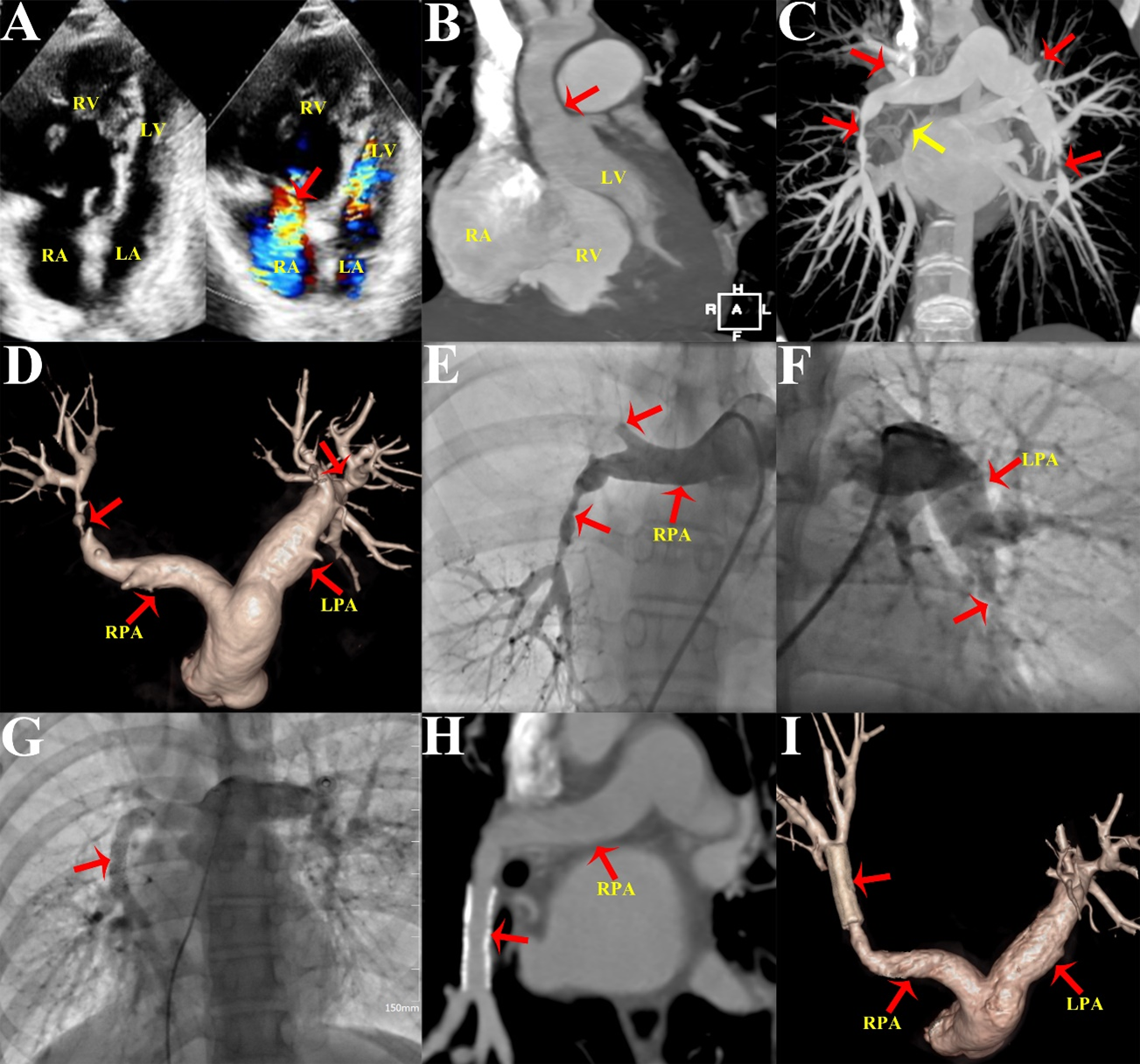
Laboratory examination was unremarkable. Electrocardiogram revealed bilateral ventricular hypertrophy and a prolonged QT interval. Transthoracic echocardiography showed right heart enlargement, severe tricuspid regurgitation, and an estimated main pulmonary artery (PA) pressure of 67 mm Hg (Figure A). Computed tomography angiography (CTA) revealed mild supravalvular aortic stenosis (Figure B), bilateral multiple peripheral PA stenosis and occlusion, and right superior pulmonary vein occlusion (Figure C and D). Pulmonary angiography revealed that the right middle and superior pulmonary arteries were occluded, and the right inferior pulmonary artery (RIPA) was severely stenotic with a pressure gradient of 63 mm Hg (Figure E; Video S1). Additionally, there was left PA trunk dilatation and left inferior PA stenosis (Figure F; Video S2). Right heart catheterization revealed an elevated central PA pressure of 53 mm Hg. Transcatheter RIPA stenting was performed using an 8 mm x 29-mm Omnilink Elite stent (Abbott) (Figure G; Video S3); the pressure of the RIPA decreased to 26 mm Hg.
The postoperative course was uneventful, and the patient was discharged after a 7-day stay. Follow-up after 12 months revealed that her symptoms had significantly improved. PA CTA showed stent patency (Figure H and I).
WBS is a multisystem genetic disorder affecting the cardiovascular, connective tissue, and central nervous systems.1 Mitral valve prolapse, pulmonary arterial stenosis, and supravalvular aortic stenosis are the most prevalent cardiovascular disorders. Aortic coarctation, ventricular septal defect, patent ductus, and hypertrophic cardiomyopathy are uncommon cardiac conditions.2 WBS-associated peripheral PA stenosis generally yields severe hemodynamic abnormalities, and the diagnostic and treatment strategies are challenging.
Advanced imaging of the arterial tree using either CTA or cardiovascular magnetic resonance imaging should be considered in patients with moderate or severe peripheral PA stenosis.3 CTA can give precise details for planning, navigating, and noninvasive assessment of secondary arterial changes in WBS, eliminating the need for invasive contrast catheterization procedures. Despite surgical PA reconstruction remaining the preferred approach for WBS-associated peripheral PA stenosis, transcatheter interventions may also be pursued out of necessity due to specific associated morbidities or the lack of surgical expertise; stent placement can be performed to achieve acute hemodynamic outcomes and improve prognosis.4
Affiliations and Disclosures
Leizhi Ku, MD1; Yuhang Wang, MD1; Xiaojing Ma, PhD2
From the Departments of 1Radiology and 2Echocardiography, Wuhan Asia Heart Hospital Affiliated to Wuhan University of Science and Technology, Wuhan, P.R. China.
Dr Ku and Dr Wang have contributed equally to the article.
Disclosures: The authors report no financial relationships or conflicts of interest regarding the content herein.
Funding: This work was funded by the Wuhan Clinical Medical Research Center for Cardiovascular Imaging (CMRC202307).
Address for correspondence: Xiaojing Ma, PhD, Department of Echocardiography, Wuhan Asia Heart Hospital Affiliated to Wuhan University of Science and Technology, No.753 Jinghan Road, Hankou District, Wuhan, P.R. 430022, China. Email: klz1534292102@163.com
References
- Collins RT II, Collins MG, Schmitz ML, et al. Peri-procedural risk stratification and management of patients with Williams syndrome. Congenit Heart Dis. 2017;12(2):133-142. doi:10.1111/chd.12424
- Das KM, Momenah TS, Larsson SG, et al. Williams-Beuren syndrome: computed tomography imaging review. Pediatr Cardiol. 2014;35(8):1309-1320. doi:10.1007/s00246-014-0946-6
- Collins RT II, Gravenhorst V, Faury G, et al. Clinical care for cardiovascular disease in patients with Williams-Beuren syndrome. J Am Heart Assoc. 2024;13(19):e036997. doi:10.1161/JAHA.124.036997
- Lan IS, Yang W, Feinstein JA, et al. Virtual transcatheter interventions for peripheral pulmonary artery stenosis in Williams and Alagille syndromes. J Am Heart Assoc. 2022;11(6):e023532. doi:10.1161/JAHA.121.023532