Managing Interstitial Plantar Fascial Tears in Chronic Heel Pain: Diagnosis and Treatment Strategies
Plantar fasciitis is one of the most common complaints foot and ankle providers diagnose and treat. Interstitial tearing of the plantar fascia is prevalent, especially in chronic or recalcitrant heel pain patients. These authors describe their experience treating interstitial tears of the plantar fascia.
Key Takeaways
- Interstitial plantar fascial tears are common in chronic heel pain and may be present in over one-third of patients with recalcitrant symptoms, underscoring the importance of advanced imaging and avoiding empiric corticosteroid injection when a tear is suspected or confirmed.
- Immobilization is foundational once an interstitial tear is identified, with CAM boot offloading serving as a critical first step to reduce rupture risk and optimize outcomes before adjunctive therapies are introduced.
- Biologic and energy-based therapies offer effective nonoperative options, with shockwave therapy and platelet-rich plasma (PRP) demonstrating favorable outcomes in pain reduction and functional improvement, while surgical repair remains a reliable option for patients who fail conservative and regenerative treatments.
Plantar fasciitis is one of the most common causes of outpatient visits in the United States, and accounts for approximately 1 million patient visits yearly.1 Plantar fasciitis is defined as a degenerative process and overuse injury, often attributed to overall foot type placing excess strain on the plantar fascia.2 Equinus, or a tight Achilles tendon, is often considered one of the driving forces behind plantar fasciitis, placing excessive strain on the plantar heel.3
Treatment for acute plantar fasciitis often consists of multiple conservative modalities in the office, although it can take weeks to months to resolve.4 Stretching and strengthening is one of the first line treatments for plantar fasciitis, which focuses on reducing the impact of the equinus and also with soft tissue mobilization of the plantar fascial aponeurosis.5 Shoe gear modifications with better supportive/fitting shoes, in addition to inserts that help support the foot architecture, are also part of the treatment algorithm and aim to help reduce future flares.6-7 Local injectable corticosteroid therapy is often an early line of therapy for acute plantar fasciitis, especially when patients need to get back to activity quickly.8 Although effective, injectable corticosteroids have their own side effect profile, as local infiltration of steroid around soft tissue structures can in fact weaken tendons/ligaments by affecting collagen synthesis.9 Local administration of steroid therapy is used sparingly in our hands.
Regenerative medicine has also seen increased utilization, especially for plantar fasciitis. For plantar fasciitis, shockwave therapy (extracorporeal shockwave therapy (ESWT) or extracorporeal pulse activation technology (EPAT)) has emerged as a viable treatment option. Although most devices are FDA-cleared, shockwave therapy is generally not covered by insurance, but nonetheless offers a noninvasive option. Shockwave utilizes high energy sound waves to stimulate tissue healing by causing local microtrauma, promoting angiogenesis, and acts as a pain modulator.10 Study and usage of shockwave therapy exists for many different musculoskeletal pathologies across the human body. To date, literature supports using shockwave therapy to improve function, decrease pain, and increase overall quality of life, especially in patients with plantar fasciitis.11 Specifically, one study found shockwave therapy as effective as local corticosteroid therapy without the added risks.12
Platelet-rich plasma (PRP) therapy is a trending subset of orthobiologic medicine as a nonoperative treatment with varying results. PRP utilizes one’s own blood to concentrate platelets and growth factors for localized injection.13 While PRP efficacy and optimization is still under study in the medical community, it does appear to have early success, especially in soft tissue injuries. For plantar fasciitis, evidence not only supports PRP’s safety for chronic plantar fasciitis and role in improving pain and functionality, but it can also help with reducing plantar fascial thickness.14-15 While PRP is FDA approved, this is also a treatment modality typically not covered under insurance.
The authors of this article have presented their yet-unpublished findings on the prevalence of interstitial tears of the plantar fascia, and find it occurs in approximately 36.67% of patients presenting with chronic heel pain. Interstitial tears complicate treatment, as, if the tear is not addressed appropriately it can lead to rupture of the plantar fascia. Injectable corticosteroid therapy is not indicated when one identifies an interstitial tear. The purpose of this article is to present the authors’ treatment recommendations in the setting of an interstitial plantar fascial tear.
Walking Through the Clinical Process: History and Physical
We define acute plantar fasciitis as first-time plantar fasciitis, or heel pain for less than 6 weeks. These patients often experience pain in the bottom of their foot, which hurts when taking the first step after being off of their foot for an extended period of time. Typically, this pain gets better throughout the day. In contrast, patients with chronic heel pain are those with recurring heel pain, heel pain lasting more than 3 months, or with symptoms that do not align with traditional plantar fasciitis. Oftentimes, patients with interstitial tears of the plantar fascia still do have the hallmark “first step” pain, but they often relate the pain worsening as the day goes on. Patients with chronic heel pain have often also tried conservative modalities in the past, with no success.
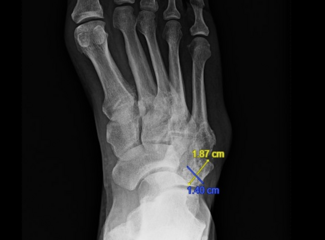
On physical examination, patients with chronic heel pain exhibit symptoms at the aponeurosis of the plantar fascia and the physician can sometimes feel palpable underlying scar tissue. Equinus is also a driving force, as discussed, especially with chronic heel pain and must be part of the treatment plan to optimize outcomes. We often recommend magnetic resonance imaging (MRI) of the affected extremity without contrast to give better information on the integrity of the plantar fascia. Interstitial tears diagnosis can also result from ultrasound, but the authors have found it quite difficult to truly diagnose due to the extent of chronic degenerated scar tissue. Thus, we commonly pursue MRI for diagnosis. While all views are integral in defining the integrity of the plantar fascia, we have found the coronal and axial views to give better information, and the sagittal view allows thickness calculation. The authors of this article have presented unpublished data on the correlation of plantar fascial thickness and interstitial tearing of the plantar fascia and have found an average thickness of 6.04mm. Patients then return to our clinic for MRI review and treatment recommendations.
Our Treatment Pathways
Immobilization. Once we diagnose an interstitial tear of the plantar fascia, we often recommend placing patients into a CAM boot for immobilization. We find this allows for decreased strain on the fascia and decreased pain overall. We recommend immobilization for at least 4 weeks, and up to 2 months depending on how or if the symptoms resolve. Immobilization is the key first step for treating this pathology, because with chronic scar tissue and interstitial tearing, it is very possible for the plantar fascia to rupture. After an appropriate timeline of immobilization, we then transition patients to weight-bearing in sneakers and we recommend either over-the-counter or custom orthotics to help continue offloading the plantar fascia. We often recommend formal physical therapy at this point with a focus on anti-inflammatory modalities, ultrasound, stretching, and overall strengthening.
Shockwave Therapy. Shockwave therapy (ESWT and EPAT) have been shown to be effective treatment options for plantar fasciitis, both acute and chronic cases.10-12 In our outpatient foot and ankle clinic, we often recommend shockwave therapy as a noninvasive treatment option for chronic plantar fasciitis and with patients with interstitial tears. We utilize an ESWT system in our clinic with 120mJ of energy and at 12 hZ. We still immobilize patients with interstitial tears in a tall CAM boot, but will also recommend they undergo 6 treatments of high-intensity shockwave therapy. We usually space these appointments out 5-7 days. All patients are to cease nonsteroidal anti-inflammatory drug (NSAID) therapy for 7-12 days prior to beginning shockwave treatment and will remain off all NSAIDs for 4 weeks during the treatment. This ensures we can maximize the inflammatory response at the plantar fascial aponeurosis. We check in with all patients right before their fifth shockwave treatment as the first official check-in, and then 7 weeks after that, which will be 3 months after the initiation of treatment. At the first official check-in, we typically can discontinue the CAM boot and get patients back into regular walking sneakers with accommodative inserts. We then see the patient back in 3 additional months, which is 6 months out from starting treatment. With shockwave therapy, some patients get an immediate response, some get a delayed response, and some get no response. As the shockwave treatment is designed to break the chronic inflammation cycle and create an acute inflammatory state, response to treatment varies and we tell all of our patients we normally know how the patient truly responded to shockwave at the 6 month follow-up.
Platelet Rich Plasma (PRP). We use this modality to enhance the biology in the area, and often augment with either shockwave or laser to enhance the effects of PRP. In our office we draw 60cc of blood from the patient, which we then spin in a centrifuge to separate the blood into its vital components. We then further concentrate the buffy coat layer to yield high-dose PRP with some leukocytes to assist in soft tissue regeneration. Finally, we inject this into the plantar fascia under direct ultrasound guidance to ensure that we envelope the interstitial tear with high-dose PRP. Patients are still immobilized with a tall CAM boot for 4 weeks with PRP therapy, as the body tries to heal the interstital tear.
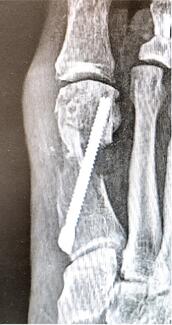
Endoscopic Debridement with Interstitial Tear Repair. Patients who have had failed conservative treatment options, or ones who fail shockwave and/or PRP therapy may often go on to surgical intervention. The senior author of this paper has published results on endoscopic debridement without cutting the ligament for chronic plantar fasciitis as an alternative to endoscopic plantar fasciotomy, and has 98% satisfaction with 5 years of follow up.16-17 Currently, the authors are investigating outcomes with a novel technique to repair these interstitial tears. In the very short term, we currently observe a high satisfaction rate, decreased pain, and increased functionality. We will be publishing our short-term data soon. Patients who undergo operative intervention are allowed to weight-bear to tolerance in a tall CAM boot after surgery. They start physical therapy at postop week 3, and then are out of the CAM boot at week 4 and often go back into regular sneakers.
Conclusion
Chronic heel pain, or, recalcitrant plantar fasciitis often poses obstacles in treatment, especially in the context of interstitial tears. The authors have had great success with all of the above treatments, but, for patients looking for a quicker return to activity, we feel that a combination of shockwave and PRP therapy provides a nonoperative treatment with good outcomes in our hands, to date.
Dr. Cottom is a fellowship-trained foot and ankle surgeon with Florida Orthopedic Foot and Ankle Center, where he serves as Fellowship Director. He is a Fellow of the American College of Foot and Ankle Surgeons.
Dr. Verdoni is an Associate of the American College of Foot and Ankle Surgeons and prior surgical fellow at Evolve Health/Florida Orthopedic Foot and Ankle Center. He is a current attending physician at Seaview Orthopaedic and Medical Associates in New Jersey.
References
1. Buchanan BK, Sina RE, Kushner D. Plantar Fasciitis. [Updated 2024 Jan 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK431073/
2. Mørk M, Soberg HL, Hoksrud AF, Heide M, Groven KS. The struggle to stay physically active-A qualitative study exploring experiences of individuals with persistent plantar fasciopathy. J Foot Ankle Res. 2023 Apr 15;16(1):20.
3. Riddle DL, Pulisic M, Pidcoe P, Johnson RE. Risk factors for plantar fasciitis: a matched case-control study. J Bone Joint Surg Am. 2003 May;85(5):872-7.
4. Fouda KZ, Ali ZA, Elshorbagy RT, Eladl HM. Effect of radial shock wave and ultrasound therapy combined with traditional physical therapy exercises on foot function and dorsiflexion range in plantar fasciitis: a prospective randomized clinical trial. Eur Rev Med Pharmacol Sci. 2023 May;27(9):3823-3832.
5. Thong-On S, Bovonsunthonchai S, Vachalathiti R, Intiravoranont W, Suwannarat S, Smith R. Effects of strengthening and stretching exercises on the temporospatial gait parameters in patients with plantar fasciitis: a randomized controlled trial. Ann Rehabil Med. 2019 Dec;43(6):662-676. doi: 10.5535/arm.2019.43.6.662. Epub 2019 Dec 31. PMID: 31918529; PMCID: PMC6960082.
6. Wapner KL, Sharkey PF. The use of night splints for treatment of recalcitrant plantar fasciitis. Foot Ankle. 1991 Dec;12(3):135-7.
7. Pfeffer G, Bacchetti P, Deland J, et al. Comparison of custom and prefabricated orthoses in the initial treatment of proximal plantar fasciitis. Foot Ankle Int. 1999 Apr;20(4):214-21.
8. Karakılıç GD, Aras M, Büyük F, Bakırcı EŞ. Prolotherapy versus phonophoresis and corticosteroid injections for the treatment of plantar fasciitis: a randomized, double-blind clinical trial. J Foot Ankle Surg. 2023 Nov-Dec;62(6):922-927.
9. Mikolyzk DK, Wei AS, Tonino P, et al Effect of corticosteroids on the biomechanical strength of rat rotator cuff tendon. J Bone Joint Surg Am. 2009 May;91(5):1172-80. doi: 10.2106/JBJS.H.00191. PMID: 19411466; PMCID: PMC7002078.
10. Simplicio CL, Purita J, Murrell W, Santos GS, Dos Santos RG, Lana JFSD. Extracorporeal shock wave therapy mechanisms in musculoskeletal regenerative medicine. J Clin Orthop Trauma. 2020 May;11(Suppl 3):S309-S318. doi: 10.1016/j.jcot.2020.02.004. Epub 2020 Feb 12. PMID: 32523286; PMCID: PMC7275282.
11. Leão RG, Azuma MM, Ambrosio GHC, Faloppa F, Takimoto ES, Tamaoki MJS. Effectiveness of shockwave therapy in the treatment of plantar fasciitis. Acta Ortop Bras. 2020 Jan-Feb;28(1):7-11. doi: 10.1590/1413-785220202801227402. PMID: 32095104; PMCID: PMC7006537.
12. Grady J, Boumendjel Y, LaViolette K, Smolinski T. Extracorporeal pulse-activated therapy versus injection: treatment of recalcitrant plantar fasciitis. J Am Podiatr Med Assoc. 2019 Mar;109(2):108-112. doi: 10.7547/17-075. PMID: 31135197.
13. Jain NK, Gulati M. Platelet-rich plasma: a healing virtuoso. Blood Res. 2016 Mar;51(1):3-5. doi: 10.5045/br.2016.51.1.3. Epub 2016 Mar 25. PMID: 27104183; PMCID: PMC4828525.
14. Kothari U, Shah S, Pancholi D, Chaudhary C. Efficacy and safety of platelet-rich plasma injection for chronic plantar fasciitis: a prospective study on functional restoration and pain relief. Cureus. 2024 Jan 16;16(1):e52414. doi: 10.7759/cureus.52414. PMID: 38371014; PMCID: PMC10869993.
15. Yang WY, Han YH, Cao XW, et al. Platelet-rich plasma as a treatment for plantar fasciitis: A meta-analysis of randomized controlled trials. Medicine (Baltimore). 2017 Nov;96(44):e8475. doi: 10.1097/MD.0000000000008475. PMID: 29095303; PMCID: PMC5682822.
16. Cottom JM, Baker JS. endoscopic plantar fascia debridement for chronic plantar fasciitis. Clin Podiatr Med Surg. 2016 Oct;33(4):545-51. doi: 10.1016/j.cpm.2016.06.004. Epub 2016 Jul 27. PMID: 27599439.
17. Cottom JM, Wolf JR, Sisovsky CA. Midterm outcomes of endoscopic plantar fascia debridement in 125 patients: a 5-year follow-up. J Foot Ankle Surg. 2023;62(3):444-447. doi:10.1053/j.jfas.2022.11.001
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Podiatry Today or HMP Global, their employees, and affiliates.