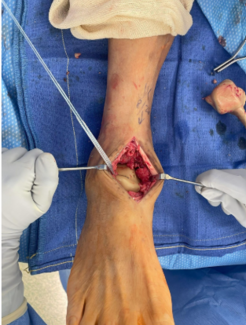
Wound Salvage After Total Ankle Replacement: Multidisciplinary Management of Postoperative Dehiscence
Key Takeaways
-
Early, aggressive intervention is critical in suspected implant communication. Prompt surgical debridement, negative pressure wound therapy (NPWT), and infectious disease consultation can prevent progression to deep infection and prosthetic failure following Total Ankle Replacement.
-
Multidisciplinary coordination improves implant salvage rates. Collaboration between foot and ankle surgery, infectious disease, and plastic surgery enables structured escalation of care—particularly when soft tissue compromise threatens implant viability.
-
Free tissue transfer can achieve durable long-term outcomes. In cases of full-thickness defects or compromised soft tissue envelopes after total ankle arthroplasty, microvascular free flap reconstruction (eg, gracilis muscle flap with STSG) can result in sustained implant function and infection-free survival at extended follow-up (57 months in this case).
Complex Wound Management Following Total Ankle Replacement
Wound complications after Total Ankle Replacement (TAR)—also referred to as Total Ankle Arthroplasty (TAA)—can be limb threatening and jeopardize implant survival. Despite advances in third-generation prosthetic systems, postoperative wound dehiscence with potential implant communication remains a serious complication requiring early, coordinated intervention. This case study presented at the American College of Foot and Ankle Surgeons (ACFAS) Annual Scientific Conference, February 2026, Las Vegas, NV, highlights successful long-term limb and implant salvage following complex wound breakdown after TAA.1
Case Presentation and Surgical Course
In April 2018, a 64-year-old woman underwent total ankle arthroplasty using a third-generation ankle system. Six weeks postoperatively, she developed a superficial wound dehiscence. Given concern for possible implant communication, the patient underwent surgical debridement with partial wound closure and application of negative pressure wound therapy (NPWT) at eight weeks postoperatively.1
Soft tissue cultures were obtained and returned negative. Infectious disease consultation was obtained, and the patient completed six weeks of intravenous antibiotics per specialist recommendations. Due to persistent soft tissue compromise, plastic surgery was consulted. In September 2018, the patient underwent microvascular free gracilis muscle flap reconstruction with split-thickness skin grafting (STSG) for definitive soft tissue coverage.1
Long-Term Outcomes After Total Ankle Arthroplasty Complication
The patient healed uneventfully following reconstruction. At final follow-up—57 months postoperatively—the flap remained viable, implant function was intact, and there was no evidence of recurrent infection. At nearly five years after total ankle replacement, the patient maintained complete flap survival and stable prosthetic alignment.1
Clinical Implications for Foot and Ankle Surgeons
The poster authors contended that wound dehiscence after total ankle arthroplasty requires early recognition and aggressive management to prevent catastrophic implant failure. This case reinforces several key principles:
-
Early multidisciplinary coordination (foot and ankle surgery, infectious disease, plastic surgery) improves limb salvage potential.
-
NPWT and prompt debridement are critical when implant communication is suspected.
-
Free tissue transfer, including gracilis muscle flap reconstruction, may be necessary in cases involving full-thickness defects or compromised soft tissue envelopes.
The durable five-year outcome in this case underscores that even complex postoperative wound complications following total ankle replacement can be successfully managed with a structured, collaborative approach.
Reference
-
Egdorf JR, Hilton CJ, Keaton J, Laxson SE. Complex wound management following wound dehiscence after total ankle replacement. Poster presented at: American College of Foot and Ankle Surgeons Annual Scientific Conference; February 2026; Las Vegas, NV.
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Podiatry Today or HMP Global, their employees, and affiliates.