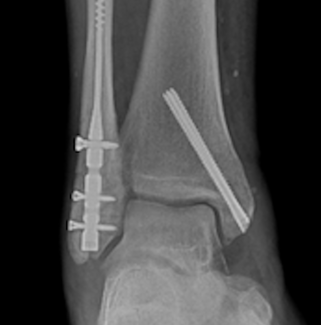
Notes on Biointegrative Fixation
Key Takeaways
1. Biointegrative fixation becomes bone over time.
Unlike traditional metal hardware, these silica–calcium phosphate implants integrate and are replaced by native bone, eliminating long-term retained hardware.
2. Reduced hardware removal and better imaging are major advantages.
Biointegrative implants minimize irritation, avoid secondary removal surgeries, and improve MRI/CT visualization without metal artifact.
3. Comparable strength — with future expansion ahead.
Current screws, staples, nails, and anchors offer fixation strength similar to metal, with plates likely forthcoming. The long-term trend may shift away from metal fixation in many foot and ankle procedures.
Transcript
Jennifer Spector, DPM:
Welcome back again everybody to Podiatry Today Podcasts, where we bring you the latest in foot and ankle medicine and surgery from leaders in the field. Today, we are so excited to have Dr. Bob Baravarian back with us again this time to talk about biointegrative non-metal fixation in foot and ankle surgery. If you missed our last episode where he was talking about biologics in foot and ankle pathology, be sure to go back and see that other episode. But today we're thrilled to be welcoming him back. He's a fellow of the American College of Foot and Ankle Surgeons, board certified in foot surgery and reconstructive rear foot and ankle surgery, co-director of the University Foot and Ankle Institute and Assistant Clinical Professor at UCLA School of Medicine. And last but not least, he's a member of our editorial advisory board for Podiatry Today. Welcome back, Doc. We're so glad to have you here.
Bob Baravarian, DPM:
Thank you for having me. I appreciate it.
Jennifer Spector, DPM:
So to start us out, could you walk us through what exactly is biointegrative non-metal fixation and how does it differ from traditional metal fixation in foot and ankle surgery?
Bob Baravarian, DPM:
So biointegrative fixation is a material that will over the period of anywhere between six months and a couple of years, integrate and become bone. So unlike what we used to know 20, 30 years ago, which was called absorbable, which was a problem because as the material absorbed, you had cystic changes and you were left with a void. Biointegrative material is a combination of silica and calcium phosphate that actually is naturally occurring in the body and your body will actually fill it like a bone graft and replace it. Unlike bone graft material or bone screws, the biointegrated material can be, and in many cases, is as strong as metal at the time of fixation. And unlike metal where you can have reaction, have cold allergy, have nickel allergy, have a need for removal, biointegrative material actually adheres to the bone, becomes stronger and gets completely replaced by the body's own bone. So there's nothing to remove and nothing that can cause reaction.
Jennifer Spector, DPM:
That's great. What are some of the main clinical advantages that you've observed? Is there anything to note in terms of healing or imaging or patient recovery?
Bob Baravarian, DPM:
All of that. So the number one thing is I tell our fellows, I say the worst surgery for me to do is a hardware removal. You've done the perfect surgery, everything's great, the patient's happy, and now there's a screw bothering them and you have to go remove it. And first of all, it's not a fun surgery. Second of all, removing screws is not easy to do. And third of all, the only thing that comes of it is, oh, the screw had broke or it's stripped, or I had a hard time getting it out or I had to dig it out. It's really not good for the patient. It's not good for the economics of healthcare, and it's not good for you as a physician because you can only do bad. Otherwise, it's expected that you're going to take the screw out and it'd be perfect.
The other thing that we notice is MRIs and even CTs, the quality of the image is degraded by the metal. And the third thing that I always tell patients and I tell other doctors is the strongest point at which you put in a metal screw is at the point where you tighten it. So you pat yourself on the back, you say, "I put in this screw. Look how tight it is. Great, great, great." As the person starts to walk on it, that screw will only loosen. It will not get tighter. Whereas with biointegrated material, once you put the biointegrated material in, it's tight. But as the body starts to adhere to it, and there's a sticky factor with these biointegrative screws and pins and staples, as it gets stickier, it actually becomes stronger and it adheres to the bone. So I see less inflammation, very, very little chance of having to remove it and far less irritation from the material.
Jennifer Spector, DPM:
Are there any sort of ideal patient scenarios for these to be used or conversely, any contraindications to be aware of?
Bob Baravarian, DPM:
I don't think there's any contraindications. I think there's places where you need a large plate, like let's say a fibular fracture, and these materials don't come in plate format yet. But other than that, there really is, to me, no reason why you should use metal if you can use one of these biointegrative screws. I know that we all really like looking at metal on an x-ray and being like, "Look at what we put in here." But when a patient sees it, they're horrified. And a clean x-ray, which I call ghost surgery, a clean x-ray to them is amazing. So again, you're patting yourself on the back, but they're not patting you on the back. They would rather not have this stuff in their foot.
Jennifer Spector, DPM:
Does your surgical workflow change at all when you're using biointegrative fixation over traditional hardware?
Bob Baravarian, DPM:
No, not at all. It's exactly the same, exactly the same sort of fixation, exactly the same structural adherences. It really doesn't change anything at all for me.
Jennifer Spector, DPM:
Well, to round out this discussion today, I'm curious what you feel are maybe the next steps for biointegrative fixation. What do you feel might be on the horizon in technology development or research in this area?
Bob Baravarian, DPM:
Right now, we have nails, we have staples, we have screws, and we have anchors. I think plates are in the work and coming, and I truly think that the need for metal fixation will disappear fairly quickly in the next 10 years. There's really no need for it. The amount of reactions to metal that people don't really realize is much more than you think, and the amount of hardware removal and the cost associated with it is much higher than you think. So I think that it's something that is going to change fairly quickly.
Jennifer Spector, DPM:
Well, it's definitely something for us to keep an eye on. And as always, we're very appreciative of your expertise here. Thank you so much for joining us for this additional episode today.
Bob Baravarian, DPM:
I appreciate you. Thank you so much for having me, and thank you for doing this to really progress our profession forward.
Jennifer Spector, DPM:
Well, thank you. We really appreciate that as we do appreciate the audience joining us today too. Make sure, as always, that you're going to podiatrytoday.com, SoundCloud or your favorite podcast platforms to find this and other episodes of Podiatry Today Podcasts. I'm Dr. Jennifer Spector, the Associate Editorial Director for podiatry today, and we hope you'll join us next time.
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Podiatry Today or HMP Global, their employees, and affiliates.