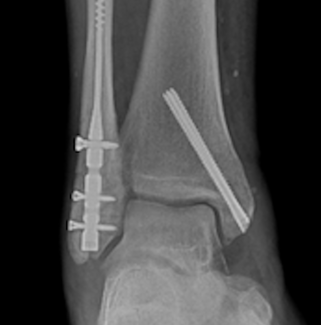
Invisible Barriers in Radiographic Healing
Key Takeaways
1. Healing Depends on More Than the X-Ray
In MIS bunion surgery, important healing variables—soft tissue support, blood supply, fixation stress, and patient health factors—aren’t visible on radiographs. Optimizing outcomes requires looking beyond the bone cut alone.
2. Fixation Matters—But Balance Is Key
Evolving fixation options (from K-wires to screws to radiolucent constructs) influence stability and bone healing. Too rigid or not rigid enough can both create problems, making construct selection critical.
3. Technique Is Advancing—Monitoring Still Requires Judgment
While modern instrumentation has improved reproducibility and shortened the learning curve, postoperative management still relies on careful clinical judgment—knowing what’s normal, when healing is lagging, and how to prevent complications as MIS continues to evolve.
Transcript
What are these invisible variables that maybe we're not seeing on radiographs or with our patients in an MIS bunion and in their healing process? I really think there's a host of them actually, and this is where our future research should probably focus on a lot of that stuff. Such things as just the soft tissues in general. We've done a couple studies to look at that, what exactly is happening with the soft tissues and holding it together. That's not necessarily something you see on plain film radiographs. And so that's one component. I think the blood supply coming into the osseous structure that you're looking at that's trying to heal. Again, not really a great test to look at that or to see it on an X-ray. How about the effect of your fixation construct, whether you're using one or two screws to fixate that first metatarsal.
These things do have an effect on the stress that gets placed on the metatarsal bone, and that can affect on the patient's behalf, how their bone then goes on to heal. And then there's a host of other just patient characteristics. What's their medical status, their age? Do they use tobacco or not? Are they on some medications that might affect their healing? What's their nutritional status? Are they osteoporotic? So these are some of the components we have to all put together when you're monitoring these patients in the postoperative period or even when you're trying to optimize them preoperatively before the procedure.
I think all those factors I mentioned, you must combine it with your fixation construct and these are all going to have some kind of effect on your patient's healing. And the fixation has evolved over time. That's been well documented in the literature. We've gone from no fixation to K-wires to now screws, and even the current screws we have, I mean most companies have a beveled head type screw that we use for these MIS bunion procedures, and now you're starting to see people start to maybe even play around with radiolucent fixation, which also allows you to see the bone a little bit better and kind of monitor that bone as it's healing and filling in over time. So I think it's another area in the future to kind of look at. And then again, there's probably an effect on how rigid your construct is or how non rigid it is.
If it's too rigid, it may not be getting enough stress to produce the bone that's necessary to heal these metatarsal osteotomies. Whereas if it's not rigid enough, then your patient could be at risk for certain complications such as a fracture or suboptimal outcomes. And so these are all factors we got to consider when doing these procedures. I don't think, I guess the advancement in surgical materials has really affected how we follow them. I would say I'm still following them very similar to when I first started this stuff, but I would say what those surgical materials have really done is made these procedures just more reproducible intraoperatively and hopefully it has cut down the learning curve for new MIS users or maybe folks that are trying to get into these types of procedures, which certainly has an effect on the backend for your patient. If you're comfortable with the able to reproduce it, it's safe. You're able to do it efficiently or quick. Your patient's probably not going to have as many complications potentially. So I do think it has really optimized that process, but I don't think it has really changed how we follow them. But maybe as more advancements come on, we will see that type of effect.
Yeah, I think in the postoperative period, it's just what to look for as far as what is normal and what's not. How long do you maybe wait to give these metatarsal osteotomies time to fill in? How do you avoid some of the complications that come with them? And as always, how can we do it better? We're constantly learning about this procedure and trying to make it better, and we do that through experience, but also through research and development. And so I think that's going to be a big takeaway is where are we at now versus maybe even five years ago, and where is it going in the future? And things to look out for people that are interested in getting into these procedures.
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Podiatry Today or HMP Global, their employees, and affiliates.