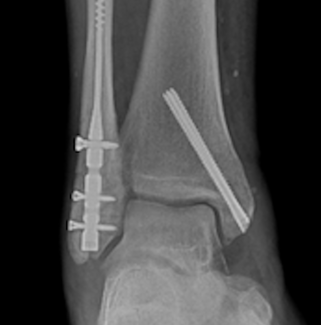
Alternative Lesser Metatarsal Osteotomies: Expanding Your Toolkit
This article explores when and why metatarsal osteotomies other than the Weil may offer useful alternatives for deformity-driven correction. By matching osteotomy selection to underlying biomechanics, the authors share how surgeons can optimize alignment, preserve joint stability, and reduce postoperative complications.
Key Takeaways
• The Weil osteotomy remains effective—but not universal.
Although highly reliable in some scenarios, the Weil osteotomy may be less than ideal for certain deformities, where alternative osteotomies may be preferred to reduce potential complications such as the floating toe.
• Dorsal chevron osteotomy offers stable, in-line shortening with joint preservation.
For isolated parabola disruption with minimal digital deviation, the dorsal chevron provides stable axial decompression, preserves the MTPJ, and allows early weigh-tbearing without symptomatic floating toe.
• Oblique metatarsal osteotomy enables powerful multiplanar correction.
For crossover toes, windswept deformity, or MTPJ subluxation, the oblique osteotomy enables simultaneous shortening and transverse translation to restore tendon balance and MTPJ alignment.
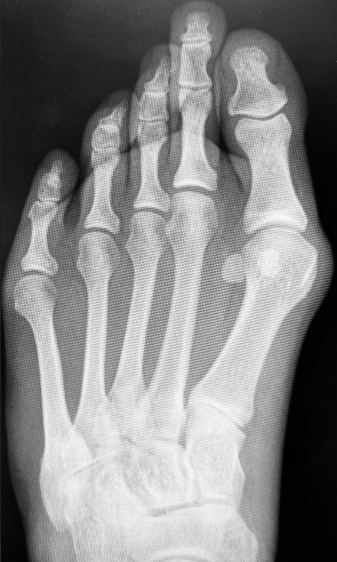
The Weil osteotomy remains the most widely used technique for surgical management of metatarsalgia and is often considered the procedure of choice for this condition. Dr. Lowell Weil, DPM, FACFAS, described an osteotomy oriented parallel to the weight-bearing surface of the metatarsal, which allows controlled proximal translation of the capital fragment to achieve axial decompression.1 Surgeons can perform the procedure with or without fixation and with consistent demonstration of favorable outcomes.2
Although reports of floating toe are common as a radiographic consequence of the Weil osteotomy, its clinical significance is often limited, with multiple studies demonstrating that most floating toes are not painful and do not affect patient satisfaction or function.3,4 Nonetheless, high reported incidence rates—Wagner and colleagues noted 57% at ≥4 years5, and Hofstaetter and team reported 68% at 84 months6—have led many surgeons to explore alternative osteotomies, particularly in cases with digital deformity or multiplanar imbalance.
The Weil osteotomy remains particularly effective for metatarsalgia resulting from an elongated lesser metatarsal or “third-rocker metatarsalgia,” a biomechanical concept described by Perry.7 However, in patients with concurrent transverse- or sagittal-plane deformity, alternative osteotomies may better address the underlying mechanics. In our practice, two such options—the dorsal chevron osteotomy and the oblique metatarsal osteotomy—have provided reliable, reproducible correction with no observed cases of symptomatic floating toe.
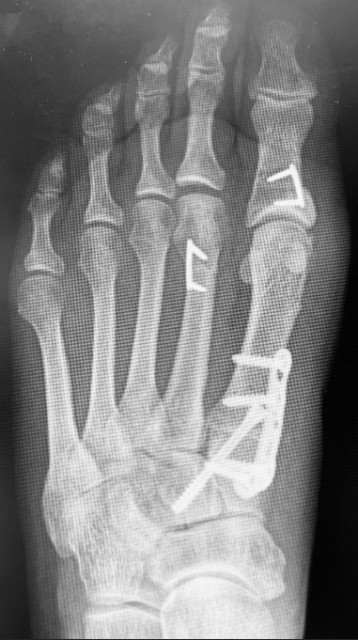
Considerations When Selecting an Osteotomy
When determining the most appropriate osteotomy, we consider several clinical factors:
• Amount of shortening required
• Presence of transverse-plane deviation or digital overlap
• Metatarsal declination and sagittal-plane abnormalities or other global foot deformities (eg, cavus foot type, metatarsus adductus, etc.)
• Need to preserve MTPJ stability
• Risk of floating toe or dorsal stiffness
The following sections describe the operative technique and rationale for the distal chevron and oblique osteotomies.
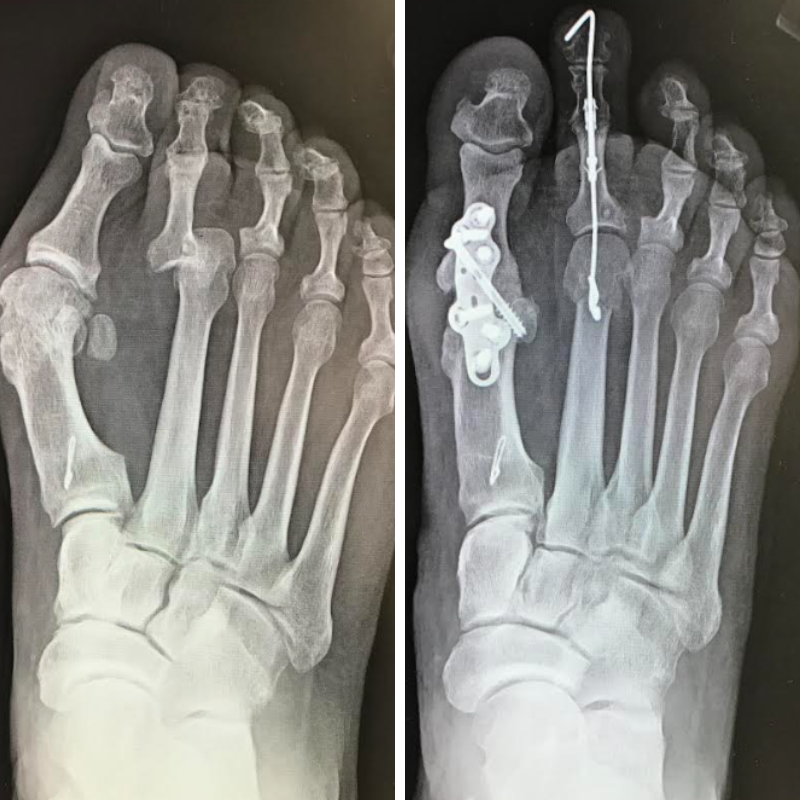
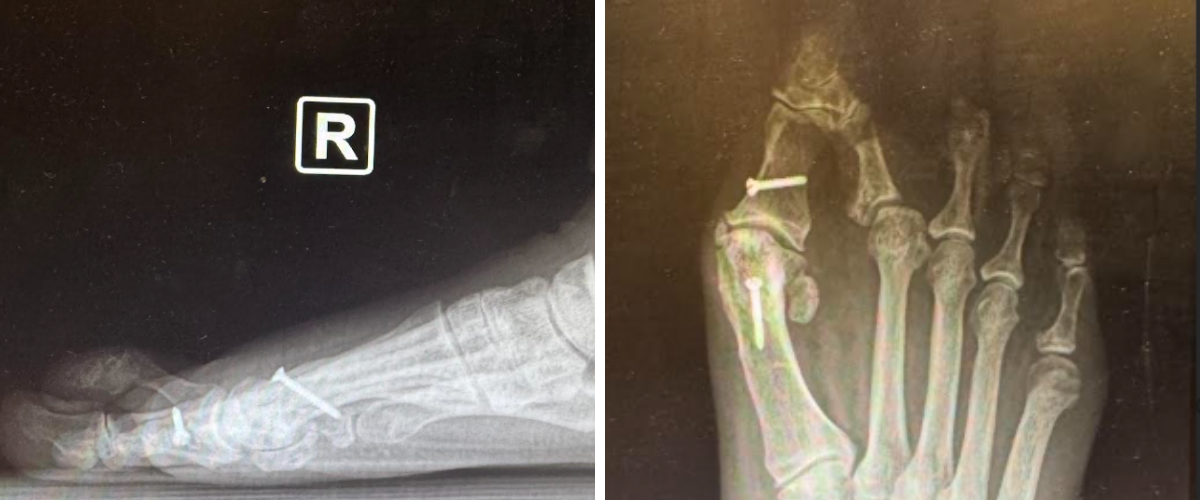
Dorsal Chevron Osteotomy/Jacoby Osteotomy
The dorsal chevron osteotomy is our preferred technique in patients whose primary pathology is metatarsal parabola disruption, with minimal digital deviation. Its V-shaped geometry provides intrinsic transverse-plane stability, and because the osteotomy takes place in the metatarsal neck, the MTPJ capsule can largely remain intact—limiting soft-tissue morbidity.
Surgical Technique. The surgeon makes a longitudinal incision over the target metatarsal, or between rays if addressing multiple metatarsals. Retraction of the extensor tendon is next, as lengthening only occurs when necessary to correct deformity. Dissection proceeds to the periosteum while maintaining capsular integrity.
Using a small precision sagittal saw blade, one plans the chevron osteotomy >4 mm proximal to the dorsal capsule/articular surface. The orientation of the osteotomy must accommodate planned fixation, as one must have adequate space far enough away from the articular surface for the placement of the distal dorsal staple arm. Creation of the medial and lateral wings takes place perpendicular to the metatarsal shaft, converging centrally in the neck.
Once the surgeon mobilizes the capital fragment, they can achieve controlled shortening by resecting a parallel wedge proximally. Fluoroscopy can confirm metatarsal length; we recommend incremental bone removal to the desired amount of shortening.
Fixation typically consists of a single 10-mm dorsal staple. The chevron geometry provides transverse plane stability, while the staple offers reliable sagittal plane control. In our experience, this combination has prevented floating toe and dorsal stiffness and has allowed early weightbearing in a surgical shoe.
Indications
• Parabola disruption requiring precise in-line shortening
• Minimal transverse-plane digital deformity
• Desire to preserve MTPJ soft tissues
• Need for a stable construct that tolerates early weightbearing
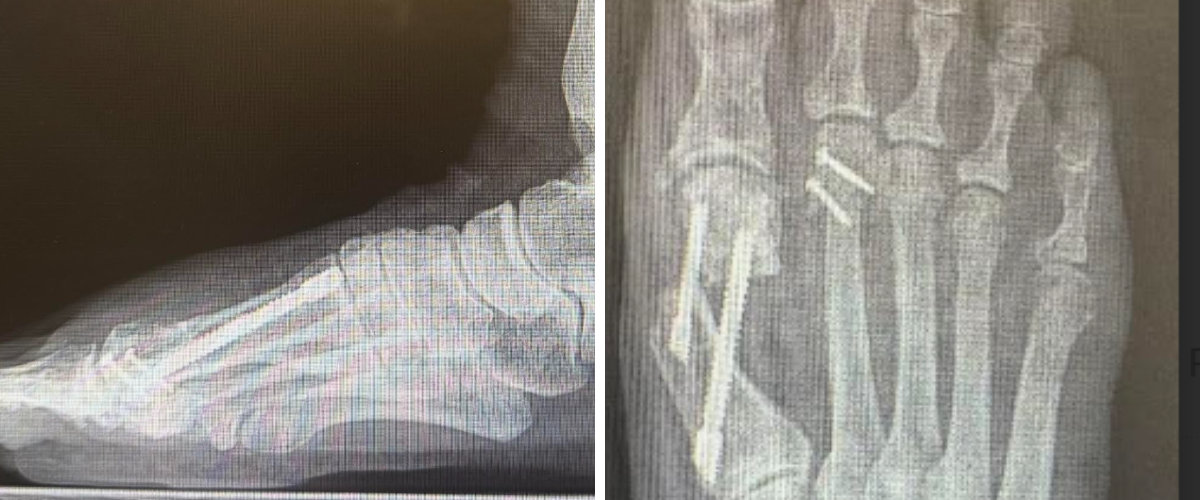
Oblique Metatarsal Osteotomy
For patients with transverse-plane deformity—including crossover toes, digital overlap, or windswept deformities—we prefer an oblique style osteotomy. This technique enables simultaneous shortening and medial or lateral translation of the metatarsal head, thereby improving tendon balance and MTPJ alignment.
Surgical Technique. We perform a linear capsulotomy, exposing the metatarsal head and neck. Transection of the lateral collateral ligaments facilitates reduction of the capital fragment. We avoid using a McGlamry elevator to protect the articular cartilage. Retractors placed around the metatarsal assist with controlled exposure.7
For medial translations (eg, medial crossover second toe), the osteotomy begins at the lateral aspect of the metatarsal head just proximal to the articular surface and exits proximal at the medial cortex in an oblique fashion. For lateral translations (eg, windswept toe deformity), the osteotomy begins at the medial aspect of the metatarsal head just proximal to the articular surface and exits proximally at the lateral cortex in an oblique fashion.
After freeing the capital fragment, shortening can take place as needed, and the surgeon can adjust the sagittal plane position by plantarflexing or dorsiflexing the head. Frequent fluoroscopic evaluation helps confirm correction and alignment. As the capital fragment naturally translates proximally, it realigns the metatarsal phalangeal joint, reducing the tendon imbalance which can cause toe deformity. Fixation uses two snap-off screws placed perpendicular to the osteotomy. The surgeon should remodeling the distal metatarsal to eliminate any step-off distally. Soft tissue balancing and hammertoe correction can then take place as indicated, adding temporary MTPJ pinning if desired to enhance postoperative stability.
Indications
• Transverse-plane deformity requiring metatarsal head translation
• Digital overlap or MTPJ subluxation
• Combined deformity involving sagittal and transverse components
• Need for a forgiving osteotomy that permits fine-tuning of shortening and alignment
In Conclusion
The Weil osteotomy has been considered the most effective technique for metatarsal shortening in the treatment of metatarsalgia for greater than 30 years. However, alternative osteotomies provide valuable solutions for specific deformity patterns and may mitigate risks such as floating toe.
The dorsal chevron osteotomy offers controlled axial decompression, inherent transverse-plane stability, early weightbearing, and preservation of the MTPJ capsule—features that have contributed to our absence of floating toe in this cohort.
The oblique metatarsal osteotomy provides the versatility of simultaneous shortening and transverse-plane correction, making it ideal for deformities involving digital overlap, windswept toes, or combined MTPJ instability.
By incorporating these alternative osteotomies, surgeons can employ a more individualized, deformity-specific approach, improving overall alignment, function, and postoperative outcomes.
Dr. Dunn is the Fellowship Director at University of Michigan Health—Sparrow Orthopedics in Lansing, MI.
Dr. Garvin is a Fellow at the Michigan Advanced Foot and Ankle Reconstructive Surgery Fellowship. Lansing, MI.
References
- Monteagudo M, Maceira E. Evolution of the Weil osteotomy. Foot Ankle Clin. 2019;24(4):599-614.
- Boss A, Herrmann E, Gramlich Y, Klug A, Neun O, Manegold S, et al. The conventional Weil osteotomy does not require screw fixation. J Clin Med. 2023;12(2):428.
- Bougiouklis D, Tyllianakis M, Deligianni D, Panagiotopoulos E. Comparison of the Weil and triple Weil osteotomies: a clinical retrospective study. Cureus. 2022;14(2):e22220.
- Wagner E, O’Connell LA, Radkievich R, Caicedo N, Mococain P, Wagner P. Incidence and functional significance of floating toe after Weil osteotomy. Foot Ankle Orthop. 2019;4(4):2473011419891956.
- Hofstaetter SG, Hofstaetter JG, Petroutsas JA, Gruber F, Ritschl P, Trnka HJ. The Weil osteotomy: a seven-year follow-up. J Bone Joint Surg Br. 2005;87(11):1507-11.
- Perry J. Gait Analysis: Normal and Pathologic Function. Thorofare, NJ: SLACK Inc.; 1992.
- Barouk P, Dias M. Lateral metatarsal osteotomy. Orthop Traumatol Surg Res. 2024;110(1S):103782.
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Podiatry Today or HMP Global, their employees, and affiliates.