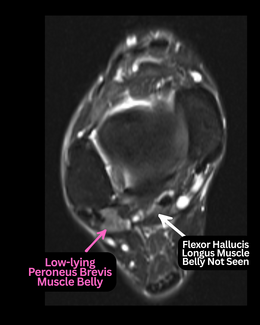
Biologics in Foot and Ankle Pathology
Key Takeaways
1. Biologics function as a toolkit, not a single solution.
PRP, bone marrow aspirate, amniotic products, exosomes, and peptides each have distinct roles. Strategic selection — and sometimes combination — is key to optimizing healing outcomes.
2. Many chronic conditions need stimulation, not suppression.
In tendinopathy and fasciopathy, the goal is often to re-initiate a controlled inflammatory response to “flip” chronic pathology back into an active healing phase.
3. Regenerative medicine is expanding — transparency matters.
While many therapies are used off-label, proper patient consent and education are essential as biologics and peptides become more integrated into podiatric practice.
Transcript
Jennifer Spector, DPM:
Welcome back everybody to Podiatry Today Podcasts, where we bring you the latest in foot and ankle medicine and surgery from leaders in the field. Today, we're so excited to have Dr. Bob Baravarian with us. He's board certified in foot surgery and reconstructive rear foot and ankle surgery, and he's a fellow of the American College of Foot and Ankle Surgeons. He's the co-director of University Foot and Ankle Institute and an Assistant Clinical Professor at the UCLA School of Medicine. He's also a member of our Podiatry Today Editorial Advisory Board. And today we're going to start out a series of conversations with him, this first one being on biologics for foot and ankle ailments, and we're super excited to hear what he has to say. I'm Dr. Jennifer Spector, the Associate Editorial Director for Podiatry Today, and welcome Dr. Baravarian.
Bob Baravarian, DPM:
It sounds like I know what I'm talking about, but I think a lot of what I've learned, I've learned from Podiatry Today, so it's really a pleasure to be here with you.
Jennifer Spector, DPM:
Oh, well, we're super excited to hear about your knowledge on this topic.
Bob Baravarian, DPM:
Thank you.
Jennifer Spector, DPM:
Giving a little bit of background, I think it's a great place to start. We hear a lot about regenerative medicine options, such as PRP, exosome therapies, amniotic tissue products. Could you briefly define a few of those that you are most excited about these days and a little bit about what their clinical intent is for foot and ankle conditions?
Bob Baravarian, DPM:
Yeah, so I think that the excitement is really the entire field. I don't think it's really one thing because I think that what happens is a lot of people will be like, "Well, I'm going to start doing PRP." And it's wonderful. Doing anything is better than not doing anything, but I think that each of these have categorical places where they are better and sometimes we'll combine them together. Sometimes we'll do one, it's not working, we'll do another. So I think having a full toolkit is where you're going to have the best result. I think this field as a whole is the future of medicine. And the grappling with it is some of these products are not FDA approved. Of course, as a physician, you're allowed to use them as long as you're telling your patient that the product is not FDA approved and it's an off-label use.
But the question is, why is it not FDA-approved? And it really comes down to probably bureaucracy more than the products because these products have been around forever. Even your own blood is not FDA-approved, which makes no sense. But I think that this stuff is going to become more and more and more mainstream over the course of the next couple of years.
Jennifer Spector, DPM:
Well, that's great. Could you tell us a little bit about a couple of different options where you feel there's good evidence that these can be used for things like tendon injuries or plantar fasciitis?
Bob Baravarian, DPM:
Yeah. So I think that the main places where I use these products a lot are the Achilles tendon, any tendon, basically. So posterior tibial tendon is common, perineal tendon's common. And then plantar fascia is common, plantar plate is common, and then arthritic conditions, midfoot arthritis, big toe arthritis, ankle arthritis, all common areas where we use it. I also use these products in surgery. So we use these intraoperatively to augment surgery and augment surgery healing for a lot of our patients.
Jennifer Spector, DPM:
So let's start out with one of these options. Where do you find yourself using bone marrow aspirate in this realm?
Bob Baravarian, DPM:
So I think bone marrow aspirate is best intraoperatively. So anytime I'm doing a fusion procedure, whether it's a lapidus, first MPJ fusion, an ankle fusion, midfoot fusion, I find that with fusion procedures, a bone aspirate is a no-brainer. What you're doing is taking mesenchymal cells, concentrating them. And although you're not differentiating them to say, "Hey, become bone." When you take a cell and you put it into its environment, it will adapt to that environment. So we're able to basically just concentrate the mesenchymal cells, put it into the environment of the fusion. And my rate of fusion has pretty much been close to a hundred percent with using the bone aspirate. And we usually will take it either from the calcaneus with a small lateral incision or from the anterior tibia if I'm doing calcaneal work, but usually I just take it from the lateral calcaneus.
Jennifer Spector, DPM:
That's really interesting. And what about PRP? Where are you finding that being most applicable?
Bob Baravarian, DPM:
So PRP, I like to think of as a inflammatory material that also will place cells that are helping to heal an area. So PRP is wonderful in an area where you have a fasciopathy, a tendinopathy. It has been used somewhat in arthritic conditions where in the knee there's been research showing PRP injections helping to reduce arthritic pain, but I actually think that PRP is much better for fasciopathies and tendinopathies. What you're doing in this case is you have a chronic condition where it's a non-inflammatory part of the cycle, usually three to six months out, and the body is non-responsive to the damaged area. So what you're trying to do is put cells in and create inflammation to have your body respond and help heal the tissue.
Jennifer Spector, DPM:
It seems like a lot of these options are designed to sort of break inflammatory cycles and bring you back to that acute phase of healing.
Bob Baravarian, DPM:
I think that the idea of breaking inflammatory cycles is something that we're taught that probably is not the exact answer. You are actually, in many of these cases, increasing the inflammatory cycle to help with healing. So if you think of when you have an injury, you have inflammation. Inflammation is the rush of blood to the area to help heal the tissue. And when you end up in anopathy, fasciopathy, tendinopathy, your inflammatory response has been degraded or reduced. The body will not constantly send blood to an area for an extended period of time. So what we're trying to do is augment the cells in the area, but also increase the inflammatory process to bring the body back to the injured site, and hopefully under controlled circumstances help it heal.
Jennifer Spector, DPM:
That's a great way of putting it. What about amniotic products? Where do you see them falling in this area?
Bob Baravarian, DPM:
So amniotic products are a little bigger category because you can use amniotic membrane, you can use amniotic scaffold, you can use amniotic fluid. The one that I like to use the most is called Wharton's Jelly, W-H-A-R-T-O-N, Wharton's Jelly. And I like it because not only does it give you a lattice work, it also has stem cell quality to it and it has some anti-inflammatory qualities to it. So I use amniotic injections in fasciopathy, tendinopathy, arthritic conditions, inflammatory conditions, almost anywhere you can use the product. The other thing is that several of the amniotic materials have been shown to be helpful to decrease scar tissue and decrease stiffness or scar formation. So I use a lot of amniotic injections post-surgery at the time of surgery to help with soft tissue healing and to try to help with decreasing scar tissue in joints.
Jennifer Spector, DPM:
So something else I've heard people talking about lately that I would love to hear your take on its role in the biologic space is exosomes. What can you tell us about that?
Bob Baravarian, DPM:
Exosomes are somewhat kind of related to the same amniotic material, but they are more at a cellular level than the amniotic material. Exosomes seem to have a larger reaction, meaning they actually have a larger impulse of the body's own reaction to healing. Exosomes are also used IV in many cases. So you can do whole body treatments or you can actually do any partial injection locally augmented with a IV treatment to get more of a full body response. Exosomes are in their infant stage compared to amnio and PRP and bone aspirate, but exosomes are significantly stronger in the response and healing potential compared to PRP and amnio. Where we use exosomes a lot is when we find that, let's say amnio hasn't done enough and we want to get a little bigger boost, we sometimes will switch to an exosome for a little bigger response, a little bit more of the body responding.
And sometimes we'll actually do a combination of injection locally and IV exosomes to get a larger boost for the repair. But exosomes are basically another portion of the umbilical material that helps with healing.
Jennifer Spector, DPM:
And what about therapeutic peptides? That's another sort of hot topic that we're hearing more about.
Bob Baravarian, DPM:
Therapeutic peptides are my favorite. This is like the holy grail of medicine, and I've gone down that rabbit hole really, really far. There's 400 peptides, maybe more, that are available. And just to give you an idea, peptides, insulin is a peptide. The GLP or medications, the medications for weight loss, their GLP stands for glucagon-like peptide. And peptides are able to treat almost anything. Hair loss, collagen loss, tendon, ligament, inflammatory conditions, muscle rebuilding, gut health, you name it, there's a peptide for it. The peptides that we use the most are orthopedic peptides. And there is a few that I highly recommend people learning about. The probably biggest workhorse is BPC157, which is a gut peptide. It helps with gut lining. It can help with arterial lining healing, but it also has been shown to help with tendon, ligament, cartilage, and bone healing. BPC157 often is combined with a second peptide called TB500.
The combination is called wolverine. And that combination just augments BPC157 to be even stronger and the TB500 helps BPC work even better. Then a third peptide that sometimes is added called GHK-CU, which is a collagen peptide. It's often used for healing of plumping the face and collagen production. But as we all know, collagen is a significant portion of orthopedic issues. So GHK can be added and that becomes known as glow. And then a fourth peptide called KPV can be added, which is just a very strong anti-inflammatory peptide, and that becomes known as klow, K-L-O-W. Those wolverine glow and klow are kind of 90% of what we use. There's a peptide that's been shown to be really wonderful for neuropathy nerve problems called ARA-290, which we use often. And then it becomes, okay, what else does the patient need for assistance with healing? There's some peptides that can be used for muscle rebuilding in cases where patients have been off their feet for extended periods of time, and they're not like testosterone or any of these kinds of things.
They're just tell the body to heal itself. But there's pretty much a peptide for everything. And again, peptides are not FDA approved. I think the main reason is because pharmaceutical companies cannot patent a peptide, which is not to their favor. But I do think that this year you're going to start to see a significant number of peptides becoming FDA approved by the administration because there's tons and tons of research out there showing wonderful results with it. But peptides are something that I think are even stronger in assisting podiatric surgeons with good outcomes, wound care, orthopedic trauma, arthritic conditions, inflammatory conditions. I think they're even probably stronger than the biologics. But again, the whole idea is to combine these together to make the optimal situation for healing.
Jennifer Spector, DPM:
I really do appreciate what you mentioned about being aware of the current regulatory status and potential evolution of that potentially coming up so that docs can be aware of where it is and can be transparent with patients about off-label usage when applicable. But it occurs to me that it might be great for us to learn a little bit about your setup. How are you using these things in your practice and in what combinations to learn a little bit more from a practical perspective?
Bob Baravarian, DPM:
Yeah. So I think that it's important for doctors to realize that if something is not FDA approved, it doesn't mean that it's not safe. Regulatory issues are such a complicated issue, but first of all, amniotic injections and amniotic material has been used for 50, 60 years. The way I first learned about it was probably 15 years ago when my buddy was using it for ophthalmology cases to prevent scar tissue after corneal transplants. And you in your office are probably using amniotic membranes for diabetic wounds. So why is it that you feel like it's okay to use it for a diabetic wound, but it's not okay to inject it when it's the same material? So I think that you need to open your vision and open your thoughts to what is good for your patient and realize that as long as you consent people properly and let them know that this is for off-label use, it's not FDA approved, as long as you have consent, there's no reason you can't use this products.
I mean, amniotic injections are used like crazy. How I use it, I tend to feel like you need to make sure that you give your patients their choices and try to make your outcomes be as good as they can be without making decisions for patients. And I think that we as physicians sometimes are like, "Well, it's expensive," or, "I don't know if my patient wants it, " but you're making a decision for them instead of letting them be involved in the decision-making for their care. I use amniotic injections a lot intraoperatively for wound healing and scar tissue prevention. I use PRP a lot intraoperatively in tendon repairs, fascia cases. I use bone aspirate intraoperatively a lot in fusion cases, and sometimes I'll use bone aspirate and amnio. I use peptides, which I start preoperatively and have the patients continue to take the peptides postoperatively to help with healing.
And then in the office, I use a combination of amnio and PRP very commonly in cases that are prolonged non-healing. So I see a lot of patients who've been to two, three doctors, they come in with chronic conditions and I need to flip the chronic to acute. And so we use a lot of amnio, a lot of PRP, sometimes combined with shockwave to try to stimulate the body to start to heal itself. But I think the biggest piece of advice I would give to physicians regarding their patients is one, make sure you consent them properly. And two, this is the future of medicine, not giving patients prescriptions for NSAIDs and giving them prescriptions for gabapentin. If you can do something that is going to allow the body to heal itself without just medicating patients, it behooves you to actually learn about it because your patients are looking for it.
And if you're not providing it, they're going somewhere else. I can tell you that for sure.
Jennifer Spector, DPM:
Will, what else would you like the audience to know about some of these biologics pathways? Is there anything else that you hope that they take home from the conversation?
Bob Baravarian, DPM:
I mean, listen, I'm always available. I love educating people. If it's something where you have questions, please just reach out to me. My email is Dr.bob@docsdocsfootankle.com. I'm more than happy to answer questions for you. I really think that what I've started to notice is that people are coming into our office and saying, "I've seen Dr. Jones and Dr. Smith, and I'm not getting better. And I don't know why they're not offering me amnio or offering me PRP, but I know you do it, so I'm coming here." I think that we need to really start to think broader about what we offer our patients because patients are super educated these days and they're learning about their condition and learning about their options. And so you really need to also become educated and be able to service your patient better.
Jennifer Spector, DPM:
No, definitely. Patient outcomes and new science should be at the forefront of what we're all thinking about. And thank you for sharing your experience on these items with us today. We can't wait to have you back to talk about our next topic, so we'll be looking out for that really soon, but thank you also to our audience for joining us today for this episode of Podiatry Today Podcasts. You can find us on podiatrytoday.com on SoundCloud, Apple Podcasts, Spotify, and your favorite podcast platforms. Dr. Baravarian, we hope you'll join us again next time right along with our audience.
Bob Baravarian, DPM:
Thank you for having me. I truly appreciate it.
Jennifer Spector, DPM:
Absolutely. Thanks to all and have a wonderful day.
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Podiatry Today or HMP Global, their employees, and affiliates.