The Landscape of Skin and Wounds: Exploring the Role of the Microbiome in Podiatric Health and Chronic Wound Healing
From pathogenic colonization to probiotic potential, this article reviews the skin-gut axis as it applies to chronic wound care. Learn more from this review about how the microbiome can influence wound healing—and what this means for the future of clinical care.
Key Takeaways
1. Microbiome balance—not just bacterial presence—drives wound outcomes. Chronic wounds are characterized by dysbiosis, with pathogenic, biofilm-forming organisms disrupting healing, while protective commensals are diminished. Understanding and managing this microbial imbalance is essential to improving wound healing and reducing persistent inflammation.
2. The skin–gut axis expands wound care beyond the wound bed. Emerging evidence shows that gut microbiome composition, influenced by diet and lifestyle, is closely linked to skin health and immune response. Dysregulation in the gut may contribute to chronic skin inflammation and impaired wound healing, positioning nutrition and systemic microbial health as important adjuncts in podiatric and wound care management.
3. Probiotics represent a promising adjunctive therapy in wound healing. Both topical and systemic probiotics demonstrate the ability to modulate inflammation, inhibit pathogenic biofilms, enhance re-epithelialization, and promote tissue repair. While much of the strongest evidence comes from animal and surgical wound models, these findings support continued research into probiotic-based strategies—particularly in the context of antibiotic resistance and chronic wound care.
Microorganisms are infinite in number, and they are an intricate necessity for homeostasis. Humans and microorganisms have evolved together, establishing a symbiotic relationship that underpins all known microbiomes today. One of the most well-known microbiomes is the gut flora. The bacteria in the gut have been shown to help regulate the immune system, provide nutrition, and cause dysregulation that can result in a host of inflammatory diseases, such as irritable bowel syndrome (IBS) and Crohn’s disease.1-4
This can significantly impact podiatric patients, since there is a link among the microbiome, autoimmune diseases, and wound care. Many such patients also contend with chronic diseases and their sequelae, including impaired healing, depression, and reduced quality-of-life.5-7 Although the relationships of these conditions with the natural microorganism world do not remain fully understood, the presence of bacteria in humans can yield both beneficial and harmful outcomes. The objective of the article is to review insights from current literature on microbiome in the context of wound healing.
Skin Flora in Wounds
The skin is home to its own unique microbiome, which is important in skin structure integrity. Skin sites are generically categorized into different microenvironments including moist, dry, and sebaceous. Common skin flora microbes exhibit distinct microbial signatures unique to each individual person’s flora. Hands, for example, harbor a diverse array of easily transmittable microbes. Additionally, the skin microbiota is easily influenced by immediate external forces (skin contact transfer) and may, therefore, be less understood than internal gut forces which involve multiple factors including chemical interactions, diet, and lifestyle.8 Research shows that age and handedness can change a patient’s microbiome.8
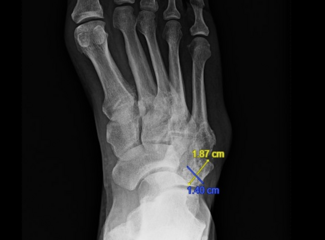
Chronic wounds have biofilms which often contain coaggregated bacterial species that promote organism persistence and impede healing. A 2011 quorum sensing study published in Wound Repair and Regeneration analyzed 15 wound swab samples from patients with chronic wounds located at the sacrum, the coccyx, or the feet. The researchers then compared bacterial diversity to samples from normal skin. Employing pyrosequencing, they identified an average of 17 genera of bacteria in each wound. Notably, they found increased numbers of anaerobes, gram-negative rods, and gram-positive cocci in the chronic wounds compared to intact skin.9 Specifically, commonly cited bacterial families found in chronic wounds include Staphylococcus, Streptococcus, and Pseudomonas, which cause skin destruction and necrosis through exotoxins that disrupt benign skin flora and cellular metabolism.9
Unlike the destructive bacteria mentioned above, the Actinobacterium family is one that is in fewer numbers in chronic wounds, the same study suggested therefore that Propionibacterium may therefore act as a benign colonizer with protective effects against biofilm formation.9
These findings, however, underscore the complex interplay among bacterial species in chronic wounds, particularly the detrimental impact of certain pathogenic organisms on skin integrity. In this context, it is essential to consider the role of multispecies biofilms, which act as antagonists to protective species, thrive in moist, adherent skin environments, and are embedded in the exopolysaccharide matrix. Chronic wounds, with their persistently moist conditions, provide ideal environments for biofilm formation. Biofilms are produced through bacterial communication via quorum sensoring molecules, which regulate expression of virulence factors. They are composed of approximately 15% bacterial cells and 85% of matrix, offering protective barriers that promote bacterial persistence and resistance.9
Evaluating the multispecies census in a biofilm and comparing them to another biofilm of a “control” healthy tissue bed shows that chronic wounds are also associated with increased bacterial load and increased inflammatory responses.9
For instance, a 2014 review by Christensen and Brüggermann further reinforces the significance of commensal bacteria such as P. acnes, which possess both protective and potentially harmful properties.10 They further posit that there are other protective agents in the microbiota. S. epidermidis is determined as the species that would most successfully colonize due to mutualistic lifestyle, low cytotoxicity, and ability to evade host defenses, causing a low host immune response. Referred to as a mutual nonaggression pact, the bacteria are able to persist beyond the aggressive host-damaging properties.10 It is likely that the pathogen developed in a long-term co-evolutionary history with the human skin serving as the host. This idea, however, becomes complicated, as the authors above also shared that these organisms contribute to mutualistic properties and parasitic properties as the genus P. acnes acts not only as a chimeric species with probiotic potentials, but also as one that has the potential to secrete degrading hemolytic enzymes.10
What Role Does the Gut Play?
While the skin is often the first line of defense against harmful microorganisms, the gut plays an equally crucial role in maintaining overall health of the human body. The microbiota of the skin includes bacteria that interacts with the immune system and external factors. The gut microbiota serves as a diverse ecosystem, which is thought to influence digestion. Some research suggests a connection between the skin and gut microbiome, indicating that imbalances in one may potentially influence the other.
The skin-gut axis refers to the bidirectional communication between the skin and the gut. Research shows that an imbalance in the gut microbiome can be associated with skin conditions such as acne, eczema, and psoriasis. In turn, skin inflammation may also affect gut health.11 The connection demonstrates how microbial ecosystem of the human body are closely linked to the immune responses of the gut. Thus, understanding the skin-gut axis can help treat skin disorders by addressing gut health.
Moreover, enhancing knowledge on microbial dynamics is essential, especially in terms of physical interactions such as those encountered in healthcare settings or through food handling as these serve as conduits for the gut-skin axis. It is understood that influences on the gut microbiome are through dietary and lifestyle factors, although research suggests that the interaction between the skin microbiota and its gut counterpart may be more intimate than previously believed to be key in order to maintain a healthy skin flora.
A 2021 German cross-sectional study published in the British Journal of Dermatology attempts to bridge the gap between diet lifestyle and skin patterns.11 Skin samples (a total of 1794) were obtained from 647 participants in 2 population-based German cohorts. A 16S ribosomal RNA gene sequencing on these samples were observed to establish any potential patterns. The researchers found that beta diversity and amplicon-sequenced genes linked to lifestyle factors. The study reinforces the protective findings of the genus P. acnes and finds them associated with the least amplicon sequence variants (ASVs).11
These ASVs are utilized to analyze the association between dietary intake of macronutrients and bacteria. Macronutrients of dietary intake, carbohydrates, fat, fiber, and protein, are evaluated. It is discovered that, with respect to dietary energy, fat and fiber were associated in both positive and negative directions with different Corynebacterium and Staphylococcus variants. Protein intake is positively associated with two Corynebacterium and two Staphylococcus variants, including S. hominis.11
Probiotics
While many are familiar with the purpose of antibiotics to eliminate harmful bacteria, there is a lesser-known objective of probiotics to impact wound healing such as infected cutaneous wounds and intestinal ulcers. Probiotics are live microorganisms that contribute diversity or replenishment to bacteria in the human body. They can be taken through various delivery methods, including oral, topical, and intranasal routes, and provide various different protective processes and health benefits. They can also induce fibroblasts, promote epithelial cell migration, displace or eliminate certain pathogens, and reinforce the epithelial barrier.12 Probiotics thus hold new, promising therapeutic potentials for the wound healing process, especially in the context of antibiotic resistance.
The first phase of wound healing involves inflammation, identified by an influx of inflammatory cells such as leukocytes and macrophages.13 Probiotics act as immunomodulators, interacting with the bacteria and inhibiting signaling factors to prevent spread of infection. The Lactobacillus genus, specifically, has shown a continuous augmentation of leukocytes and attraction of neutrophils and macrophages in the wound site by increasing cytokines, which boosts the inflammatory process and reepithelialization.13
Several studies investigated the impact of topical probiotics on wound healing. A 2021 systematic review found that implementation of probiotics revealed positive outcomes on wound re-epithelialization, neurovascularization, and wound healing without adverse effects. The review examined the effects of probiotics on surgical wound healing, either used alone or in combination with nanotechnology-based techniques.13 Though the review excluded studies involving burns, chronic wounds, and diabetic ulcers, the results on surgical wounds are promising.
One 2020 meta-analysis looked at the addition of topical probiotics to regulate inflammation, prevent infection, and aid healing.14 The researchers reviewed multiple probiotic strains with healing potential across various studies, aiming to develop treatment algorithms based on the effects of these beneficial bacteria on the skin microbiome and cutaneous wound healing.
In animal studies, L. fermentum histologically showed improved healing and increased wound closure in infected wounds. Saccharomyces cerevisiae, also known as Brewer’s yeast, improved wound healing in burns relative to silver sulfadiazine.14 The effects of wound treatment with kefir gel demonstrated improvement in granulation and neurovascularization in wounds compared to those of control wounds treated with saline or neomycin-clobetasol.15 Additionally, a 2012 animal study similarly found a kefir gel promoted advanced healing in burns compared to silver sulfadiazine.14
Another notable probiotic strain is L. plantarum, which improves tissue repair and collagen concentration and decreases bacterial translocation, the severity and the length of infections, mortality, septicemia, blood poisoning by bacteria, and production of inflammatory markers.14 One study in the meta-analysis compares a control group of individuals treated with an ointment and an experimental group of individuals with wounds treated with L. plantarum. The probiotic enhanced keratinocyte migration, cytokines, and chemokines in the immune response, inhibited bacterial growth of S. aureus, reduced bacterial load, and modified inflammation. In a study with infected second- and third-degree burns, the probiotic strain was as effective as silver sulfadiazine in decreasing bacteria load and promoting granulation.14
In two studies, S. thermophilus increased skin ceramides, which are lipids in skin cells that promote skin hydration and strengthen the skin barrier. Additionally, the introduction of probiotics into pathogenic bacterial cultures inhibited biofilm formation by bacteria and fungi by approximately 50%.14 Another probiotic strain, L. bulgaricus, accelerated the healing process of diabetic wounds.16 Both probiotics modulate inflammatory cells at wound sites, with elevated mRNA levels of inflammatory cytokines observed following treatment.
The Blood-Brain Barrier
As the human body harbors both harmless and harmful microbes at various anatomical sites, such as skin and gut, the effects that result may reflect health and disease states of individuals depending on the balance of the host innate immune system and the microbial inhabitants that are vital to normal skin function and wound repair.17-18 For example, wound care can wreak havoc on the healthcare system due to a multitude of perspectives, such as interdisciplinary care, finances, and public health.17 Although associations between mood and cognitive dysfunction with chronic wounds have been explored,19 a further investigation of the relationship between microbiota-gut-brain axis and depression remains unanswered.
Because of increasing research on intestinal flora effects throughout the human body, a plethora of findings on the gut brain axis has emerged. This research illustrates the interaction between the microbiome of the gut and the function of the brain.20 Gut peptides regulate processes such as satiety, feeding behavior, insulin, and glucose secretion and sensitivity, and influence tissue functions.20 The axis has also been profound in the therapeutic interventions for not only gastrointestinal-related conditions but also inflammatory and autoimmune diseases, allergic reactions, and psychiatric disorders.18
Specifically, composition of resident bacteria in the gut has been found to affect the brain and behavior processes, such as cognitive functioning, anxiety-like tendencies, and depression, through direct link of emotional and cognitive centers in association with the central nervous system and enteric nervous system.25 In one model, transferring fecal microbiota-depleted rats caused behavioral and biochemical depressive signs in rats.25 In another model, fecal microbiota composition comparison between that of nondepressed patients and that of depressed patients demonstrated higher levels of Bacteroidetes and lower levels of Faecalibacterium indicate correlation between microbiome and mood.25
The gut brain axis has been found to have endocrine, immune, humoral, metabolic, and neural reciprocal mechanisms through multiple experiments.20-24 However, the brain-skin axis has only recently been recognized as bidirectional.26 Initial descriptions characterized it as a target to the skin via brain neuroimmune signaling. Now, it is thought that the central nervous system affects the skin physiologically, and the skin, in turn, cascades stress signals to the brain via neuroimmunomodulator and catecholamine byproducts.26 Devoting more energy in understanding the skin-brain-axis in relation to cognition may further approaches in those infected with chronic, infected wounds.19
As the skin-brain-axis theory is in its infancy, it does not provide much insight on skin microbiome dysbiosis in relation to psychiatric disorders.18 For a long time, the monoamine hypothesis has been widely accepted as a leading neurobiological mechanism, which claims that molecular changes in central nervous system neurotransmitters go hand in hand with depression.26 Furthermore, like alterations in chemical substances, increased number of inflammatory cytokines systemically also appear in those with major depressive disorder.26 However, one notable study tests the hypothesis to determine whether the skin microbiome dysbiosis is akin to the gut microbiota and its impact on cognition and behavior.22 The study involves studying two groups, non-wounded mice and wounded mice infected with Pseudomonas aeruginosa. The mice perform various tasks that test for anxiety, depression, and memory recall.26 The findings reveal elevated expressions of Nod-like receptors, glucocorticoid receptors, cytokines, increased anxiety, altered cognition, and increased depressive behavior in both groups; however, the wounded group had a higher magnitude across the board.26
While the digestive system and the integumentary system serve distinct roles in the body, recent research highlights an intricate relationship between the microbiome of these systems and brain function.20 The emerging concept of the microbiome skin-brain axis suggests that there is a critical link among skin flora, chronic wound inflammation, and neuropsychiatric health, including the development of mood disorders such as depression.19 As more studies uncover the shared pathways and mechanics among the gut, the skin, and the brain, particularly in the context of wound healing and immune response, the potential for therapeutic interventions targeting both the skin-brain axis and gut-brain axis become increasingly significant.20 Understanding how skin flora in wound beds specifically affects the blood-brain barrier will serve crucial in addressing the bidirectional influence between chronic wounds and mental health. This growing field opens new avenues for improving both physical well-being and mental well-being in patients who have chronic skin conditions.
Concluding Thoughts
The intricate relationship among skin flora, wound healing, and mental health underscores the critical importance of microbiomes in the maintenance of overall health. Chronic wounds experience an impact from both the presence of pathogenic bacteria that hinder healing and an absence of beneficial microbes that play roles in protection and skin integrity. Disruptions in the skin microbiota may influence neuropsychiatric health, linking chronic wound conditions with mood disorders such as depression based on the concept of the microbiome skin-brain axis. As research continues to uncover the complex dynamics involved in the gut, the skin, and the brain microbiomes, there is likely significant potential for developing innovative therapeutic strategies that target these interconnected systems.
 Published in partnership with the American Association for Women Podiatrists.
Published in partnership with the American Association for Women Podiatrists.
Dr. Mutyala is a graduate of Kent State University College of Podiatric Medicine.
Dr. Boussi is chief and third-year resident at UCSF Health: St. Mary’s Medical Center in San Francisco, CA.
Dr. Wagman is a first-year resident at Mount Sinai Medical Center in Miami Beach, FL.
Dr. Elizabeth Ansert is fellowship-trained in diabetic limb salvage and is currently the Medical Director at the Thibodaux Regional Wound Healing and Limb Preservation Center in Thibodaux, LA.
References
1. Korn T, Bettelli E, Oukka M, Kuchroo VK. IL-17 and Th17 cells. Annu Rev Immunol. 2009;27:485–517.
2. Macpherson AJ, Harris NL. Interactions between commensal intestinal bacteria and the immune system. Nat Rev Immunol. 2004;4:478–485.
3. Packey CD, Sartor RB. Interplay of commensal and pathogenic bacteria, genetic mutations, and immunoregulatory defects in the pathogenesis of inflammatory bowel diseases. J Intern Med. 2008;263:597–606.
4. Vernocchi P, Del Chierico F, Putignani L. Gut microbiota metabolism and interaction with food components. Int J Mol Sci. 2020;21(10):3688.
5. Young A, McNaught CE. The physiology of wound healing. Surgery (Oxford). 2011;29(10):475-479.
6. DeJean D, Giacomini M, Vanstone M, Brundisini F. Patient experiences of depression and anxiety with chronic disease: a systematic review and qualitative meta-synthesis. Ont Health Technol Assess Ser. 2013;13(16):1.
7. Megari K. Quality of life in chronic disease patients. Health Psychol Res. 2013;1(3).
8. Kumar KV, et al. Co-aggregation of bacterial flora isolated from the human skin surface. Microb Pathog. 2019;135:103630.
9. Han A, Zenilman J, et al. The importance of a multifaceted approach to characterizing the microbial flora of chronic wounds. Wound Repair Regen. 2011;19(5):532–541.
10. Christensen GJM, Brüggemann H. Bacterial skin commensals and their role as host guardians. Benef Microbes. 2014;5(2):201–215.
11. Moitinho Silva L, et al. Host traits, lifestyle and environment are associated with the human skin bacteria. Br J Dermatol. 2021;185. doi:10.1111/bjd.20072.
12. Lukic J, Chen V, Strahinic I, Begovic J, Lev-Tov H, Davis SC, Tomic-Canic M, Pastar I. Probiotics or pro-healers: the role of beneficial bacteria in tissue repair. Wound Repair Regen. 2017;25(6):912-922.
13. Bekiaridou A, Karlafti E, Oikonomou IM, Ioannidis A, Papavramidis TS. Probiotics and their effect on surgical wound healing: a systematic review and new insights into the role of nanotechnology. Nutrients. 2021;13(12):4265.
14. Knackstedt R, Knackstedt T, Gatherwright J. The role of topical probiotics on wound healing: a review of animal and human studies. Int Wound J. 2020;17:1687–1694.
15. Mohtashami M, Mohamadi M, Azimi-Nezhad M, Saeidi J, Nia FF, Ghasemi A. Lactobacillus bulgaricus and Lactobacillus plantarum improve diabetic wound healing through modulating inflammatory factors. Biotechnol Appl Biochem. 2021;68:1421-1431.
16. Holmes CJ, et al. Dynamic role of host stress responses in modulating the cutaneous microbiome: implications for wound healing and infection. Adv Wound Care. 2015;4(1):24–37.
17. Goswami A, et al. Role of microbes in the pathogenesis of neuropsychiatric disorders. Front Neuroendocrinol. 2021;62:100917.
18. Hadian Y, Fregoso D, Nguyen C, Bagood MD, Dahle SE, Gareau MG, Isseroff RR. Microbiome-skin-brain axis: a novel paradigm for cutaneous wounds. Wound Repair Regen. 2020;28(3):282–292.
19. Arck P, Handjiski B, Hagen E, Pincus M, Bruenahl C, Bienenstock J, Paus R. Is there a 'gut-brain-skin axis'? Exp Dermatol. 2010;19(5):401-405.
20. Shanahan F. Brain-gut axis and mucosal immunity: a perspective on mucosal psychoneuroimmunology. Semin Gastrointest Dis. 1999;10:8–13.
21. Romijn JA, Corssmit EP, Havekes LM, Pijl H. Gut-brain axis. Curr Opin Clin Nutr Metab Care. 2008;11:518–521.
22. Beraza N, Trautwein C. The gut-brain-liver axis: a new option to treat obesity and diabetes? Hepatology. 2008;48:1011–1013.
23. Niess JH, Mönnikes H, Dignass AU, Klapp BF, Arck PC. Influence of stress on immune mediators, neuropeptides and hormones with relevance for inflammatory bowel disease. Digestion. 2002;65:131–140.
24. Hadian Y, Isseroff RR, Gareau M, Fregoso D. 16416 Cutaneous wounds and wound infection affect cognition and behavior in mice. J Am Acad Dermatol. 2020;83(6):AB178.
25. Fregoso DR, Hadian Y, Gallegos AC, Degovics D, Maaga J, Keogh CE, Kletenik I, Gareau MG, Isseroff RR. Skin-brain axis signaling mediates behavioral changes after skin wounding. Brain Behav Immun Health. 2021;15:100279.
26. Rodrigues KL, Caputo LRG, Carvalho JCT, Evangelista J, Schneedorf JM. Antimicrobial and healing activity of kefir and kefiran extract. Int J Antimicrob Agents. 2005;25(5):404-408.
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Podiatry Today or HMP Global, their employees, and affiliates.