Distal Transradial Coronary Procedures in Chronic Versus Acute Coronary Syndromes: Insights From the DISTRACTION Registry
© 2025 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of the Journal of Invasive Cardiology or HMP Global, their employees, and affiliates.
Abstract
Objectives. The benefits of distal (dTRA) over proximal transradial access (pTRA), mainly faster hemostasis and fewer radial artery occlusion, have been highlighted. Nevertheless, data addressing chronic vs acute coronary syndromes peculiarities are lacking; thus this study aimed to assess those differences.
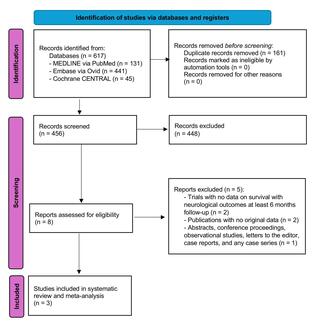
Methods. The authors conducted a retrospective analysis of 6871 consecutive and all-comers patients from a real-world, large-scale registry of routine coronary angiography and/or percutaneous coronary intervention (PCI) via dTRA.
Results. Mean patient ages were 63.8 ± 15.7, 64.8 ± 15.7, and 62.9 ± 16 years for total, chronic, and acute coronary syndromes groups, respectively. In the chronic coronary syndromes group (n = 2,767, 40.3%) there was predominance of hypertension (83.5% vs 72.9%; P < .001), diabetes (46.2% vs 37.4%; P < .001), previous PCI (37.2% vs 20.2%; P < .001) or coronary bypass surgery (4.9% vs 2.7%; P < .001), previous ipsilateral pTRA (13.9% vs 8.5%; P < .001) or dTRA (21.7% vs 8.9%; P < .001) sheath insertion, and ultra-low contrast procedures (66.5% vs 61.2%; P < .001). In the acute coronary syndromes group, there was predominance of male patients (66.9% vs 63.3%; P = .002), smokers (53.9% vs 45.6%; P < .001), total amount of PCI (72.3% vs 48.5%; P < .001), and right dTRA (85.3% vs 70.3%; P < .001). No major adverse events directly related to dTRA were recorded.
Conclusions: When performed by proficient operators, routine coronary procedures via dTRA appear to be safe and feasible in both chronic and acute coronary syndromes, with similar low rates of access-site crossovers and complications.
Introduction
Compared with classic transfemoral access, proximal (conventional) transradial access (pTRA) has been shown to be more cost-effective and associated with fewer access site-related complications, earlier patient ambulation, and greater postprocedural comfort.1 Thus, pTRA is recommended as the standard approach, unless it is overridden by procedural considerations.2,3
Patients with acute coronary syndromes are at higher risk of vascular access-site complications and bleeding.2,3 For this subset of patients, pTRA has shown a significant reduction of vascular complications and stroke in general.4 In addition, in the setting of ST-segment elevation myocardial infarction, pTRA has been associated with lower rates of death.5
Distal transradial access (dTRA), as compared with pTRA, has advantages such as faster hemostasis and lower rates of proximal radial artery occlusion,6-10 the most frequent complication of pTRA.11
Despite the increasing incorporation of dTRA by interventionalists around the world, there is a clear lack of data addressing routine coronary angiography and/or percutaneous coronary intervention (PCI) via dTRA in chronic vs acute coronary syndromes. Thus, we aimed to assess those differences from a real-world, large-scale registry of consecutive and all-comers patients.
Methods
From February 2019 to July 2024, 6871 consecutive patients who underwent coronary angiography and/or PCI via dTRA at Hospital São Paulo, Escola Paulista de Medicina, Universidade Federal de São Paulo in São Paulo, Brazil were enrolled in the DIStal TRAnsradial access as default approach for Coronary angiography and intervenTIONs (DISTRACTION) registry (ensaiosclinicos.gov.br Identifier: RBR-7nzxkm). The presence of any (even weak) palpable pulses at both proximal and distal radial arteries was the eligibility criterion for enrollment. Of note, patients with unstable hemodynamic conditions were not excluded. The study was approved by the Research Ethics Committee, Hospital Universitário I, Universidade Federal de São Paulo (protocol 4.071.731), CAAE 30384020.5.0000.5505, and informed consent was given as a prerequisite before enrolling each subject in this registry. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). Our standardized protocol for dTRA procedures has been extensively described elsewhere.12-14
Statistical analysis
Study data were collected and managed using Research Electronic Data Capture (REDCap) version 15.4.0 (Vanderbilt University), hosted at Escola Paulista de Medicina. Statistical analyses were performed using RStudio 2025.05.0+496 "Mariposa Orchid" for Windows, with support for Quarto 1.6.42. Continuous variables were expressed as mean ± SD and compared between chronic and acute coronary syndrome groups using Welch's t-test, which is appropriate for independent samples with different sizes and variances. Categorical variables were expressed as absolute and relative frequencies (n and %) and compared between the 2 groups using Pearson's chi-square test. P-values of less than 0.05 were considered statistically significant.
Results
The baseline demographic features and the procedural characteristics of all 6871 patients according to each group are shown in Tables 1 and 2, respectively. Overall, there was a predominance of acute coronary syndromes (3790 patients, 55.2%). The mean patient ages were 63.8 ± 15.7, 64.8 ± 15.7 and 62.9 ± 16 years for total, chronic, and acute coronary syndromes groups, respectively.
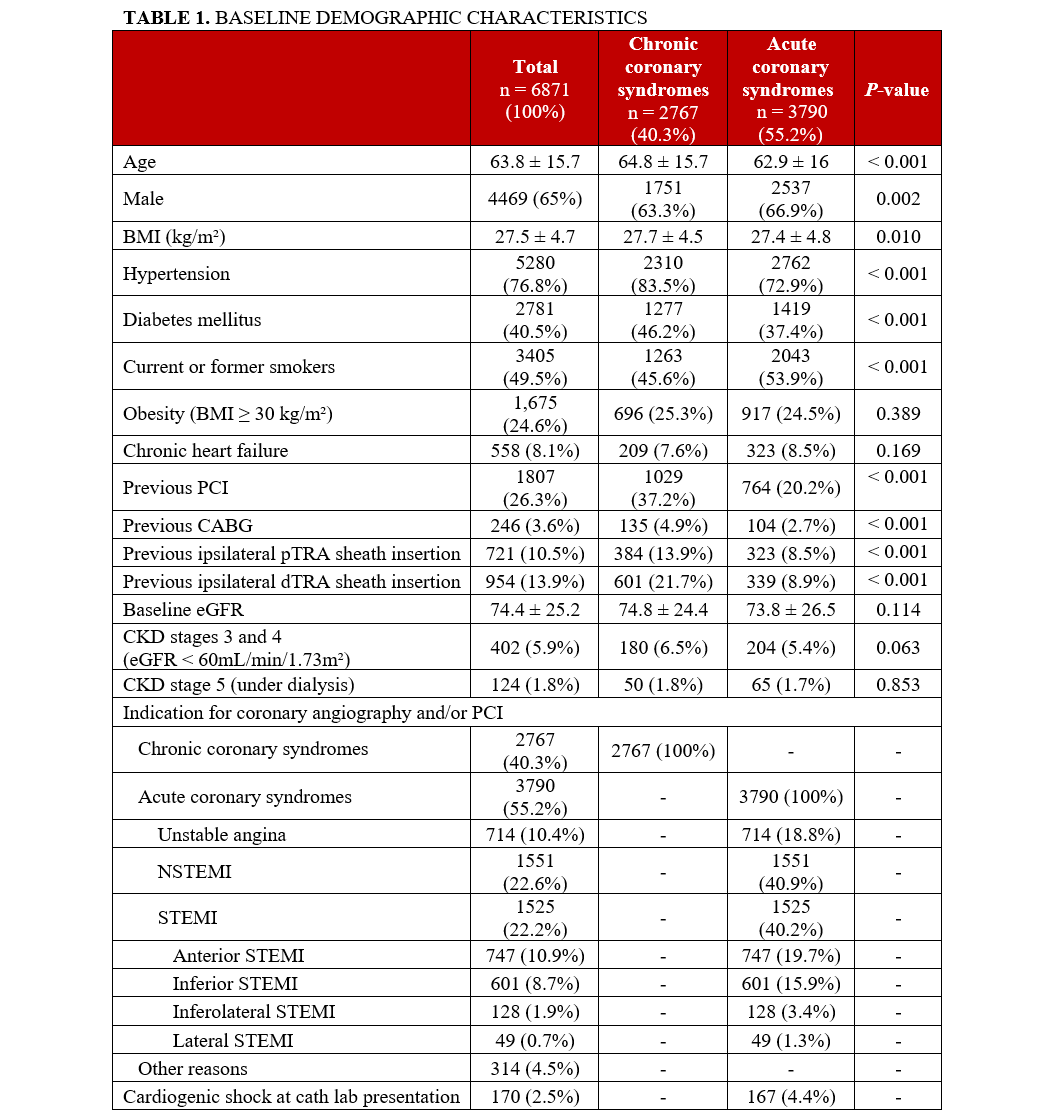
In the chronic coronary syndromes group (n = 2767, 40.3%), there was statistically significant predominance of hypertension (83.5% vs 72.9%; P < .001), diabetes (46.2% vs 37.4%; P < .001), previous PCI (37.2% vs 20.2%; P < .001), previous coronary artery bypass grafting surgery (4.9% vs 2.7%; P < .001), and previous ipsilateral pTRA (13.9% vs 8.5%; P < .001) or dTRA (21.7% vs 8.9%; P < .001) sheath insertion. In turn, in the acute coronary syndromes group, there was statistically significant predominance of male patients (66.9% vs 63.3%; P = .002) and patients who were former or current smokers (53.9% vs 45.6%; P < .001) (Table 1).
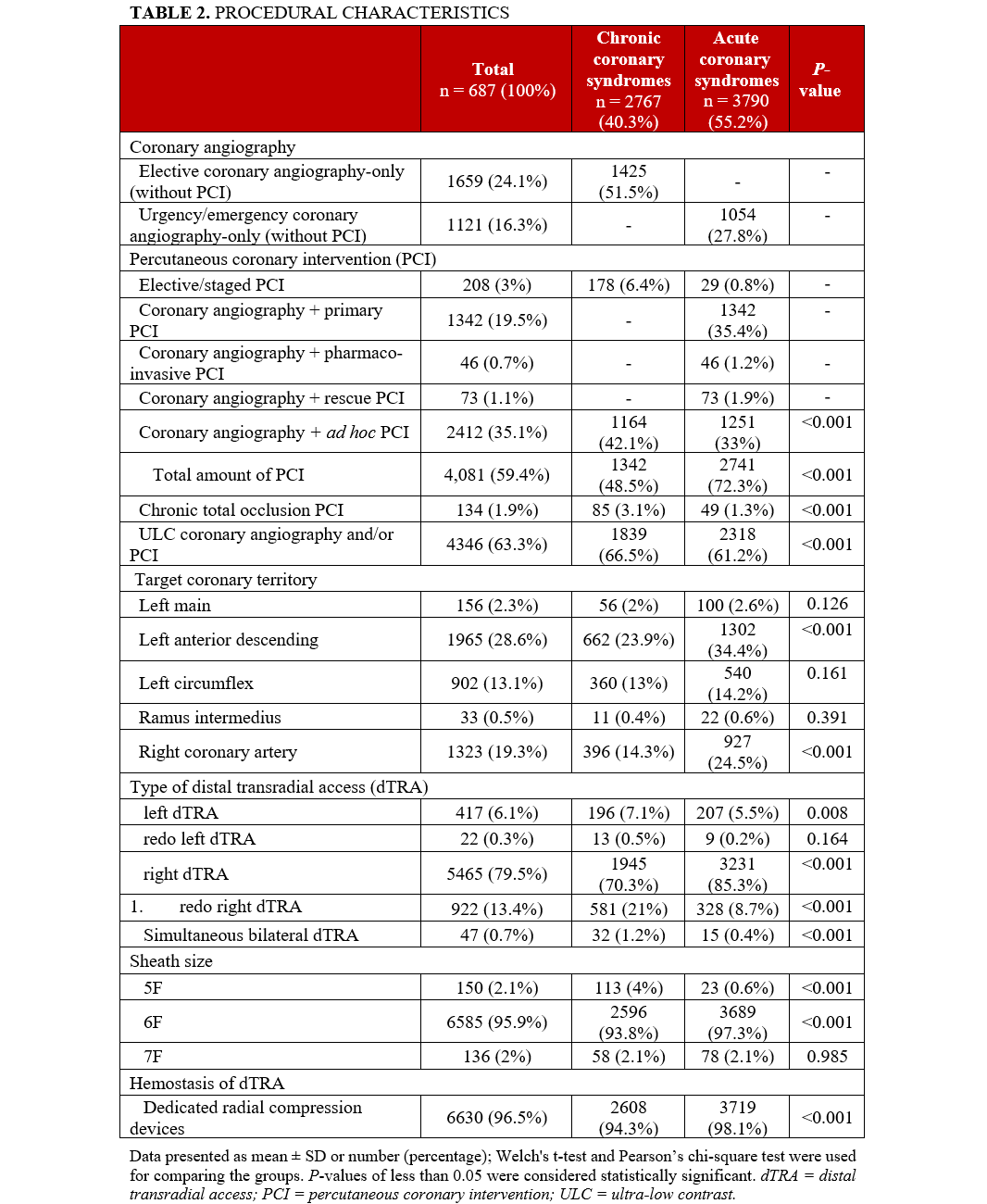
Regarding procedural characteristics, the rates of coronary angiography followed by ad hoc PCI (42.1% vs 33%; P < .001), chronic total occlusion PCI (3.1% vs 1.3%; P < .001), ultra-low contrast coronary angiography and/or PCI (66.5% vs 61.2%; P < .001), left dTRA (7.1% vs 5.5%; P = .008), redo right dTRA (21% vs 8.7%; P < .001), simultaneous bilateral dTRA (1.2% vs 0.4%; P < .001), and 5F sheath usage (4% vs 0.6%; P < .001) were statistically significantly higher in the chronic vs acute coronary syndromes group. In the acute syndromes group, there was statistically significant predominance of the total amount of PCI (72.3% vs 48.5%; P < .001), left anterior descending (34.4% vs 23.9%; P < .001) and right coronary (24.5% vs 14.3%; P < .001) arteries PCI, right dTRA (85.3% vs 70.3%; P < .001), 6F sheath usage (97.3% vs 93.8%; P < .001), and hemostasis with dedicated pneumatic radial compression devices (98.1% vs 94.3%; P < .001). Right dTRA, standard 6F radial sheaths, and hemostasis by dedicated pneumatic radial compression devices were undertaken for the vast majority of patients in both groups (Table 2).
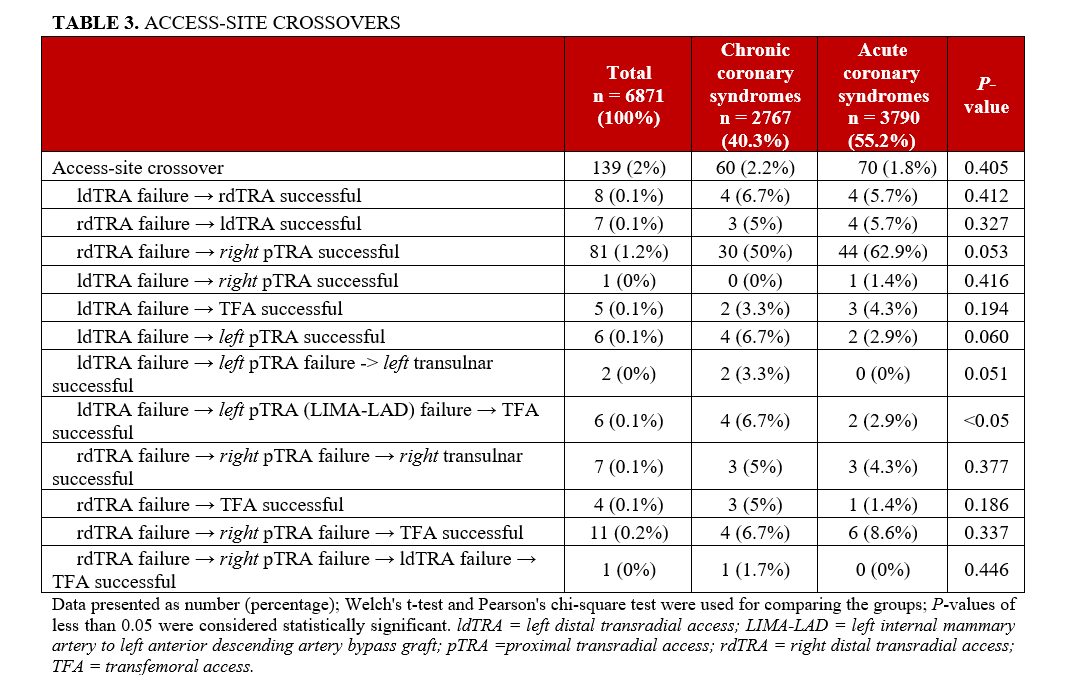
The total access-site crossover was quite low (2%); most were successfully performed via contralateral dTRA or any pTRA, without statistically significant differences between the 2 groups (Table 3).
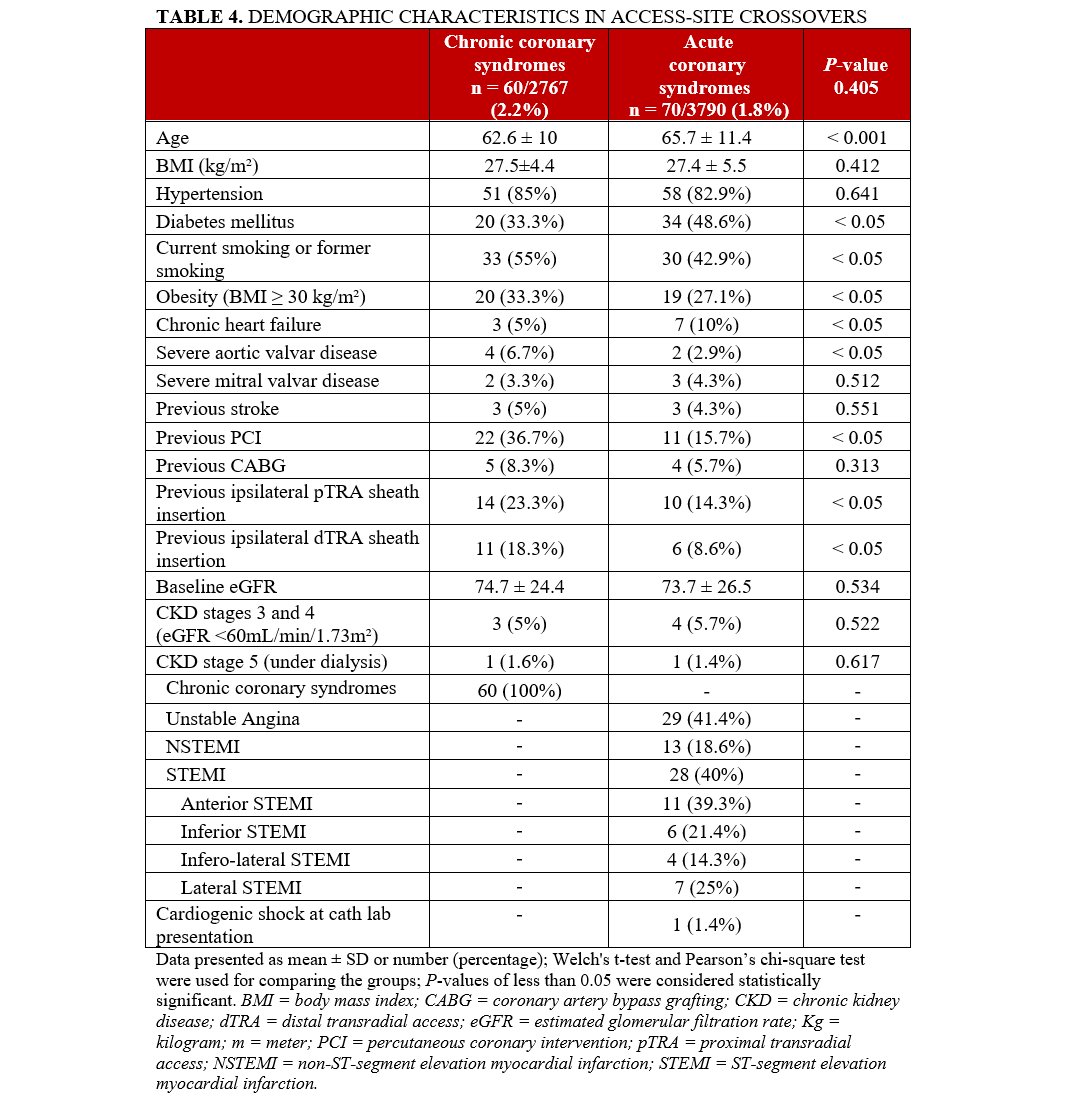
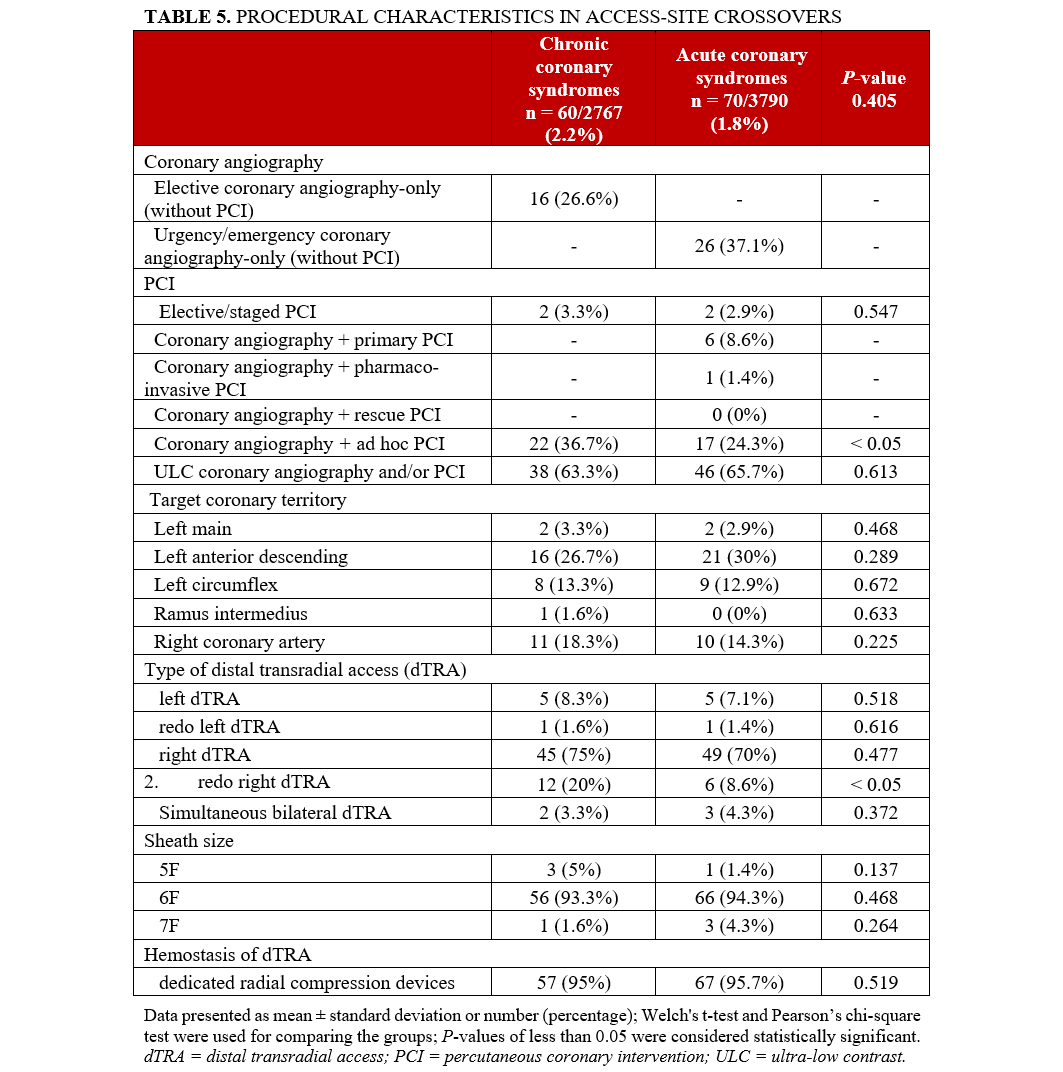
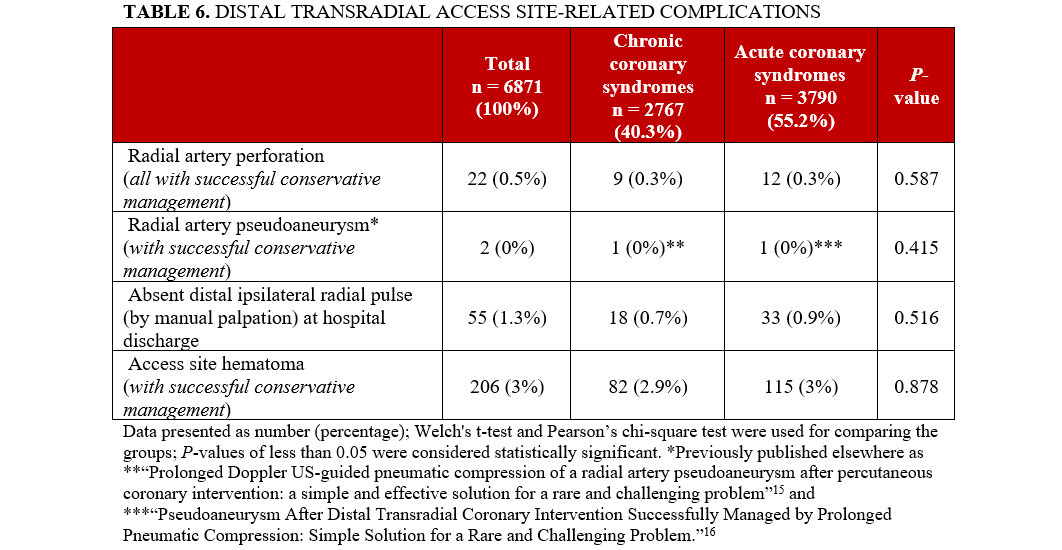
Tables 4 and 5 depict demographic and procedural characteristics in access-site crossovers only. Specific procedural-related complications are shown in Table 6.15,16
Discussion
To the best of our knowledge, the present study is the first to assess particularities of routine coronary angiography and/or PCI via dTRA in chronic vs acute coronary syndrome patients from a large, unselected, and real-world sample of all-comers comprising all presentations of coronary artery disease. Data were obtained from the DISTRACTION registry, the first Brazilian registry to address this issue. Since February 2019, our group has adopted dTRA as the default approach for routine coronary procedures, and our results have been continuously published.12-14,17-24
According to a recently published systematic review and meta-analysis encompassing 16 891 patients (8260 in the dTRA group and 8631 in the pTRA group) from 31 studies (13 randomized clinical trials, 15 prospective, and 3 retrospective),9 dTRA significantly reduced the incidence of radial artery occlusion (odds ratio [OR], 0.41; 95% CI, 0.34-0.50; P < .05) and hematoma (OR, 0.67; 95% CI, 0.56-0.80; P < .05) with shorter hemostasis time (weighted mean difference: -0.43; 95% CI, -0.65 to -0.20; P < .05), but had a significantly lower procedure success rate (OR, 0.41; 95% CI, 0.30-0.56; P < .05), a lower puncture success rate (OR, 0.44; 95% CI, 0.27-0.71; P < .05), and a longer puncture time (weighted mean difference, 0.60; 95% CI, 0.44-0.75; P < .05). No significant differences were observed between the 2 approaches in terms of success rate of a single attempt, radial artery spasms, puncture site bleeding, procedural time, and contrast volume. A subgroup analysis of patients with acute coronary syndromes showed that dTRA significantly reduced the incidence of radial artery occlusion, puncture point bleeding, hematoma, and radial artery spasms, but had significantly longer puncture time. There were no significant differences in the success rates of arterial puncture, procedural time, contrast volume, and hemostasis time.
Another recently published systematic review and meta-analysis assessed 4 studies comprising 543 patients who underwent emergency coronary procedures, of whom 447 (82.3%) had ST-segment elevation myocardial infarction (STEMI).10 Compared with pTRA, dTRA was associated with lower radial artery occlusion rates (relative risk [RR], 0.21; 95% CI, 0.06-0.72) and a shorter hemostasis time (mean difference, -4.23 h; 95% CI, -6.23-2.13). There was no significant difference between the 2 modalities in terms of puncture failure (RR, 1.38; 95% CI, 0.31-6.19), access-site crossover (RR, 1.37; 95% CI, 0.42-4.44), puncture time (mean difference, 0.33; 95% CI, -0.16-0.81), procedural time (mean difference, 0.97 min; 95% CI, -5.19-7.13), cannulation success (RR, 0.94; 95% CI, 0.83-1.06), and other periprocedural complications. These findings remained consistent in a subgroup analysis of patients with STEMI.
Xu et al evaluated 550 patients with acute coronary syndromes submitted to PCI via dTRA or pTRA.25 The rates of all-cause death (hazard ratio [HR], 0.688; 95% CI, 0.323-1.463; P = .331], cardiovascular death (HR, 0.330; 95% CI, 0.107-1.105; P = .053), major adverse cardiac events (HR, 0.806, 95% CI, 0.515-1.263; P = .347), and unplanned revascularization (HR, 0.860; 95% CI, 0.483-1.529; P = .606) were not significantly different between the 2 groups. PCI for acute coronary syndromes via pTRA compared with dTRA had the same long-term prognoses, but hemostasis time and bleeding rates were lower in patients undergoing PCI via dTRA.
Contrary to the majority of data published to date,6,7,9,26,27 which essentially included patients at stable conditions, we have been continuously including patients with any (even weak) proximal (and distal) radial artery palpable pulses, no matter the clinical scenario. Of note, the majority (55.2%) of the patients in the present study presented with acute coronary syndromes, being 22.2% of total casuistic with STEMI.
In the Korean Prospective Registry for Evaluating the Safety and Efficacy of Distal Radial Approach (KODRA) registry,27 access-site crossover occurred in 333 of 4977 (6.7%) patients. Since our very early experience with the DISTRACTION registry,12 access-site crossover has decreased from 3% to 2.5%, with 8.5-fold the initial number of patients,14 and then to only 2% after reaching more than 6800 consecutive patients.20,21 In this present analysis of 6871 patients, the total access-site crossovers rate—successful distal radial artery puncture but failed wire and sheath advancement—was kept very low (2%), with no statistically significant differences between chronic and acute coronary syndromes patients. The majority of dTRA crossover was successfully performed via any pTRA or contralateral dTRA, thus avoiding the transfemoral approach.
Limitations
All procedures of this observational registry were performed or supervised by 2 interventional cardiologists proficient with dTRA. Certain peculiarities may be specific to the population under study, in spite of being all-comers. The 2 groups were not comparable at baseline and the data cannot provide any meaningful conclusions on procedural parameters or outcomes; thus, the results of the present study should not be extrapolated or generalized to other centers and/or to interventional cardiologists unfamiliar with the technique. Distal radial artery puncture attempts, time to sheath insertion, and fluoroscopy and procedure times were not systematically recorded. Distal radial artery punctures were not performed under ultrasound guidance, and no distal or proximal radial artery diameters measurements were evaluated before or after the procedures. The lack of routine post-procedure Doppler ultrasound evaluation might have underestimated vascular complications rates.
Conclusions
When performed by proficient operators, routine coronary procedures via dTRA appear to be safe and feasible in both chronic and acute coronary syndromes, with similar low rates of access-site crossovers and complications.
Affiliations and Disclosures
Marcos Danillo Oliveira, MD, MSc; Adriano Caixeta, MD, PhD
From the Department of Interventional Cardiology, Hospital Universitário I, Escola Paulista de Medicina, Universidade Federal de São Paulo, São Paulo-SP, Brazil.
Acknowledgments: The authors acknowledge Samantha Propper, RCIS, BS, MBA (@dontmissabeat, orcid.org/0009-0007-5530-0851) for the preparation of the Figure.
Disclosures: The authors report no financial relationships or conflicts of interest regarding the content herein.
Address for correspondence: Adriano Caixeta, MD, PhD, Department of Interventional Cardiology, Hospital São Paulo, Escola Paulista de Medicina, UNIFESP. Napoleão de Barros, nº 715 - Vila Clementino, São Paulo-SP 04024-002, Brazil. Email: acaixeta@me.com
References
1. Corcos T. Distal radial access for coronary angiography and percutaneous coronary intervention: a state-of-the-art review. Catheter Cardiovasc Interv. 2019;93(4):639-644. doi:10.1002/ccd.28016
2. Byrne RA, Rossello X, Coughlan JJ, et al; ESC Scientific Document Group. 2023 ESC guidelines for the management of acute coronary syndromes. Eur Heart J. 2023;44(38):3720-3826. doi:10.1093/eurheartj/ehad191
3. Rao SV, O'Donoghue ML, Ruel M, et al. 2025 ACC/AHA/ACEP/NAEMSP/SCAI guideline for the management of patients with acute coronary syndromes: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2025;151(13):e771-e862. doi:10.1161/CIR.0000000000001309
4. Jolly SS, Yusuf S, Cairns J, et al; RIVAL trial group. Radial versus femoral access for coronary angiography and intervention in patients with acute coronary syndromes (RIVAL): a randomised, parallel group, multicentre trial. Lancet. 2011;377(9775):1409-1420. doi:10.1016/S0140-6736(11)60404-2
5. Alnasser SM, Bagai A, Jolly SS, et al. Transradial approach for coronary angiography and intervention in the elderly: a meta-analysis of 777,841 patients. Int J Cardiol. 2017;228:45-51. doi:10.1016/j.ijcard.2016.11.207
6. Ferrante G, Condello F, Rao SV, et al. Distal vs conventional radial access for coronary angiography and/or intervention: a meta-analysis of randomized trials. JACC Cardiovasc Interv. 2022;15(22):2297-2311. doi:10.1016/j.jcin.2022.09.006
7. Feghaly J, Chen K, Blanco A, Pineda AM. Distal versus conventional radial artery access for coronary catheterization: a systematic review and meta-analysis. Catheter Cardiovasc Interv. 2023;101(4):722-736. doi:10.1002/ccd.30602
8. Oliveira MD, Caixeta A. Distal transradial access to prevent proximal radial artery occlusion: what is really known? J Transcat Interv. 2021;29:eA202102. doi:10.31160/JOTCI202129A202102
9. Yang Q, Wei X, Wu J, et al. Efficacy and safety of distal transradial access for coronary angiography and percutaneous coronary intervention: a meta-analysis. Front Cardiovasc Med. 2025;12:1530995. doi:10.3389/fcvm.2025.1530995
10. Bittar V, Trevisan T, Clemente MRC, Pontes G, Felix N, Gomes WF. Distal versus traditional radial access in patients undergoing emergency coronary angiography or percutaneous coronary intervention: a systematic review and meta-analysis. Coron Artery Dis. 2025;36(1):18-27. doi:10.1097/MCA.0000000000001411
11. Sgueglia GA, Di Giorgio A, Gaspardone A, Babunashvili A. Anatomic basis and physiological rationale of distal radial artery access for percutaneous coronary and endovascular procedures. JACC Cardiovasc Interv. 2018;11(20):2113-2119. doi:10.1016/j.jcin.2018.04.045
12. Oliveira MD, Navarro EC, Kiemeneij F. Distal transradial access as default approach for coronary angiography and interventions. Cardiovasc Diagn Ther. 2019;9(5):513-519. doi:10.21037/cdt.2019.09.06
13. Oliveira MD, Navarro EC, Caixeta A. Distal transradial access for post-CABG coronary and surgical grafts angiography and interventions. Indian Heart J. 2021;73(4):440-445. doi:10.1016/j.ihj.2021.06.005
14. Oliveira MD, Navarro EC, Caixeta A. Distal transradial access for coronary procedures: a prospective cohort of 3,683 all-comers patients from the DISTRACTION registry. Cardiovasc Diagn Ther. 2022;12(2):208-219. doi:10.21037/cdt-21-542
15. Oliveira MD, Perillo P, Lemos L, Caixeta A. Prolonged Doppler US-guided pneumatic compression of a radial artery pseudoaneurysm after percutaneous coronary intervention: a simple and effective solution for a rare and challenging problem. J Vasc Bras. 2023;22:e20210212. doi:10.1590/1677-5449.202102122
16. Oliveira MD, Alves de Sá G, Navarro EC, Caixeta A. Pseudoaneurysm after distal transradial coronary intervention successfully managed by prolonged pneumatic compression: simple solution for a rare and challenging problem. J Invasive Cardiol. 2021;33(10):E836-E838. doi:10.25270/jic/21.00139
17. Oliveira MD, Caixeta A. Distal transradial access (dTRA) for coronary angiography and interventions: a quality improvement step forward? J Invasive Cardiol. 2020;32(9):E238-E239. doi:10.25270/jic/20.00160
18. Oliveira MD, Caixeta A. Distal transradial access for primary PCI in ST-Segment elevation myocardial infarction. JACC Cardiovasc Interv. 2022;15(7):794-795. doi:10.1016/j.jcin.2022.02.021
19. Oliveira MD, Navarro EC, Branca NR, Garcia ME, Scarpa MC, Caixeta A. Coronary procedures via distal transradial access in older as compared with non-older patients: insights from the DISTRACTION registry. J Invasive Cardiol. 2023;35(9). doi:10.25270/jic/23.00132
20. Oliveira MD, Motta RFOS, Caixeta A. Distal transradial access for coronary procedures: insights from 6,800 consecutive all-comers patients from the DISTRACTION registry. Int J Cardiovasc Sci. 2024;37:e20240084. doi:10.36660/ijcs.20240084
21. Oliveira MD, Motta RS, De Azevedo Oliveira LCF, Caixeta AM. Distal transradial access for coronary procedures: insights from 6,852 consecutive all-comers patients from the DISTRACTION registry. J Am Coll Cardiol. 2025;85(12):906.
22. Oliveira MD, Motta RS, Oliveira LC, Caixeta A. Ultra-low contrast strategy for routine coronary procedures: insights from the DISTRACTION (distal transradial access as default for coronary angiography and interventions) registry. J Am Coll Cardiol. 2025;85(12):1016.
23. Oliveira MD, Caixeta A. Ultra-low contrast strategy for routine coronary procedures via distal transradial access: real-world experience with consecutive all-comers patients from the DISTRACTION registry. J Invasive Cardiol. 2025;37(4). doi:10.25270/jic/24.00276
24. Oliveira MD, Caixeta A. Routine coronary procedures via distal transradial access in male versus female patients: insights from the DISTRACTION registry. J Invasive Cardiol. 2025. doi:10.25270/jic/25.00130
25. Xu L, Lu W, Shi G, et al. Comparison of long-term prognoses of percutaneous coronary intervention via distal transradial and conventional transradial access for acute coronary syndrome. Hellenic J Cardiol. 2025;83:28-37. doi:10.1016/j.hjc.2024.03.001
26. Coomes EA, Haghbayan H, Cheema AN. Distal transradial access for cardiac catheterization: a systematic scoping review. Catheter Cardiovasc Interv. 2020;96(7):1381-1389. doi:10.1002/ccd.28623
27. Lee JW, Kim Y, Lee BK, et al. Distal radial access for coronary procedures in a large prospective multicenter registry: the KODRA trial. JACC Cardiovasc Interv. 2024;17(3):329-340. doi:10.1016/j.jcin.2023.11.021