IBD for the Dermatologist: Extraintestinal Clues, Medication Overlap, and When to Refer
Ryan W. Stidham, MD, MS, delivered a clinically practical review of inflammatory bowel disease (IBD) tailored specifically for dermatologists during his Masterclasses in Dermatology session, “IBD for the Dermatologist: Update.” His focus: understanding Crohn’s disease (CD) and ulcerative colitis (UC), recognizing dermatologic extraintestinal manifestations (EIMs), and navigating overlapping therapeutics.
Dr Stidham framed IBD as “an abnormal systemic immune response leading to intestinal and extra-intestinal inflammation.” While UC is limited to mucosal inflammation of the colon in a continuous pattern, CD can affect the entire gastrointestinal tract, often involve the terminal ileum, and feature patchy, transmural inflammation.
A key distinction for dermatologists: “Symptoms do not reflect disease activity” in CD. Chronic transmural inflammation can lead to fibrosis, strictures, fistulas, and penetrating complications even when symptoms appear controlled. Early intervention with a goal of mucosal healing is critical to prevent long-term disability.
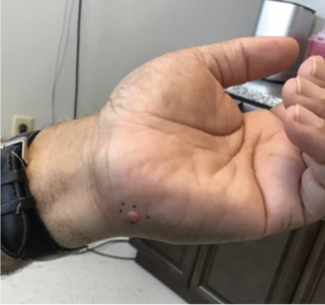
Extraintestinal manifestations occur in 30% to 40% of patients with IBD. Dermatologic EIMs affect 10% to 15%, with erythema nodosum (EN) being the most common. EN may precede IBD diagnosis in 15% of cases, and its activity often mirrors intestinal inflammation. Dr Stidham advised considering fecal calprotectin testing and GI referral, even in asymptomatic patients.
Pyoderma gangrenosum (PG), the second most common dermatologic EIM (1%–3%), behaves differently. “PG does not mirror IBD activity,” he noted. High-dose anti-TNF therapy remains effective, with increasing experience using JAK inhibitors and IL-23 agents. Peristomal PG presents unique challenges and often requires escalation of systemic therapy.
Cutaneous (metastatic) CD, although rare (<0.1%), is frequently misdiagnosed and may occur independently of gut severity. Histopathology is essential, and chronic biologic therapy is typically required.
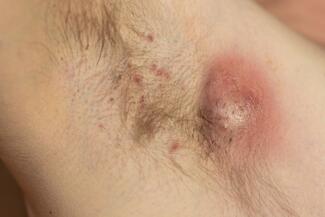
Hidradenitis suppurativa (HS) also intersects with IBD. Patients with CD have a fivefold increased risk of HS, which often precedes CD diagnosis. Magnetic resonance imaging of the pelvis can help distinguish perianal HS from Crohn’s-related fistulizing disease, as treatment strategies differ.
Medication overlap is increasingly relevant. Anti-TNF agents, JAK inhibitors, and IL-23 therapies may address both IBD and dermatologic disease. However, “IL-17 is generally contraindicated in IBD,” requiring close coordination with gastroenterology if considered.
Dr Stidham closed with a reminder that dermatologic EIMs can precede gastrointestinal symptoms and warrant evaluation for clinically silent disease. In patients with overlapping pathology, early, mechanism-driven therapy can prevent long-term complications on both sides of the gut-skin axis.
For more meeting coverage, visit the Masterclasses in Dermatology newsroom.
Reference
Stidham R. IBD for the dermatologist: update. Presented at: Masterclasses in Dermatology; February 19–22, 2026; Sarasota, FL.