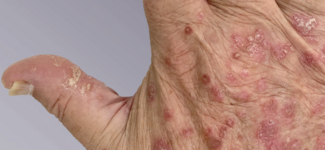
Beyond the Gut: Recognizing and Managing Inflammatory Bowel Disease in Dermatologic Practice

Inflammatory bowel disease (IBD) is often thought of as a condition confined to the gastrointestinal (GI) tract, but for many patients, its earliest or most visible signals may appear on the skin. And because cutaneous manifestations can precede GI symptoms, they offer a critical window for early diagnosis.
In this in-depth discussion, Dr David Fudman explores the intersection of IBD and dermatologic conditions, highlighting key clinical clues, shared inflammatory pathways, and practical strategies for interdisciplinary coordination between gastroenterologists and dermatologists.
THE DERMATOLOGIST’S ROLE IN IDENTIFYING IBD
The Dermatologist: What are the most common cutaneous manifestations of IBD that dermatologists should recognize early?
Dr Fudman: The 2 most common cutaneous manifestations of IBD are erythema nodosum (EN) and pyoderma gangrenosum (PG). EN tends to follow luminal disease activity, whereas PG may not necessarily do that. And it is remarkable how many patients with PG have underlying IBD—about half. Recognizing this as a potential signal of an underlying diagnosis of IBD is key.
The Dermatologist: How frequently do you see skin symptoms precede GI symptoms in patients with IBD?
Dr Fudman: While this may not be specific to dermatologic manifestations, in general, extraintestinal manifestations of IBD, including those of the joints, skin, eyes, and other organs, preceed the diagnosis of IBD in 1 in 4 patients, so it is quite common
The Dermatologist: Are there particular patient demographics or risk factors that should raise clinical suspicion?
Dr Fudman: In terms of patients who have cutaneous manifestations, there are a few hints. GI symptoms can be a clue. Abdominal pain is the most common symptom in Crohn’s disease rather than diarrhea. Ulcerative colitis is more commonly manifested by diarrhea or hematochezia. A family history of IBD can often be present in patients who have other findings that are not explained; for example, iron deficiency anemia or persistent elevation of inflammatory markers despite control of the skin condition, or other pieces that just do not quite fit the picture. These should definitely raise your eyebrows to look for something underlying such as IBD.
THE GUT-SKIN CONNECTION
The Dermatologist: How do you explain the pathophysiologic link between intestinal and cutaneous inflammation?
Dr Fudman: We know that there are shared pathophysiologic mechanisms between cutaneous and luminal autoimmune diseases and that is why we can often use many of the same medications to treat both sets of conditions. There are also some shared genetic predispositions between hidradenitis suppurativa (HS), PG, and psoriasis and IBD, particularly with Crohn’s disease. There are shared cytokine pathways and environmental triggers, and links between cutaneous diseases and microbiome dysfunction just as we see with IBD. Overall, it is not completely teased out, but it is definitive that there is a pathophysiologic link.
The Dermatologist: Have biomarkers or imaging tools emerged that can help dermatologists identify systemic inflammation earlier?
Dr Fudman: From an IBD perspective, we have a valuable tool for screening for luminal bowel inflammation, although it is not the most convenient. And that tool is stool calprotectin, a protein produced by neutrophils. It is much more sensitive to bowel inflammation than systemic markers of inflammation, such as C-reactive protein or erythrocyte sedimentation rate. By testing for calprotectin in the stool, we can detect gut inflammation with much more sensitivity than we can with any blood test. Although calprotectin can be elevated by any cause of gut inflammation, such as infection, ischemia, or even peptic ulcers, a normal calprotectin level almost always rules out IBD. So, if in the clinic there is any suspicion that there may be underlying IBD, a simple stool test can often create reassurance because of its very good negative predictive value. Of course, its positive predictive value is not as good, but that may trigger the referral to a gastroenterologist to determine whether any further workup, such as imaging or a colonoscopy, may be prudent.
BIOLOGIC THERAPY AND SHARED MANAGEMENT
The Dermatologist: How should dermatologists approach biologic therapy selection for patients with concurrent IBD and HS or psoriasis?
Dr Fudman: For patients with both IBD and HS, we typically try to pick a single biologic therapy to treat the IBD, whether perianal or luminal, and HS. While these are classically thought of as distinct entities, we know that certain patients fit in the middle of a Venn diagram of these diseases. Typically, in our practice, we prefer to use anti-TNFs for patients with IBD and HS, and there is evidence from Crohn’s perianal disease that we need to target high trough levels of our anti-TNFs to have good fistula outcomes. There are limited data from the dermatology literature that suggests the same—higher trough levels are helpful in terms of improving HS outcomes. In patients who have active Crohn’s perianal disease, we target levels of at least 10 mcg/mL for infliximab, perhaps closer to 15 to 20 and certainly over 10 mcg/mL or even higher for adalimumab as well. If a patient has well-controlled perianal disease, we do not necessarily target a specific level if the disease is quiescent and the patient’s drug level is not so low that it puts them at risk for immunogenicity.
For patients with psoriasis and IBD, typically in our practice we use IL-23s. If the patient has both psoriatic and luminal manifestations, IL-23s or ustekinumab tend to work quite well.
The Dermatologist: Can you highlight some key differences in how biologic agents affect IBD vs dermatologic diseases?
Dr Fudman: In general, for IBD, we need to use higher doses of our advanced therapies, whether that is a JAK inhibitor or biologics like anti-TNFs or IL-23s, all of which might share activity in psoriasis. For example, when using a JAK inhibitor for IBD, we start with an induction dose of 45 mg and most of the time maintain 30 mg vs the lower 15-mg dose. And we typically use higher doses of ustekinumab or IL-23s, as well as targeting higher trough levels for anti-TNFs. In general, it seems that we need much more drug to treat IBD than we need to treat skin disease, although HS may be an exception. This comes into play when we consider what type of dosing to use in patients who have both IBD and skin disease, recognizing that often the on-label dosing for different diseases is quite different. For example, the on-label risankizumab dosing for IBD that we most commonly use is 360 mg every 8 weeks for maintenance, which is more than twice the label dose for psoriasis.
The Dermatologist: What are the red flags or contraindications that dermatologists should know before initiating certain biologics such as IL-17 inhibitors?
Dr Fudman: IL-17s are certainly a special case, as we know that they can either trigger de novo IBD or exacerbate existing IBD. For this reason, it is prudent to take a brief history of any chronic GI symptoms or family history of IBD before starting a patient on an IL-17 inhibitor. Expert consensus recommends checking calprotectin as well. If the calprotectin level is normal and there are no other red flags, you can feel comfortable proceeding with IL-17 therapy with regard to minimizing IBD risks. In contrast, if the calprotectin level is high, that would warrant either consideration of an alternative agent or referral to a gastroenterologist to see if the elevated calprotectin requires any further workup. If the patient is found to have just quiescent IBD, then it is not contraindicated to proceed with IL-17 therapy, but if there is an alternative, typically that would be preferred. However, if a patient has active or historically difficult to control IBD, we are always going to try to avoid an IL-17 agent.
The Dermatologist: How should dermatologists coordinate co-management with gastroenterology for these complex cases?
Dr Fudman: As a gastroenterologist, I think having a relationship with my dermatology colleagues who are comfortable managing these cases is important. Sometimes it is going to be better for the gastroenterologist to prescribe a medication; sometimes it is going to be better for the dermatologist to prescribe a medication, so having an open line of communication is imperative. Perhaps we are using 2 different advanced therapies, in which case it may make sense for one specialist to prescribe one and the other to prescribe another to facilitate payer coverage. I think understanding each other’s assessment of a patient’s disease activity is also very helpful. If I see a patient with psoriasis and they find their symptoms burdensome, is this something that the dermatologist feels warrants biologic therapy? Should I be making my decision on biologic therapy to try to overlap efficacy with the patient’s psoriasis or does the dermatologist feel I should choose whatever agent I think will work best for the luminal disease? These are the types of conversations we can have on a routine basis to make sure we are getting the patient on the right track regarding which types of cytokine blockers we choose for them.
EMERGING RESEARCH AND EVOLVING PRACTICE
The Dermatologist: What do you find most exciting or promising in current IBD-dermatology research?
Dr Fudman: One of the most exciting things is our work on combination therapy. The reality is that we cannot always treat all of the patient’s immune-mediated diseases with one drug. We have been piecemealing this together for a decade now; we combine drugs based on predominantly retrospective evidence and very little prospective evidence. But as drugs are trialed in combination, more will have good perspective data, not just on efficacy, but also on the safety of this approach, which is not as well characterized in a retrospective manner. Even if these studies are not specifically on IBD, we can extrapolate them to our treatment of skin disease plus luminal disease at the same time. And moreover, we continue to see development of single-agent drugs that are effective for both psoriasis and luminal disease.
The Dermatologist: Are there new therapeutic targets or trials?
Dr Fudman: We are enthusiastic to see the results of ongoing phase 3 trials for 3 separate therapies in the TL1A class of medications. These seem to hold great promise in Crohn’s disease and look to be effective in ulcerative colitis as well. One of the reasons we are excited about these therapies is that it seems like they will be effective across many different extraintestinal manifestations of IBD, potentially including axial arthritis. This is a condition we have trouble with, given that right now our only options to cover both the gut and the axial skeleton are anti-TNFs and JAK inhibitors. Presumably, the TL1A class will also be effective in a variety of skin conditions, and we will see how this plays out over the next few years.
The Dermatologist: How might microbiome research or precision medicine reshape dermatologic care for IBD-associated conditions?
Dr Fudman: In the field of IBD, there is a big focus on the microbiome, but we have not yet learned to manipulate it in a way that is consistently therapeutically effective. This is due to a variety of reasons, including heterogeneity of fecal microbiota products, as well as a lack of understanding completely how we can pursue things like engraftment so that any microbiome changes we induce are durable. But presumably many of the same lessons we learn in the IBD space can be applied to the dermatology space and vice versa. It is possible that we may see something like a microbiome adjunct therapy to one of our biologic therapies, for example, that could also be used for controlling skin disease, not just luminal disease. Of course, that research is still ongoing and years away from clinical practice.
PATIENT-CENTERED AND PRACTICAL TAKEAWAYS
The Dermatologist: How can dermatologist best communicate with patients who may be reluctant to pursue GI evaluation?
Dr Fudman: I think the key message is that it may be the patient’s symptoms triggering the suspicion of an underlying GI disorder. Hopefully, by seeing the gastroenterology team, they can have some improvement in their quality of life, whether the diagnosis is ultimately IBD or something else. But if they do have IBD, particularly if they have Crohn’s disease, the earlier we get effective therapy on board, the more likely they are to avoid disease complications, such as flares, hospitalization, and surgery. We know in Crohn’s disease that the difference between early vs later initiation of therapy is huge, and so if we can get the patient plugged into care earlier, we can assure them that their outcomes will be better.
The Dermatologist: What clinical pearls can help streamline interdisciplinary care?
Dr Fudman: Recognizing the extraintestinal manifestations of IBD and that coordinated selection of a single advanced therapy or multiple therapies can get the patient on the right track is important. As is understanding that the dosing may be higher on the GI side and therefore it may be more helpful for the gastroenterologist to prescribe the medication so the patient can more easily receive the higher dose even if we are predominantly treating a skin condition. The other thing would be to make sure that we facilitate early diagnosis of IBD by referring patients with any degree of suspicion and sending them to the gastroenterologist with the calprotectin stool test completed. Since the dermatologist has already established a rapport with the patient, it may be easier to convince them to do the stool test rather than the gastroenterologist they just met. It is sometimes not straightforward to persuade patients to complete stool tests because of both the nature of the test and the inconvenience of it. But if the patient arrives with the calprotectin stool test completed, it may result in a different care pathway than if the first step at the gastroenterologist visit is to check the calprotectin.
The Dermatologist: If you could leave dermatology practitioners with a key takeaway message about IBD, what would it be?
Dr Fudman: The biggest takeaway from my perspective is that it is a team sport to coordinate care for patients who have cutaneous manifestations of IBD or both IBD and an immune-mediated skin condition, particularly regarding dosing and selection of advanced therapies, as well as treatment targets. We very much rely on our partners in dermatology, and I know our dermatology partners count on us. Getting on the same page about which types of therapies we can use to best target all the manifestations our patients have at what doses and what are the practicalities in terms of who is prescribing takes a team approach so we can get our patients better faster and for longer.
Conclusion
As IBD is increasingly recognized as a systemic, immune-mediated condition, dermatologists are often on the front lines of detection, encountering cutaneous manifestations that may precede or parallel luminal disease. Recognizing these warning signs, understanding shared inflammatory pathways, and appreciating how treatment strategies differ between the skin and gut are essential to optimizing care. Just as important is close collaboration between dermatology and gastroenterology, aligning on diagnosis, drug selection, dosing strategies, and treatment goals. By embracing a team-based, interdisciplinary approach and prioritizing early evaluation and intervention, clinicians can improve disease control, reduce complications, and ultimately deliver better, more durable outcomes for patients living with IBD and its dermatologic manifestations.
Disclosure: Dr Fudman is on consulting/advisory boards for Pfizer, Fresenius Kabi, Janssen Pharmaceuticals, and Eli Lilly and Company.