EGFR Inhibitor Rashes: Prophylaxis, Isotretinoin, and When to Culture
At the 2026 Masterclasses in Dermatology Annual Meeting, Meghan Heberton, MD, delivered a practical roadmap for managing epidermal growth factor receptor (EGFR) inhibitor toxicities, highlighting prevention, early intervention, and drug-specific nuances.
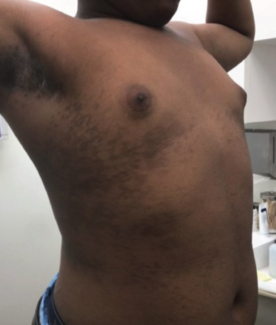
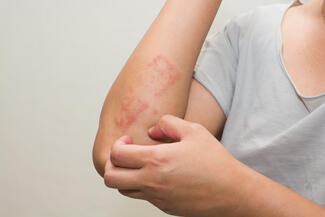
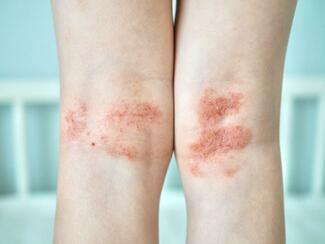
EGFR inhibitors include small-molecule tyrosine kinase inhibitors (osimertinib, erlotinib) and monoclonal antibodies (cetuximab, panitumumab). Cutaneous toxicities are common and predictable, forming a recognizable constellation: acneiform eruption, xerosis, eczema, paronychia, fissures, hair changes, and staphylococcal infections.
Acneiform eruptions occur in more than half of patients—estimates approach 90% in some series—and typically begin within weeks 1–2 of therapy. Papules and pustules involve the face, scalp, chest, and back, often “more pronounced with monoclonal antibodies.” Notably, severity of rash correlates with treatment response; in metastatic colorectal cancer, grade ≥2 rash with cetuximab was associated with improved survival (hazard ratio 0.33; P<.001).
Superinfection is common and often underrecognized. Retrospective data show staphylococcal, MRSA, HSV, and dermatophyte infections in up to 38% of patients. Rapid worsening or disproportionate pain should prompt culture. There is a “low suspicion to look for superinfection; culture an unroofed pustule.” Cephalexin may be preferred over chronic doxycycline in patients who are heavily pretreated.
Paronychia affects approximately 20% of patients and typically develops after months of therapy, often coexisting with infection. Painful nail fold inflammation may include pyogenic granulomas and superinfection (72% Gram-positive). Early intervention, including dilute vinegar soaks, clobetasol ointment, and mupirocin, is critical. Severe cases may require nail avulsion or partial matricectomy.
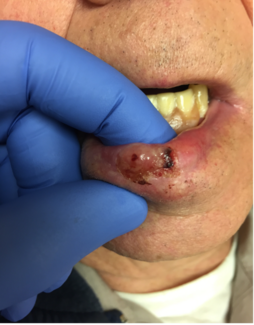
Amivantamab, the “new kid on the block,” presents distinctive toxicities, including early severe scalp rash and genital/lower extremity ulcerations. In the MARIPOSA and COCOON trials, structured dermatologic management significantly reduced grade ≥2 adverse events (42% vs 75% at week 12).
Dr Heberton closed with future areas of research: “It's in the literature that many patients with these toxicities also have concomitant zinc nutritional deficiencies. We don't know if correcting those helps with the rash, but it's always good for our patients to be nutritionally whole, and so that's something I also screen for in these patients.”
There is “lots of room to figure out how to help these patients with target inhibitors,” she concluded. “Don't be afraid to give them a break.”
For more meeting coverage, visit the Masterclasses in Dermatology newsroom.
Reference
Heberton M. Managing EGFR side effects. Presented at: Masterclasses in Dermatology; February 19–22, 2026; Sarasota, FL.