Checkpoint Inhibitor Rashes: When to Treat, When to Rechallenge, and When It’s Not the Drug
At the 2026 Masterclasses in Dermatology Annual Meeting, Meghan Heberton, MD, delivered a practical framework for evaluating and managing cutaneous toxicities of cancer immunotherapy. Her message: Grade carefully, diagnose precisely, and avoid reflexive steroid escalation.
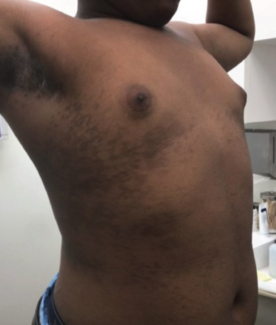
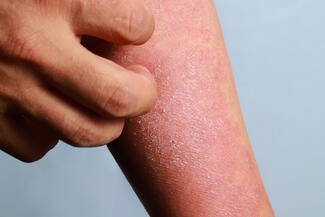
Immune checkpoint inhibitors (ICIs), including PD-1 and PD-L1 inhibitors, are now standard across multiple malignancies, from melanoma to cervical cancer and urothelial carcinoma. Cutaneous immune-related adverse events (cIRAEs) are among the most common toxicities and span eczematous, morbilliform, psoriasiform, lichenoid, bullous pemphigoid, vitiligo, granulomatous, and even Stevens-Johnson syndrome/toxic epidermal necrolysis-like reactions.
Lichenoid eruptions are common and range from subtle lichenoid keratoses to classic lichen planus with mucosal involvement. Management may include topical steroids, phototherapy, acitretin, or apremilast.
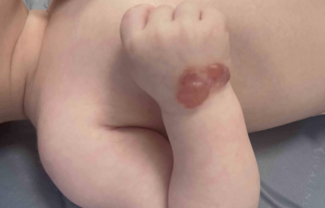
Psoriasis and psoriasiform eruptions may represent flares of pre-existing disease or de novo onset. Bullous pemphigoid (BP), although rare, is often therapy-limiting. “This is also something that presents with great latency.” In an MD Anderson review, most BP cases required ICI interruption and steroid-sparing agents. Dupilumab has emerged as a targeted option for BP-associated cIRAEs.
Next, Dr Heberton discusses treatments and rechallenges. Systemic corticosteroids may blunt immunotherapy efficacy. “Steroids are associated with poor responses to immunotherapy,” Dr Heberton noted, although indication and context matter. Emerging data suggest that biologics used alongside steroids in BP may not negatively impact tumor response and may even correlate with improved outcomes.
Rechallenge decisions require nuance. In one case, a patient with biopsy-confirmed autoimmune eruption and positive Ro antibody improved on low-dose methotrexate and hydroxychloroquine, then successfully resumed pembrolizumab. “If there’s a clear alternative etiology or diagnosis, I push for rechallenge even in severe cases,” Dr Heberton emphasized.
“Not all that happens on immunotherapy is related to immunotherapy,” she reminded the audience.
For more meeting coverage, visit the Masterclasses in Dermatology newsroom.
Reference
Heberton M. Cutaneous toxicities of cancer immunotherapy. Presented at: Masterclasses in Dermatology; February 19–22, 2026; Sarasota, FL.