Nearly 30 Percent of Patients With Resistant Hypertension Have a Hormone Disorder Caused by High Cortisol
Study led by Mount Sinai researcher can help clinicians find optimal therapies for blood pressure elevation from cortisol
Study led by Mount Sinai researcher can help clinicians find optimal therapies for blood pressure elevation from cortisol
New primary results from the MOMENTUM Study (“Prevalence and Clinical Impact of Hypercortisolism in Individuals with Resistant Hypertension”) show that 27% of patients with resistant hypertension have hypercortisolism, a rate that researchers say is higher than previously understood. The findings were presented as a Featured Clinical Research Presentation at the American College of Cardiology (ACC) Scientific Session 2026 by Deepak L. Bhatt, MD, MPH, MBA, Valentin Fuster Professor of Cardiovascular Medicine at the Icahn School of Medicine at Mount Sinai and Director of Mount Sinai Fuster Heart Hospital.
Resistant hypertension occurs when blood pressure remains elevated despite treatment with three or more different blood pressure medications and affects nearly 10 million Americans with high blood pressure. The MOMENTUM results suggest a substantial subset of these patients may have an underlying endocrine driver, excess cortisol, that contributes to persistent hypertension despite standard therapy.
“The fact that such a high percentage (more than 25 percent) of patients with resistant hypertension have elevated cortisol levels is very different from what doctors have been historically taught in medical school. These findings should prompt more screening for excess levels of cortisol in patients with resistant hypertension,” said Dr. Bhatt. “The next step to further this research is conducting randomized trials to determine if therapies that lower the impact of cortisol can safely and effectively treat high blood pressure in these patients.”
Why this matters
Resistant hypertension places patients at high risk of cardiovascular complications, including heart attack and heart failure. Hypercortisolism — when the body produces too much cortisol, often referred to as the “stress hormone” — can also contribute to broader metabolic and functional problems, including weight gain, muscle loss, and diabetes. Identifying hypercortisolism may provide patients and clinicians with a clearer explanation for difficult-to-control blood pressure and may open additional treatment considerations focused on the underlying condition.
Study design and methods
MOMENTUM is described as the first U.S.-based study and the largest study to date to assess the prevalence of hypercortisolism among individuals with resistant hypertension. Researchers analyzed 1,086 participants across 50 centers in the United States, including the Mount Sinai Health System in New York.
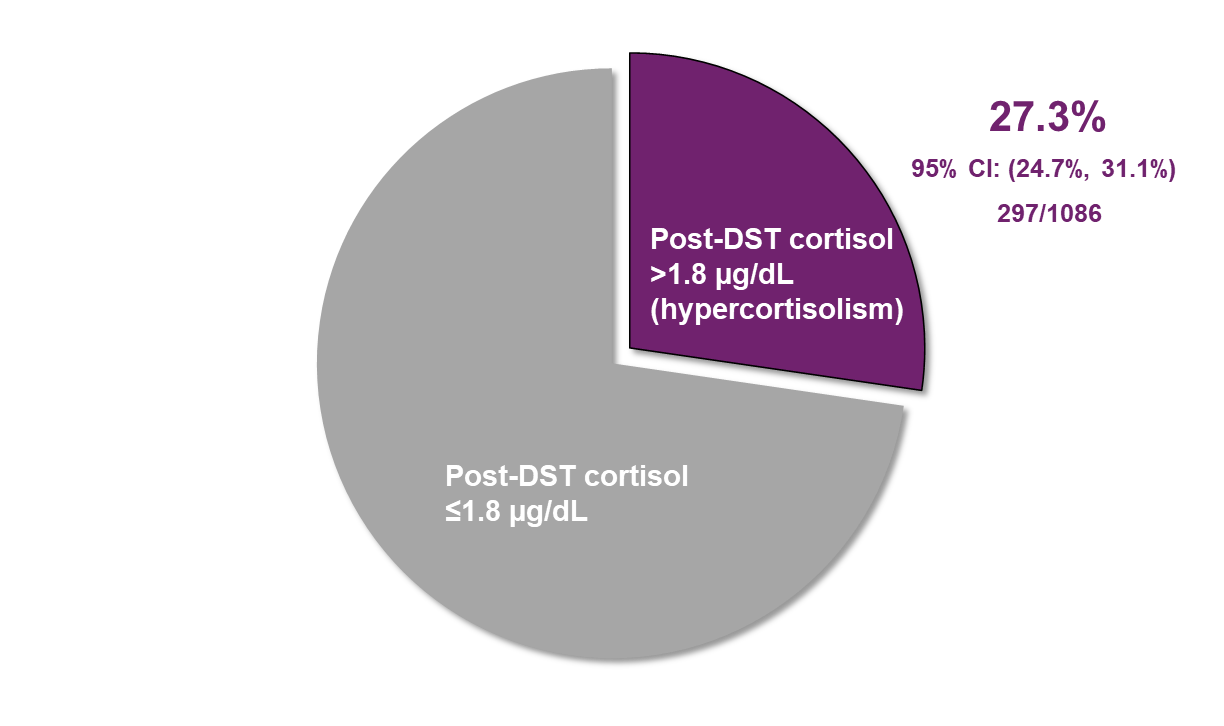
After confirming eligibility, participants underwent a dexamethasone suppression test, which involved taking a tablet of dexamethasone before bedtime followed by a morning blood test to measure cortisol. Participants with a morning cortisol level greater than 1.8 µg/dL were classified as having hypercortisolism.
Results
- 297 of 1,086 participants (27%) met criteria for hypercortisolism.
- Investigators also identified characteristics that may increase the likelihood of hypercortisolism; for example, patients with poor kidney function were more likely to have hypercortisolism.
- The study also assessed primary hyperaldosteronism (excess aldosterone), another potential contributor to resistant hypertension:
- Approximately 20% of participants had primary hyperaldosteronism.
- About 6% had both hypercortisolism and hyperaldosteronism.
- Approximately 20% of participants had primary hyperaldosteronism.
Implications for clinicians and patients
The findings suggest clinicians should consider elevated cortisol as a potentially meaningful contributor to resistant hypertension, particularly for patients at higher risk. Screening is described as practical and patient-acceptable, and the results may encourage more routine evaluation of endocrine drivers in patients whose blood pressure remains uncontrolled despite multiple medications. For patients, persistent high blood pressure despite several medications may be a reason to discuss screening for hypercortisolism with their clinician.
Funding and disclosures
The MOMENTUM Study was sponsored and funded by Corcept Therapeutics Incorporated. Dr. Bhatt is a paid consultant for Corcept Therapeutics Incorporated.
Find More:
Renal Denervation Topic Center
Cardiovascular Ambulatory Surgery Centers (ASCs) Topic Center
Grand Rounds With Morton Kern, MD
Peripheral Artery Disease Topic Center