More Than Cosmetic: Reframing Hyperpigmentation as a Clinical and Psychosocial Priority

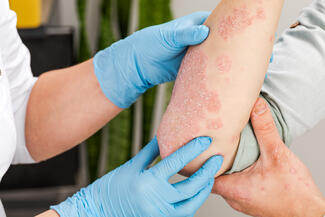
Hyperpigmentation is often minimized as a cosmetic issue, yet for many patients, particularly those with skin of color, it represents a chronic, emotionally taxing condition with significant clinical implications. From post-inflammatory hyperpigmentation (PIH) that lingers long after acne or injury has resolved to conditions like melasma, hyperpigmentation disorders can profoundly affect quality of life, mental health, and trust in care.
In this in-depth conversation, Dr Oyetewa Asempa offers practical insights into diagnosis, counseling, and treatment of hyperpigmentation disorders. Drawing on clinical experience and emerging evidence, Dr Asempa discusses common pitfalls, evolving therapies, and the importance of culturally competent, patient-centered care, underscoring why thoughtful, proactive management of hyperpigmentation is essential in dermatologic practice.
FRAMING THE CLINICAL CHALLENGE
The Dermatologist: Hyperpigmentation is often labeled as a cosmetic concern. Why is it important to reframe it as a medical and psychosocial priority, especially in patients with skin of color?
Dr Asempa: In the case of PIH, the initial inflammation that causes the dark spots is often temporary, but the hyperpigmentation can be long-lived. For a lot of our patients, their main concern is not the inflammation. They will often report having a pimple that lasted a week, but the resultant dark spot lasting for years, which is often more devastating from the patient's perspective. Then we have the types of hyperpigmentation that are, in and of themselves, the disease, such as melasma. From a mental health perspective, multiple studies have shown that patients are often much more concerned about hyperpigmentation than other dermatologic conditions.1-4 Melasma in particular has been associated with significant mental health concerns, such as anxiety and depression, in patients with darker skin.5,6 This makes sense because the more resident melanin that a person has in their skin, the more likely they are to develop hyperpigmentation and the more likely it is to last for a long period of time. Hyperpigmentation definitely warrants clinical attention beyond cosmetic considerations due to its significant psychosocial burden.
The Dermatologist: What do you see as the most common clinical missteps in diagnosing and managing hyperpigmentation disorders?
Dr Asempa: The first misstep is that clinicians may ignore or dismiss the hyperpigmentation altogether, opting to address acne first and leave the hyperpigmentation for later. However, in PIH, hyperpigmentation should always be treated at the same time as the inflammation that causes it. Of course, you will have a better handle on the hyperpigmentation if you reduce the culprit inflammation, but your patient may be more concerned about the PIH than their acne. It is important to build rapport with the patient by explaining that your treatment regimen is going to address both the inflammation and the hyperpigmentation at the same time.
A second misstep is not adequately counseling patients about photoprotection. Even though patients with darker skin are significantly less likely to develop skin cancer from the sun, they are much more likely to develop a hyperpigmentation disorder due to UV exposure. A clinician may tell their patient that a tinted mineral sunscreen must be used, but individuals with darker skin are less likely to find tinted sunscreens that match their skin tone. This can lead to reduced adherence to treatment. Instead, I recommend giving patients the option between using broad-spectrum tinted sunscreens that contain iron oxides (mineral or mixed mineral/chemical) or using non-tinted sunscreens and applying makeup with iron oxides on top. The latter option may work better for some and encourage compliance.
DIAGNOSTIC CONSIDERATIONS
The Dermatologist: PIH, melasma, erythema dyschromicum perstans (EDP), and lichen planus pigmentosa (LPP) can look similar. What key clinical or histopathologic clues help distinguish between these diagnoses?
Dr Asempa: With PIH, I want to know if there was an inciting event. The history should tell you that there was some preceding inflammation or injury and then the distribution should make sense for the preceding inflammation or injury. Even if it looks like PIH to me, if the patient is certain that there was never an inflammatory lesion in the area, I need to at least consider other diagnoses.
Melasma has the classic clinical appearance of symmetric facial distribution on the cheeks, upper lip, and forehead, so it tends to be a bit easier to diagnose. You may find that the patient has had a hormonal trigger like pregnancy or hormone replacement therapy.
With EDP and LPP, it is a lot tougher. Some clinicians will say if it used to be itchy and red, then it is EDP. If it is more of a blue-gray pigmentation, then it is LPP. I think of EDP and LPP as being on the acquired dermal macular hyperpigmentation (ADMH) spectrum. I do a biopsy for all my patients who may have EDP or LPP. If I see any active lichenoid inflammation, then it might push me toward LPP, but even with the dermatopathologist it is sometimes hard to make the call. In general, both EDP and LPP have dermal pigment and are difficult to treat.
The Dermatologist: What role does a thorough patient history, including environmental exposures and contact allergens, play in diagnosing hyperpigmentation disorders?
Dr Asempa: The patient’s history plays a large role. We need to understand how long the hyperpigmentation has been going on and what parts of the body are affected. Although you may initially only see hyperpigmentation on the face and neck, the patient may also have it on the torso, which may help with your diagnosis. Is it only in a sun-exposed area? Is the patient taking any medications that can cause drug-induced hyperpigmentation? Although the hyperpigmentation may look like LPP at first, if the patient has been on tetracycline or hydroxychloroquine, that could be why they have hyperpigmentation.
There is growing evidence that contact sensitization may trigger conditions on the ADMH spectrum, such as LPP, EDP, and pigmentary contact dermatitis.7-9 In certain studies, it has been found that up to one-third of the conditions on the ADMH spectrum may have some relation to contact sensitization, particularly paraphenylenediamine in hair dyes and other ingredients that may be in fragrances or cosmetics.10 I patch test patients who fail to improve with conservative treatment methods, and I suspect that a lot of these patients may have low-level contact allergens that may not be picked up by a traditional patch test.
TREATMENT PEARLS AND PITFALLS
The Dermatologist: What is your typical approach to PIH and melasma in patients with Fitzpatrick IV to VI skin types?
Dr Asempa: The first thing is making sure that the patient has adequate photoprotection. In addition to religious broad-spectrum sunscreen application and using iron oxides like I mentioned earlier, I also recommend broad-brimmed hats, sun-protective clothing, and avoiding the sun at the hottest times of the day. However, many of my patients express concern that they will not get enough vitamin D if they protect themselves from the sun. While newer studies have shown an association between frequent high SPF application and modest reduction in vitamin D levels, the data on this are mixed and studies are ongoing. I explain to my patients that multiple systematic reviews emphasize sunscreen does not compromise vitamin D status under typical use.11-13
Patients also express concerns that they need sun exposure for their mood and overall happiness, and we do have a small amount of data validating these concerns.14-16 I help my patients understand that I am not saying the sun is necessarily all bad for them, but that they do need protection from it, which usually goes over better. I explain to them that the approved filters in the United States only confer protection for about 2 hours, so if they are out in the sun, they should consider setting an alarm on their phone for when it is time to reapply.
Another area of discussion is heat avoidance because a lot of people do not know that melasma can be triggered by heat, not just sunlight. I will have a patient tell me they were in the shade the entire time they were at the beach, but their condition still flared badly. So, I recommend little tips and tricks that can help such as having a personal fan handy.
My first-line treatment is always triple therapy, with hydroquinone, a topical steroid, and a retinoid for 3 months at a time typically, but there are studies that suggest you can go up to 6 continuous months with 4% hydroquinone.17-19 I have found clinically that going up to 6 months has been fine for my patients, with a 4- to 6-month break in between. And then we need to determine what the alternate agent is going to be. For some patients, it is oral tranexamic acid (TXA); for others, topical thiamidol, azelaic acid, cysteamine, or other agents. We always need to be thinking about all the treatments in our arsenal because with any hyperpigmentation condition, we will need multiple modalities.
The Dermatologist: How do you choose between first-line agents like hydroquinone, retinoids, and azelaic acid and newer therapies like TXA or thiamidol?
Dr Asempa: Oral TXA has gained a lot of recognition, and it works very well for melasma. However, we must think deeply about which patients we are giving it to. Patients who have a history of clotting disorders or active cancer are not candidates. Patients are often concerned about oral TXA because of clotting risk. However, we use much lower doses of oral TXA for melasma than are used to stop bleeding in surgery, for example. To my knowledge, there has only been one case report of someone who had a clotting event from the doses of oral TXA we use for melasma, and that patient was found to have a protein S deficiency, which led to their predisposition to clotting.20,21 Having the data on hand and being able to tell patients that TXA is effective and safe, with thromboembolic events being exceedingly rare, can help reassure them. So, I find that when I counsel them using the actual data, they are more likely to want to do it.
Thiamidol has been working well for a lot of patients and plays well with other ingredients, but I am not usually using it on its own, but rather in a routine with other ingredients.22,23
For patients with hyperpigmentation, cysteamine is another topical medication. The evidence is limited compared to oral TXA, and I find clinically that cysteamine has not been as effective in my hands as oral TXA or even thiamidol. However, the data show that cysteamine can be very helpful, so I always try it in the routines.24
It is important to note that irritation from our topical treatments for hyperpigmentation should be avoided at all costs, especially in patients with darker skin. Irritation can lead to further hyperpigmentation—a downward spiral. In an effort to develop and improve our topical treatments allowing for efficacy without
irritation, multiple studies have emerged investigating solid lipid nanocarriers to reduce irritation with ingredient delivery and liposomes to help enhance penetration of certain ingredients.25
For patients with EDP, LPP, pigmented contact dermatitis, and drug-induced hyperpigmentation, the above topical treatments are frequently ineffective. These patients are much more difficult to treat, and I think of them a bit differently. In addition to allergen avoidance and removal of potential offending drug agents, laser treatments, topical anti-inflammatory medications, and systemic agents such as dapsone or oral retinoids like isotretinoin or acitretin may be beneficial.
EVOLVING THERAPIES
The Dermatologist: Are there any emerging topical or oral agents you are excited about?
Dr Asempa: Right now, we are working on getting more data for TXA, cysteamine, and thiamidol, but I definitely think we need more treatment options. I do not think that we are anywhere near where we need to be. Treating hyperpigmentation is so multifactorial, and there is no silver bullet that is going to work in all cases. Even in patients with melasma, we cannot guarantee that they are going to be fully clear. For some patients, 5 minutes of too much sun can set them back. I have seen patients fully clear on treatment go on a single cruise and flare as though we had never treated them at all.
The Dermatologist: Do you use procedural treatments, such as peels, lasers, and microneedling, in your practice for hyperpigmentation? If so, how do you prepare patients for safe outcomes?
Dr Asempa: I do offer peels and lasers. I start with topicals for most of my patients. If they are not responding, or if they are responding and they need an extra boost, sometimes we will consider either a chemical peel that includes hydroquinone or glycolic acid or a laser regimen. Before starting a laser regimen, I often pretreat my patients with hydroquinone for 2 to 4 weeks and then do a test spot. For the test, I usually draw a circle and test in one area, seeing how the patient heals over the next 4 weeks. If the skin heals well without hyperpigmentation, then I proceed with the full treatment.
Laser treatment can be very helpful when the right device, setting, and patient is selected. Lasers to consider include 1927 nm fractional non-ablative lasers, low-fluence Q-switched 1064 nm Nd:YAG lasers, and 1064 nm picosecond Nd:YAG lasers, among others. I do not offer microneedling in my practice, but I do collaborate with colleagues who do, and they see improvement with using microneedling to help some of their topicals penetrate better.
Patients often ask for laser treatments expecting immediate results and clearance in one treatment. Extensive counseling is needed to help patients understand that multiple treatments will likely be required, which can be quite expensive. After going through the risks and benefits, most of my patients opt to start with topicals and then see what happens from there.
PERSONALIZED AND PREVENTIVE APPROACHES
The Dermatologist: What strategies do you recommend for preventing PIH in patients undergoing acne treatment or minor procedures
Dr Asempa: If I am going to do a laser treatment on a patient, I typically prescribe a 4-week pretreatment regimen. I should preface this by saying that data for pretreatment with hydroquinone is mixed, and benefit of pretreatment appears to depend on the specific type of laser treatment and patient population.26 In my clinical practice, I have seen great benefit from 4 weeks of a topical azelaic acid compound in the mornings with kojic acid and maybe some niacinamide, and then in the evenings, I have them use compounded hydroquinone with tretinoin and a topical steroid. Additionally, the patient should not have any recent sun exposure prior to the procedure.
The Dermatologist: How do behavioral counseling and lifestyle modification factor into long-term hyperpigmentation management?
Dr Asempa: Right now, we are not at a place where I can say to a patient, “Go on a cruise and just wear sunscreen, that will be enough.” I tell people the reason we now call it sunscreen and not sunblock is because it does not block 100% of the UV rays. Also, when you are sweating and in and out of the pool, we do not even know how much of it is truly on your skin for a long period of time. And then most people do not reapply every single 2 hours. This is frustrating for patients, but I walk them through all they can do to boost their protection. We discuss broad-brimmed hats and sun-protective clothing, how to keep the skin cool, oral and topical medications, and avoiding triggers as much as possible. But I do not want patients feeling like they cannot live their lives.
TRAINING AND EQUITY IN DERMATOLOGY
The Dermatologist: Many hyperpigmentation conditions are under-taught in traditional curricula. What gaps in training do you believe still need to be addressed?
Dr Asempa: In general, we need more images of patients with darker skin tones in all our training. We also need the American Board of Dermatology to continue to add more questions on the board exam that address these issues. And then we need to look at the cultural competency piece. Patients often present saying they did not attempt the regimen of a previous dermatologist because they were told the hyperpigmentation would be "treated later." However, when I review what has been prescribed, it is often a phenomenal regimen! When I explain how the regimen actually does address both things, they are often thrilled to do it. Building rapport and getting patient buy-in to the treatment plan is so important, and often starts with validating the patient's concerns and making sure they know those concerns are explicitly being addressed.
The Dermatologist: How do you think dermatologists can better center equity and cultural competency when treating patients with hyperpigmentation disorders?
Dr Asempa: Patients of color often feel like the medical community does a bad job of listening to them across the board, not just in dermatology. I think the biggest and most helpful thing you can do with any patient is simply listen to them. If the patient is concerned about something, it is worth being concerned about. I have had medical students presenting a patient to me, and they will say, the patient is worried about their hyperpigmentation, but the rash is gone, so I think we will just tell her it takes time. That is always the wrong answer; time does not make it better in many cases.
In terms of centering cultural competency and equity, the most important thing is that every patient who comes in gets listened to. If they are worried about it, I am worried about it, and I am going to address it. I may not be able to miraculously make them better, but I can tell them that we are going to keep trying and there is always another option. If it is safe, I am going to try it. The truth is, we have the tools and we have the knowledge, so we need to communicate that to our patients to make sure they feel listened to and cared for.
Conclusion
Hyperpigmentation disorders are rarely self-limited, often multifactorial, and deeply tied to patients’ emotional well-being, particularly for individuals with skin of color who face higher risk and longer disease courses. Effective management requires more than a single agent or procedure; it calls for early intervention, thoughtful combination therapy, rigorous photoprotection, and ongoing patient education grounded in trust and culturally competent care. While therapeutic gaps and unmet needs remain, dermatologists already have a growing and versatile armamentarium at their disposal. By listening closely to patients, validating their concerns, and committing to individualized, long-term strategies, clinicians can meaningfully reduce both the physical burden of hyperpigmentation and its psychosocial impact.
Disclosure: Dr Asempa has been a consultant or paid advisory board member for Arcutis, Pfizer, Regeneron, Sanofi, and Veradermics.
References:
-
Passeron T, Liu W, Morita A, et al. Pigmentary disorders around the world: self-reported prevalence and impact on QOL and social stigmatization. J Invest Dermatol. 2025;S0022-202X(25):03522-03525. doi:10.1016/j.jid.2025.10.598
-
Wang JY, Kabakova M, Philip R, Stolyar J, Berger-Gutierrez R, Jagdeo J. The impact of hyperpigmentation on the lives of patients. J Drugs Dermatol. 2025;24(7):668-674. doi:10.36849/JDD.8519
-
Dabas G, Vinay K, Parsad D, Kumar A, Kumaran MS. Psychological disturbances in patients with pigmentary disorders: a cross-sectional study. J Eur Acad Dermatol Venereol. 2020;34(2):392-399. doi:10.1111/jdv.15987
-
Abad-Casintahan F, Chow SK, Goh CL, et al. Frequency and characteristics of acne-related post-inflammatory hyperpigmentation. J Dermatol. 2016;43(7):826-828. doi:10.1111/1346-8138.13263
-
Chen W, Fang R, Zhang K, et al. Prevalence and associated factors of depression and anxiety among patients with melasma: a cross-sectional study in China. Front Psychiatry. 2025;16:1655781. doi:10.3389/fpsyt.2025.1655781
-
Zhu Y, Du X, Shen S, Song X, Xiang W. Body dysmorphic disorder symptoms in patients with melasma. Int J Dermatol. 2024;63(6):787-794. doi:10.1111/ijd.17013
-
Shah S, Baskaran N, Vinay K, Bishnoi A, Parsad D, Kumaran MS. Acquired dermal macular hyperpigmentation: an overview of the recent updates. Int J Dermatol. 2023;62(12):1447-1457. doi:10.1111/ijd.16859
-
Kumarasinghe SPW, Pandya A, Chandran V, et al. A global consensus statement on ashy dermatosis, erythema dyschromicum perstans, lichen planus pigmentosus, idiopathic eruptive macular pigmentation, and Riehl's melanosis. Int J Dermatol. 2019;58(3):263-272. doi:10.1111/ijd.14189
-
Vinay K, Bishnoi A, Parsad D, Saikia UN, Sendhil Kumaran M. Dermatoscopic evaluation and histopathological correlation of acquired dermal macular hyperpigmentation. Int J Dermatol. 2017;56(12):1395-1399. doi:10.1111/ijd.13782
-
Bishnoi A, Vinay K, Arshdeep, et al. Contact sensitization to hair colours in acquired dermal macular hyperpigmentation: results from a patch and photo-patch test study of 108 patients. J Eur Acad Dermatol Venereol. 2019;33(7):1349-1357. doi:10.1111/jdv.15576
-
Tran V, Duarte Romero BL, Andersen H, et al. Effect of daily sunscreen application on vitamin D: findings from the open-label randomized controlled Sun-D Trial. Br J Dermatol. 2025;193(6):1128-1137. doi:10.1093/bjd/ljaf310
-
Passeron T, Bouillon R, Callender V, et al. Sunscreen photoprotection and vitamin D status. Br J Dermatol. 2019;181(5):916-931. doi:10.1111/bjd.17992
-
Neale RE, Khan SR, Lucas RM, Waterhouse M, Whiteman DC, Olsen CM. The effect of sunscreen on vitamin D: a review. Br J Dermatol. 2019;181(5):907-915. doi:10.1111/bjd.17980
-
Luo CW, Chen SP, Chiang CY, et al. Association between ultraviolet B exposure levels and depression in Taiwanese adults: a nested case-control study. Int J Environ Res Public Health. 2022;19(11):6846. doi:10.3390/ijerph19116846
-
Toledo A, Karppinen T, Miettinen ME, et al. Narrow-band ultraviolet B (NB UV-B) exposures improve mood in healthy individuals differently depending on chronotype. Chronobiol Int. 2019;36(11):1570-1580. doi:10.1080/07420528.2019.1661424'
-
Cui Y, Gong Q, Huang C, et al. The relationship between sunlight exposure duration and depressive symptoms: a cross-sectional study on elderly Chinese women. PLoS One. 2021;16(7):e0254856. doi:10.1371/journal.pone.0254856
-
Grimes PE, Bhawan J, Guevara IL, et al. Continuous therapy followed by a maintenance therapy regimen with a triple combination cream for melasma. J Am Acad Dermatol. 2010;62(6):962-967. doi:10.1016/j.jaad.2009.06.067
-
Torok HM. A comprehensive review of the long-term and short-term treatment of melasma with a triple combination cream. Am J Clin Dermatol. 2006;7(4):223-230. doi:10.2165/00128071-200607040-00003
-
Chandra M, Levitt J, Pensabene CA. Hydroquinone therapy for post-inflammatory hyperpigmentation secondary to acne: not just prescribable by dermatologists. Acta Derm Venereol. 2012;92(3):232-235. doi:10.2340/00015555-1225
-
Lee HC, Thng TG, Goh CL. Oral tranexamic acid (TA) in the treatment of melasma: a retrospective analysis. J Am Acad Dermatol. 2016;75(2):385-392. doi:10.1016/j.jaad.2016.03.001
-
Feng X, Su H, Xie J. Efficacy and safety of tranexamic acid in the treatment of adult melasma: an updated meta-analysis of randomized controlled trials. J Clin Pharm Ther. 2021;46(5):1263-1273. doi:10.1111/jcpt.13430
-
Lekhavat C, Rojanamatin J, Suphannaphong M, Kolbe L. Efficacy and tolerability of 0.2% thiamidol cream for facial hyperpigmentation: a randomized, double-blind, and vehicle-controlled study. Dermatol Ther (Heidelb). 2026 Jan 21. doi:10.1007/ s13555-025-01649-y
-
Desai SR, Lain ET, Elbuluk N, Frey C. Clinical evaluation of thiamidol-containing formulations for the visual management of facial hyperpigmentation. J Drugs Dermatol. 2025;24(12):1195-1202. doi:10.36849/JDD.9517
-
Mawu FO, Christopher PM. Efficacy and safety of cysteamine 5% cream for the management of melasma: a systematic review and meta-analysis of randomized controlled trials. Arch Dermatol Res. 2024;317(1):117. doi:10.1007/s00403-024-03571-3
-
Aydin BS, Sagiroglu AA, Ozturk Civelek D, Gokce M, Bahadori F. Development of curcumin and turmerone loaded solid lipid nanoparticle for topical delivery: optimization, characterization and skin irritation evaluation with 3D tissue model. Int J Nanomedicine. 2024;19:1951-1966. doi:10.2147/IJN.S453347
-
Grimes PE. Management of hyperpigmentation in darker racial ethnic groups. Semin Cutan Med Surg. 2009;28(2):77-85. doi:10.1016/j.sder.2009.04.001