Reimagining Hidradenitis Suppurativa Care: Early Recognition, Therapeutic Innovation, and Multidisciplinary Care Across the Patient Journey
Hidradenitis suppurativa (HS) is increasingly recognized as a chronic, systemic inflammatory disease rather than an isolated cutaneous disorder. During an expert discussion featuring faculty from University of Texas Southwestern Medical Center and Brigham and Women’s Hospital at the 2026 Masterclasses in Dermatology Annual Meeting, speakers emphasized that improving outcomes in HS requires earlier recognition, reduction of diagnostic delay, coordinated referral systems, and integration of medical and surgical management across the disease continuum.
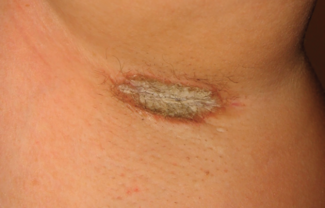
Diagnostic delay remains one of the most significant barriers to optimal care. On average, patients experience nearly a decade between symptom onset and formal diagnosis. During this period, many see multiple providers and receive several misdiagnoses before HS is correctly identified. The consequences are substantial. Patients often present with more severe disease, including extensive draining tunnels, hypertrophic scarring, and irreversible tissue destruction. Delayed diagnosis is also associated with a higher burden of comorbidities, chronic pain, impaired mobility, work disability, and profound reductions in quality of life. By the time specialty care is initiated, both physical and psychological sequelae may already be deeply entrenched.
HS is now understood to be a systemic inflammatory disease associated with numerous comorbid conditions. Inflammatory associations include arthritis and spondyloarthropathy, while endocrine and metabolic comorbidities include type 2 diabetes and polycystic ovarian syndrome. Psychiatric conditions, such as depression and anxiety, are highly prevalent, and metabolic syndrome has been reported in up to 50% of patients, conferring elevated cardiovascular risk. These data reinforce the need for comprehensive screening and longitudinal monitoring. Collaboration with primary care providers is essential, and many experts recommend spacing screening across visits to avoid overwhelming patients. Incorporating hemoglobin A1c and metabolic panels into routine biologic monitoring labs can improve efficiency. Given the chronic pain burden in HS, partnership with pain management specialists is also critical to reduce long-term opioid dependence and improve functional outcomes.
At University of Texas Southwestern Medical Center, a structured referral pathway has been developed to streamline care. Patients may enter the system through primary care, emergency departments, obstetrics/gynecology, gastroenterology, or rheumatology clinics. Once HS is suspected, referral to dermatology is prioritized, where disease severity is assessed and medical therapy initiated. Patients who do not require immediate surgical intervention can continue longitudinal medical management within the HS specialty clinic. When surgery is appropriate, dermatology and surgical teams collaborate closely to determine timing and optimize preoperative disease control. This structured approach has become a valuable resource for patients, helping them maximize the effectiveness of medical appointments and reducing fragmentation of care.
Therapeutic innovation has expanded substantially. As reviewed by Dr Alice Bendix Gottlieb, tumor necrosis factor (TNF)-α inhibition remains foundational. Adalimumab, the first US Food and Drug Administration approved biologic for HS, demonstrated significant Hidradenitis Suppurativa Clinical Response (HiSCR) responses in the PIONEER trials at week 12 compared with placebo. However, durability varies: approximately half of early responders may lose response by week 36 despite weekly dosing, whereas some initial nonresponders achieve response with continued therapy. Long-term extension data suggest sustained benefit in a subset of patients through 3 years. Infliximab, although used off label, remains an important option for severe disease. Administered intravenously at 10 mg/kg every 4 weeks, it is the only truly weight-based biologic option in HS and can be particularly useful in patients with high inflammatory burden.
Interleukin (IL)-17 pathway inhibition has further expanded treatment possibilities. Secukinumab, an IL-17A inhibitor, offers flexible dosing; in patients with inadequate response, dosing may be increased to every 2 weeks. Bimekizumab, a dual IL-17A/F inhibitor, demonstrated sustained high-level responses through 3 years in extension data from the BE HEARD trials, with durable HiSCR50, 75, and even 90 responses in many patients. A recent living systematic review and network meta-analysis comparing systemic therapies concluded that multiple cytokine inhibitors significantly outperform placebo, but most differences between active agents and adalimumab were not statistically definitive, underscoring the importance of individualized treatment selection rather than assuming a universally superior agent.
Emerging therapies in phase 2 and 3 development further illustrate the evolving landscape. Sonelokimab, an IL-17A/F nanobody, has demonstrated promising HiSCR75 responses. Brivekimig, a dual target nanobody directed at TNF and OX40 ligand, has shown encouraging efficacy signals. Remibrutinib, a Bruton’s tyrosine kinase inhibitor, is also under investigation. As targeted therapies expand, precision selection based on comorbidities, disease phenotype, and prior treatment response will likely become central to HS management.
Imaging is also reshaping clinical assessment. Dr Gottlieb emphasized the importance of ultrasound in detecting subclinical tunnels and abscesses that may not be visible on surface examination. Because draining tunnels are not fully captured in traditional outcome measures, ultrasound may identify patients with more severe disease than clinical scoring alone suggests and may influence earlier escalation of therapy.
Surgical management remains essential for select patients with persistent tunnels, fibrosis, or refractory disease. As discussed by Dr Dennis P. Orgill, the role of surgery has evolved in the biologic era. With improved systemic control, some previously extensive cases can now be managed with more limited procedures. Patients increasingly seek simpler surgeries with faster recovery. Options include unroofing, local tissue rearrangement, flaps, skin grafts, and innovative closure techniques such as negative pressure wound therapy–assisted approaches. However, surgery carries substantial risks, including wound dehiscence or infection rates approaching 20% in some series. Comorbidities, such as obesity, smoking, diabetes, Crohn’s disease, polycystic ovary syndrome, and psychiatric conditions, complicate surgical planning. Acute flares are generally avoided when scheduling procedures. Importantly, surgery does not cure HS, and most patients require continued dermatologic management postoperatively.
Patient narratives further highlight the systemic burden of HS. One patient described years of delayed diagnosis, later discovering comorbid type 2 diabetes and musculoskeletal symptoms. Tools such as the International Dermatology Outcome Measures Musculoskeletal Questionnaire have helped identify undiagnosed inflammatory joint disease in this population. Another patient, diagnosed in adolescence, underwent repeated emergency surgeries and antibiotic courses before receiving comprehensive HS care. Her disease progressed to multiple body sites, and over time she developed significant cardiovascular complications. Both patients emphasized that empathy, validation, and holistic management were transformative in reclaiming their identity beyond the disease.
Ultimately, shortening the journey to diagnosis begins with education. Increasing awareness among primary care providers, emergency physicians, obstetrician-gynecologists, and other frontline clinicians is essential. Recognizing recurrent nodules in intertriginous areas, appreciating associated comorbidities, and understanding referral pathways can dramatically alter disease trajectory. Equally important is how the initial visit is conducted. Experts stressed the importance of meeting the person, not just the condition; creating space for patients to share their experiences; and approaching care with empathy. When patients feel heard, clinicians gain the information necessary to guide effective, individualized treatment.
HS remains a challenging disease, particularly in severe cases. However, earlier recognition, structured referral systems, therapeutic innovation, integration of ultrasound assessment, and true collaboration between dermatology, surgery, primary care, pain management, and mental health professionals offer a path forward. A holistic, multidisciplinary approach is not optional; it is essential to improving long-term health, function, and quality of life for patients living with HS.
Reference
O’Brien J, Gottlieb AB, Orgill DP. Reimagining hidradenitis suppurativa care: early recognition, therapeutic innovation, and multidisciplinary care across the patient journey. Presented at: Masterclasses in Dermatology; February 19–22, 2026; Sarasota, FL.