Dermatomyositis: Interferon Biology, Steroid Dependence, and the Rise of JAK/TYK2 Targeting
At the 2026 Masterclasses in Dermatology Annual Meeting, Scott Elman, MD, and Victoria Werth, MD, delivered a comprehensive update on dermatomyositis (DM), emphasizing diagnostic accuracy, validated skin outcomes, and emerging steroid-sparing therapies.
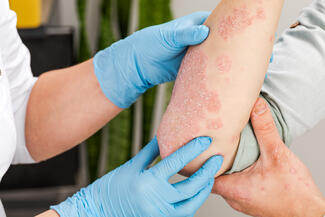
Dr Werth started with the clinical findings in the skin. Classic cutaneous findings—heliotrope rash, Gottron papules and sign, V-neck and shawl erythema, cuticular overgrowth, and inflammatory alopecia—remain central to diagnosis. However, “DM is frequently misdiagnosed as systemic or cutaneous lupus,” Dr Werth observed.
Pathogenetically, type I interferon (IFN) activation is a central driver of DM. “IFN-regulated chemokines aid in recruitment of CXCR3-positive cytotoxic lymphocytes to the dermal–epidermal junction,” leading to keratinocyte injury and sustained inflammation. Activation of the JAK/STAT pathway mediates interferon signaling, providing a rationale for targeted inhibition.
Dr Werth also touched base on the new ongoing European Alliance of Associations for Rheumatology/American College of Rheumatology myositis criteria project, evaluation of dermatomyositis, environmental triggers of DM, and outcomes in dermatomyositis.
Next, Dr Elman discussed evolving treatment strategies in the management of DM. Despite available therapies, dissatisfaction is high. Real-world data show that more than 60% of patients discontinue initial therapy within 1 year, and 73% report at least 1 disease flare annually. Nearly all patients report pain, and more than 50% describe negative social impact. Corticosteroids remain the cornerstone of therapy, reflecting limitations of current steroid-sparing options. Dr Elman emphasized that “type 1 interferon pathway activation is the central driver for DM.”
IVIG, US Food and Drug Administration approved in 2021, demonstrated meaningful cutaneous improvement, with more than 70% achieving greater than 35% Cutaneous Dermatomyositis Disease Area and Severity Index (CDASI)-A reduction at 28 weeks in post hoc analyses.
Dr Elman elaborated on what’s coming in treatments, which include “anti-interferon therapies (dazukibart, anifrolumab), JAK/TK2, and FcRn inhibitors (efgartigimod alfa-fcab).”
The dual JAK1/TYK2 inhibitor brepocitinib represents a promising advance. In a phase 2 open-label study of severe skin-predominant DM, all participants achieved CDASI-A improvements exceeding minimal clinically important differences by week 4. “The results really speak for themselves.” In the phase 3 VALOR trial (N=241), the primary endpoint—mean total improvement score at week 52—was met for brepocitinib 30 mg vs placebo (Δ 15.3; P=0.0006). Significant steroid tapering was achieved, and CDASI-A reductions were evident as early as week 4 and sustained through week 52. Cutaneous remission (CDASI-A ≤5) occurred more frequently with brepocitinib 30 mg than placebo (Δ 26.6%; P=0.0060). Adverse events of special interest occurred at similar rates across treatment arms. “The primary endpoint was met with clinically meaningful and consistent efficacy despite greater steroid tapering.”
Lastly, Dr Werth discussed the importance of interdisciplinary care in DM. “Multiple disciplines see patients with DM.” Interdisciplinary care is critical. “These collaborations allow for the optimal development of disease diagnostic and classification criteria, agreement on how to measure outcomes.”
Patients may present with skin-predominant disease or systemic involvement, including interstitial lung disease (25% of clinically amyopathic DM), malignancy risk, inflammatory arthritis, and neuropathy.
“Dermatomyositis is a multisystem disease involving skin, muscle, lungs, joints, nerves, gastrointestinal tract, and oncology in the case of paraneoplastic dermatomyositis. It is important to examine the patient carefully to determine the organs that are involved,” concluded Dr Werth. “The approach depends on which organs are involved, and the severity and responsiveness to treatment, but collaboration is important.”
For more meeting coverage, visit the Masterclasses in Dermatology newsroom.
Reference
Werth V, Elman S. Advances in dermatomyositis: the evolving landscape and potential role of novel therapies to improve disease outcomes. Presented at: Masterclasses in Dermatology; February 19–22, 2026; Sarasota, FL.