Application of Nanofiber Wound Dressings in Diabetic Wound Healing: A Review and Economic Considerations
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Wounds or HMP Global, their employees, and affiliates.
Abstract
Background. Electrospun nanofibers offer a promising solution in the treatment of diabetic wounds due to the technology’s ability to integrate a therapeutic agent, as well as its biodegradability, ability to act as a temporary extracellular matrix, and desirable wound dressing characteristics. Objective. To summarize existing literature on the use of nanofiber wound dressings in diabetic models. Methods. A scoping review was conducted to include literature investigating the application of nanofiber wound dressings loaded with a therapeutic modality in diabetic models. The query was developed using the PubMed Advanced Search Builder using key words and translated to the Embase syntax using the Embase Query Translator prior to searching both databases. Studies were excluded if they did not evaluate nanofibers as wound dressings or did not evaluate diabetic models. Results. Compared with the standard of care, nanofiber dressings loaded with antibiotics, anti-inflammatory agents, antioxidants, growth factors, and stem cells have demonstrated improved wound healing through infection control, inflammatory modulation, angiogenesis, cellular proliferation and migration, and minimized systemic adverse effects through localized drug release. Although no nanofiber wound dressing is currently commercially available, these dressings are promising in terms of cost-efficacy (despite the likely higher up-front cost) due to the potential for decreased hospital stays, amputations, and infection through accelerated wound healing. Conclusion. Electrospun nanofibers offer significant promise as a dressing for diabetic wound management; however, further studies are needed to evaluate the clinical efficacy and cost-effectiveness of such treatment.
The use of nanofiber dressings for diabetic wound healing is an emerging area of research; these dressings offering a biodegradable framework that mimics extracellular matrix (ECM), thus potentially enhancing the rate of wound healing.1,2 In addition to desirable wound dressing characteristics, nanofiber morphology, including pore size, fiber diameter, and polymer used, are easily tunable.1,2 Importantly, nanofibers provide a simple way to integrate small molecule drugs to allow for slow, sustained, localized release, thus preventing the adverse effects associated with systemic and traditional topical administration.3 Similarly, the release profile of the drugs is simple to adjust depending on desired characteristics.4,5 Nanofibers are a promising novel wound dressing with potential to accelerate wound healing, prevent or treat infection, and act as a scaffold for healing wounds. Application of these dressings to diabetic wounds may improve clinical outcomes and quality of life, making this an important area of research.
This review examines the current landscape of research into nanofiber dressings and discusses the implications of these novel dressings compared with the current standard of care.
Methods
A scoping review was conducted utilizing PubMed and Embase for studies published up until January 2025, including studies investigating nanofiber wound dressings loaded with a therapeutic agent in diabetic models. The search terms included diabetic wound, diabetic ulcer, diabetic foot ulcer, chronic wound, delayed wound healing, electrospun nanofiber, nanofiber scaffold, and electrospun mat. The query was developed using key words in conjunction with the now retired ChatGPT-4o model (OpenAI) following the PubMed Advanced Search Builder syntax. Studies were excluded if nanofibers were not used as a wound dressing, if the nanofiber dressings did not integrate a therapeutic agent, or if the study did not evaluate the therapy in a diabetic model.
Electrospun Nanofibers
Nanofiber scaffolds have excellent biocompatibility, provide continuous localized drug delivery, create an optimal microenvironment for wound healing, improve exudate absorption, have high porosity that allows for gas exchange, and block the invasion of microbes due to nanopore size exclusion, making nanofibers a good candidate for a singular treatment modality in diabetic wound healing.2 Local, controlled, and sustained drug delivery has the potential to improve wound healing. Systemic administration leads to potential off-target side effects, low bioavailability at the desired target, and poor selectivity. Compared with the currently available local drug delivery systems (hydrogels, films, sponges, and foams), nanofiber scaffolds are more convenient for the incorporation of therapeutic compounds, have hemostatic properties, have better conformation to wound surface due to flexibility, have less scar potential, and reduce the frequency of bandage changes.3 These beneficial properties can potentially improve patient compliance through enhanced comfort, the possibility of a superior cosmetic result, and decreased dedicated care time needed.
The unique properties of nanofiber wound dressings are derived from unique surface features resulting from the nanometer-diameter size, including enhanced mechanical strength and high surface-to-volume ratio.6 Studies incorporating therapeutics into nanofiber dressings have been applied in diabetic wound healing models, including murine and cell lines, yielding further healing benefit compared with nanofiber dressings alone.1,3,7 Uniquely, nanofiber dressings have tunable characteristics depending on the polymer type, the ratio or combination of polymers used, and the methods used to fabricate the nanofiber. This allows the nanofiber dressing to be adjusted to the desired drug release characteristics, making nanofiber dressings a great candidate for controlled drug release for a wide variety of therapeutics.8 Similarly, the rate of drug release and the mechanical properties can be modulated through chemical and physical crosslinking.4,5
Nanofiber dressings are fabricated by bioprinting, microfluidic spinning, wet spinning, dry spinning, and electrospinning.6 Electrospinning has frequently been used as a technique for development of nanofiber dressings for wound healing because of the high surface area–to-volume ratio, flexibility, simple preparation, wide material compatibility, ease of incorporation of therapeutic products, scalability, and easily tunable characteristics.6,8 In the electrospinning process, a polymer solution acts as a positive electrode directed at a negatively charged collector in the presence of a high electrical field and a very low flow rate of the fluid, generating a conical shaped jet known as a Taylor cone, creating a nanodiameter fiber mat.9,10 This process creates nonwoven mats of fiber size less than or equal to 1 µm with porous, solid, hollow, or core-shell structures in an aligned or random pattern.6
The electrospun nanofiber mat has structural and biological functions matching natural ECM properties, allowing it to act as a temporary scaffold during tissue healing, promoting cell adherence, multiplication, migration, and differentiation.2 The small pore size and large surface area are beneficial for hemostasis, favorable for exudate absorption, and useful for drug loading. The porosity of the electrospun nanofibers favors cellular respiration and gas permeation while preventing the wound from drying out and dehydrating.2 The nanoscale of the pore prevents microorganism invasion, ultimately inhibiting infection.2 These characteristics of electrospun nanofibers address some of the underlying dysregulation in poorly healing diabetic wounds. Nanofiber dressings transform into a hydrogel-like material upon contact with moisture, providing a moist yet breathable dressing due to the nanopore size as well as the ability to absorb wound exudate. Although products exist that achieve these goals individually, no current product contains all these characteristics. Nanofiber dressings can uniquely address the needs of wound healing through the host of beneficial effects of such dressings. Adjustment of nanofiber characteristics also creates a novel opportunity to adjust properties based on patient characteristics. Ultimately, electrospinning allows for a precise attenuation of morphology, porosity, fiber diameter, drug release profiles (depending on the polymer used), voltage applied, flow rate, and collector distance.11
Nanofiber application in diabetic wound healing
There is extensive literature on novel synthetic and natural polymers co-fabricated with existing or novel drugs applied to diabetic models both in vivo and in vitro. Generally, these preclinical studies show improved angiogenesis, collagen synthesis, fibroblast arrangement, and epithelialization.12 Drugs applied in nanofiber dressings commonly include antibiotics, inflammatory modulators, natural products, and novel drugs targeting the underlying pathogenesis of impaired healing in diabetic wounds (Table).
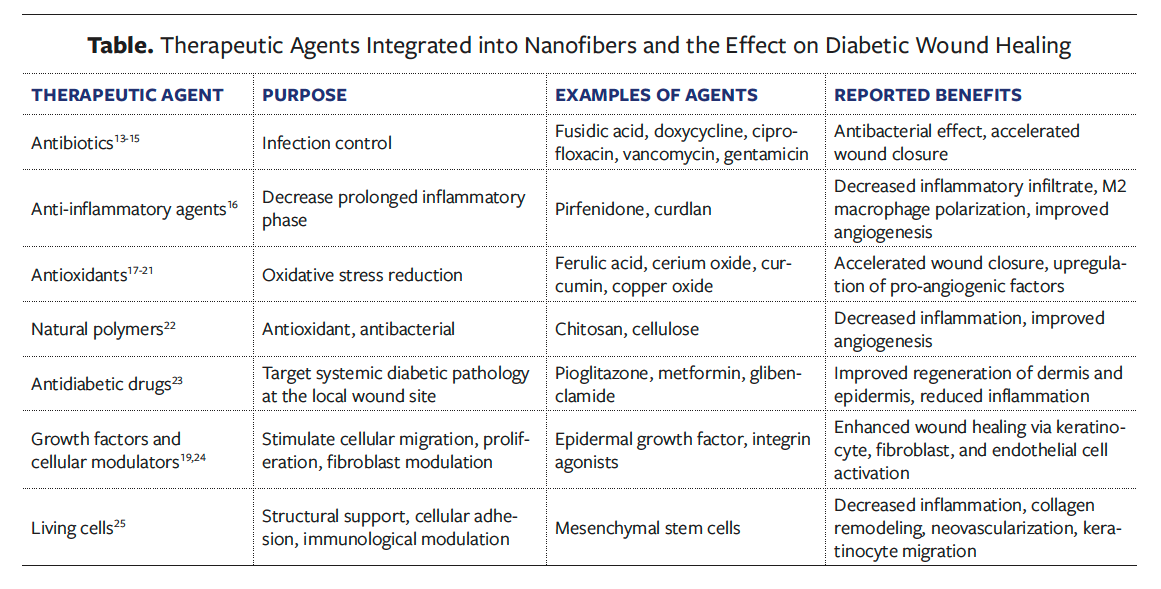
Nanofiber dressings loaded with antibiotics aim to address the concern of treating current infection and preventing new infection—one of the primary goals in wound healing. Various antibiotics have been integrated into nanofiber dressing, resulting in adequate antibacterial properties and improved wound healing in vivo.13-15 The modulation of release characteristics through adjustments to nanofiber fabrication specifications, polymer or polymers used, and postproduction processing make the integration of most known antibiotics simple and practical.
Inflammatory modulators aim to address the prolonged inflammatory phase in diabetic wound healing. Alzahrani et al16 addressed the pathogenesis with a 2-fold approach involving the use of both an antibacterial modulator (fusidic acid) and an anti-inflammatory modulator (pirfenidone), resulting in accelerated wound healing. Natural polymers, including chitosan and cellulose, inherently possess antioxidant and antibacterial properties, making them beneficial for integration into nanofiber dressings used for diabetic wound healing.14,17 The chemical properties of these natural polymers allow them to easily integrate with synthetic polymers for use in nanofiber dressings, making them a practical addition in nanofiber dressing preparations. Literature suggests that nanofiber dressings containing chitosan, synthetic polymer, and antioxidants integrated into polymer or used as the main polymer in fabrication improve wound healing with less inflammatory infiltration and increased angiogenesis.18 This mechanism allows for precision targeting of the diabetic wound pathophysiology.
Similarly, carbohydrate and synthetic combination nanofibers have been explored because of their ability to attenuate inflammation, biocompatibility, and immune modulation. One example is the polysaccharide curdlan, which stimulates macrophage polarization to the M2 phenotype in vitro and in vivo, producing favorable wound healing characteristics in diabetic models, including mature collagen and improved vascular maturity.19 Additionally, antioxidants, including ferulic acid, cerium oxide, curcumin, and copper oxide, have been loaded into nanofiber dressings as active ingredients, resulting in accelerated wound closure, with copper oxide in particular showing upregulation of proangiogenic factors.20-24 Inflammatory modulators target the inflammatory phase, which is essential to adequate wound healing progression and is highly dysregulated in diabetic wounds. In diabetic wounds, chronically elevated inflammation has a negative effect on wound healing, resulting in a prolonged inflammatory phase and the development of chronic wounds. The use of inflammatory modulators in nanofiber dressings has the potential to limit systemic adverse effects, decrease inflammation, and accelerate healing of diabetic wounds.
In addition, a bimodal approach utilizing drugs that target diabetic wound healing pathogenesis and nanofiber dressings facilitates an optimal healing environment. The integration of oral antidiabetic drugs pioglitazone, metformin, and glibenclamide into nanofibers has shown accelerated wound healing through improved regeneration of the dermis and epidermis, with less evidence of inflammation compared with controls.25 Similarly, fabrication of nanofiber dressings with GM18, an integrin agonist, modulated fibroblast activity to improve wound healing in diabetic models in vivo.26 The addition of epidermal growth factor into nanofiber dressing preparation also modulates healing through improved migration and proliferation of keratinocytes, fibroblasts, endothelial cells, and enhanced angiogenesis—vital steps in the proliferative and remodeling phases.22,27 Importantly, the integration of living mesenchymal stem cells into nanofiber dressings creates a living wound dressing, allowing for cellular adhesion, structural wound support, and immunological cell modulation.28 This methodology has been shown to improve diabetic wound healing through decreased inflammation, increased keratinocyte migration, neovascularization, and collagen remodeling.28,29 The unique ability to easily incorporate a variety of therapeutic agents into the nanofiber dressings provides the opportunity to easily adjust treatments to create individualized dressings for patients based on specific wound characteristics. This creates the novel opportunity to provide highly specific wound care treatments.
Nanofiber wound dressings have tremendous potential to target impaired physiology in diabetic wound healing, specifically by providing an optimal environment for wound healing. The structure allows for preferred wound dressing characteristics that target the dysregulation and disruption in diabetic wounds. This nanofiber structure has the potential to incorporate immunogenic modulators to target the underlying pathogenesis to then accelerate wound healing through improved cellular proliferation, angiogenesis, and collagen deposition.
Discussion and Future Direction
Previous in vivo and in vitro research has demonstrated improvement in diabetic wound models, warranting further investigation through clinical trials to determine the most efficacious combination of polymers and drugs.12 Nanofiber dressings alone, without drug integration, can augment wound healing through characteristics that have a positive effect on wound healing (eg, flexibility, moist yet breathable, infection protection, acting as temporary ECM).2,6 The addition of novel drugs targeting wound healing pathogenesis furthers the potential to improve outcomes.8
Nanofiber wound dressings can address adverse effects traditionally associated with topical and oral administration of drugs.2,30 The slow controlled release characteristics and polymer changes would allow for tunable release characteristics unique to patient needs, drug properties, and prevention of adverse effects.30 The ease of fabrication of nanofibers allows for the creation of unique dressings to address the needs of individual patients.6 Ease of modulation of nanofiber dressing characteristics opens new possibilities to tailor wound dressings for individualized wound care. Adjusting wound dressing specifications to meet individual needs has potential to accelerate wound healing, decrease health care spending, and improve quality of life, especially in the difficult to manage and burdensome disease state of diabetic wound healing.
Nanofiber dressings have the potential to reduce health care spending through decreased health care costs secondary to hospital stays, amputations, and chronic wound care, making the use of nanofiber dressings advantageous compared with standard dressings. For nanofiber dressing to be clinically feasible, the up-front cost of dressings must be low enough to justify the price, and risk reduction of complications must be both clinically and statistically significant. Currently, a cost-effectiveness analysis is not possible due to the lack of nanofiber wound dressings on the market. In future studies, such analysis will be important as nanofiber wound dressing products become available. The multitude of in vivo and in vitro studies showing promising results in diabetic models provide evidence that further investigation into nanofiber dressings is warranted.12 Importantly, the poor clinical outcomes with the current standard of care for diabetic wounds emphasizes the need for investigation into improved treatments.31,32
The aforementioned features of nanofibers and the vast need for an improved standard of care for diabetic wounds underscore the importance of further studies on nanofiber wound dressings, specifically randomized controlled trials.31,33-35 There is also an impetus to experimentally compare different drug types loaded into nanofiber scaffolds to determine which therapeutic approaches have superior promise and efficacy in improving wound healing.36 Advancing nanofiber wound dressings toward clinical adoption requires collaboration between researchers, regulatory agencies, and collaborative public and private partnerships providing funding. Future studies should be adequately powered and should focus on the clinically meaningful end points, including wound closure time, infection rates, hospitalization rates, amputations, and, importantly, patient-reported quality of life outcomes. This process could be accelerated through the standardization of fabrication processes and nanofiber dressing benchmarks to facilitate reproducibility and improve comparisons across studies. With the potential for a high-impact improvement in patient care, collaboration between researchers and regulatory bodies (eg, US Food and Drug Administration) to clarify required safety and efficacy data for this emerging technology would remove another barrier to moving this technology to the next phases. Finally, increased investment from federal organizations, support from the American Diabetes Association, and public-private partnerships would provide valuable resources to accelerate this translational research, particularly given the high clinical need and potential for cost savings.
Limitations
This scoping review has limitations. Most of the studies included in this review are preclinical, which may not fully represent outcomes in human diabetic wound healing. Similarly, polymer type, fabrication methods, and evaluation metrics vary between studies, which limits direct comparison between studies. These studies may also be influenced by publication bias favoring positive outcomes and the lack of long-term longitudinal data. Finally, the narrative scoping nature of this review limits comprehensiveness and reproducibility.
Conclusion
Chronic diabetic wounds place a significant burden on health care spending and patient quality of life, while disproportionately affecting underresourced groups. Lack of adequate treatments addressing the underlying pathogenesis of diabetic wounds and high complication rates make further research into wound dressings essential to improving morbidity and mortality of patients with diabetes.
Nanofiber wound dressings offer a solution to the difficulties of traditional wound dressings through incorporation of drugs targeting underlying pathophysiology, customizable features, and immunologically desirable characteristics. Current evidence in diabetic models suggests that nanofiber wound dressings accelerate wound contraction, thus providing support for future randomized controlled trials to assess the wound healing potential of this technology. Although up-front costs may be cost prohibitive, nanofiber wound dressings provide a solution to the substantial problem of impaired healing in patients with diabetes.
Author and Public Information
Authors: Gemma Toogood, BS1; Harrison Smith, BS1; Meghan Underwood, BS1; Robin Evans, MD2; and Junwang Xu, PhD1
Affiliations: 1Department of Physiology, College of Medicine, The University of Tennessee Health Science Center, Memphis, TN, USA; 2Division of Plastic and Reconstructive Surgery, College of Medicine, The University of Tennessee Health Science Center, Memphis, TN, USA
Funding: The authors received no financial support for this work.
Disclosures: The authors disclose no relevant financial or nonfinancial interests.
Ethical Approval: No ethical approval was required because this is a scoping review article.
Correspondence: Junwang Xu, PhD; UTHSC Department of Physiology, 71 S Manassas St Room 307, Memphis, TN 38163; jxu61@uthsc.edu
Manuscript Accepted: January 30, 2026
References
1. Chong C, Wang Y, Maitz PK, Simanainen U, Li Z. An electrospun scaffold loaded with anti-androgen receptor compound for accelerating wound healing. Burns Trauma. 2013;1(2):95-101. doi:10.4103/2321-3868.118935
2. Liu Y, Li C, Feng Z, Han B, Yu DG, Wang K. Advances in the Preparation of Nanofiber Dressings by Electrospinning for Promoting Diabetic Wound Healing. Biomolecules. Nov 22 2022;12(12)doi:10.3390/biom12121727
3. Jannesari M, Varshosaz J, Morshed M, Zamani M. Composite poly(vinyl alcohol)/poly(vinyl acetate) electrospun nanofibrous mats as a novel wound dressing matrix for controlled release of drugs. Int J Nanomedicine. 2011;6:993-1003. doi:10.2147/IJN.S17595
4. El-Lakany SA, Kamoun EA, Abd-Elhamid AI, Aly RG, Samy WM, Elgindy NA. Graphene oxide crosslinked-zein nanofibrous scaffolds for prominent Cu-adsorption as tissue regeneration promoters in diabetic rats: Nanofibers optimization and in vivo assessment. Int J Pharm. Nov 30 2020;590:119919. doi:10.1016/j.ijpharm.2020.119919
5. Fadlallah S, Tabary N, Noel S, et al. Synthesis of novel catalytic composite nanofibers containing ruthenium nanoparticles stabilized by a citric acid-beta-cyclodextrin polymer. Nanoscale Adv. May 19 2020;2(5):2087-2098. doi:10.1039/c9na00791a
6. Kong B, Liu R, Guo J, Lu L, Zhou Q, Zhao Y. Tailoring micro/nano-fibers for biomedical applications. Bioact Mater. Jan 2023;19:328-347. doi:10.1016/j.bioactmat.2022.04.016
7. Mostafa DA, Hashad AM, Abou El-Ezz D, Ragab MF, Khalifa MKA. Electrospun PVA nanofiber mat for topical Deflazacort delivery: accentuated anti-inflammatory efficacy for wound healing. Pharm Dev Technol. Nov 2023;28(9):884-895. doi:10.1080/10837450.2023.2270057
8. Feng X, Li J, Zhang X, Liu T, Ding J, Chen X. Electrospun polymer micro/nanofibers as pharmaceutical repositories for healthcare. J Control Release. May 28 2019;302:19-41. doi:10.1016/j.jconrel.2019.03.020
9. Kamoun EA, Loutfy SA, Hussein Y, Kenawy ES. Recent advances in PVA-polysaccharide based hydrogels and electrospun nanofibers in biomedical applications: A review. Int J Biol Macromol. Sep 30 2021;187:755-768. doi:10.1016/j.ijbiomac.2021.08.002
10. Morad MR, Rajabi A, Razavi M, Sereshkeh SR. A Very Stable High Throughput Taylor Cone-jet in Electrohydrodynamics. Sci Rep. Dec 5 2016;6:38509. doi:10.1038/srep38509
11. Teixeira MA, Amorim MTP, Felgueiras HP. Poly(Vinyl Alcohol)-Based Nanofibrous Electrospun Scaffolds for Tissue Engineering Applications. Polymers (Basel). Dec 18 2019;12(1)doi:10.3390/polym12010007
12. de Souza A, Santo GE, Amaral GO, et al. Electrospun skin dressings for diabetic wound treatment: a systematic review. J Diabetes Metab Disord. Jun 2024;23(1):49-71. doi:10.1007/s40200-023-01324-z
13. Cui S, Sun X, Li K, et al. Polylactide nanofibers delivering doxycycline for chronic wound treatment. Mater Sci Eng C Mater Biol Appl. Nov 2019;104:109745. doi:10.1016/j.msec.2019.109745
14. Abdel Khalek MA, Abdel Gaber SA, El-Domany RA, El-Kemary MA. Photoactive electrospun cellulose acetate/polyethylene oxide/methylene blue and trilayered cellulose acetate/polyethylene oxide/silk fibroin/ciprofloxacin nanofibers for chronic wound healing. Int J Biol Macromol. Dec 15 2021;193(Pt B):1752-1766. doi:10.1016/j.ijbiomac.2021.11.012
15. Lee CH, Liu KS, Cheng CW, et al. Codelivery of Sustainable Antimicrobial Agents and Platelet-Derived Growth Factor via Biodegradable Nanofibers for Repair of Diabetic Infectious Wounds. ACS Infect Dis. Oct 9 2020;6(10):2688-2697. doi:10.1021/acsinfecdis.0c00321
16. Alzahrani DA, Alsulami KA, Alsulaihem FM, et al. Dual Drug-Loaded Coaxial Nanofiber Dressings for the Treatment of Diabetic Foot Ulcer. Int J Nanomedicine. 2024;19:5681-5703. doi:10.2147/ijn.S460467
17. Ahmed R, Tariq M, Ali I, et al. Novel electrospun chitosan/polyvinyl alcohol/zinc oxide nanofibrous mats with antibacterial and antioxidant properties for diabetic wound healing. Int J Biol Macromol. Dec 2018;120(Pt A):385-393. doi:10.1016/j.ijbiomac.2018.08.057
18. Chen Q, Wu J, Liu Y, et al. Electrospun chitosan/PVA/bioglass Nanofibrous membrane with spatially designed structure for accelerating chronic wound healing. Mater Sci Eng C Mater Biol Appl. Dec 2019;105:110083. doi:10.1016/j.msec.2019.110083
19. Chen Y, Bera H, Si L, et al. Tailor-made curdlan based nanofibrous dressings enable diabetic wound healing. Carbohydr Polym. Jan 15 2025;348(Pt B):122876. doi:10.1016/j.carbpol.2024.122876
20. Alizadeh S, Samadikuchaksaraei A, Jafari D, et al. Enhancing Diabetic Wound Healing Through Improved Angiogenesis: The Role of Emulsion-Based Core-Shell Micro/Nanofibrous Scaffold with Sustained CuO Nanoparticle Delivery. Small. Jun 2024;20(24):e2309164. doi:10.1002/smll.202309164
21. Anand S, Pandey P, Begum MY, et al. Electrospun Biomimetic Multifunctional Nanofibers Loaded with Ferulic Acid for Enhanced Antimicrobial and Wound-Healing Activities in STZ-Induced Diabetic Rats. Pharmaceuticals (Basel). Feb 28 2022;15(3)doi:10.3390/ph15030302
22. Augustine R, Hasan A, Dalvi YB, et al. Growth factor loaded in situ photocrosslinkable poly(3-hydroxybutyrate-co-3-hydroxyvalerate)/gelatin methacryloyl hybrid patch for diabetic wound healing. Mater Sci Eng C Mater Biol Appl. Jan 2021;118:111519. doi:10.1016/j.msec.2020.111519
23. Agarwal Y, Rajinikanth PS, Ranjan S, et al. Curcumin loaded polycaprolactone-/polyvinyl alcohol-silk fibroin based electrospun nanofibrous mat for rapid healing of diabetic wound: An in-vitro and in-vivo studies. Int J Biol Macromol. Apr 15 2021;176:376-386. doi:10.1016/j.ijbiomac.2021.02.025
24. Ghosh A, Saha K, Bhattacharya T, et al. Electrospun Cerium Oxide Nanoparticle/Aloe Vera Extract-Loaded Nanofibrous Poly(Ethylene Oxide)/Polyurethane Mats As Diabetic Wound Dressings. ACS Appl Bio Mater. Aug 19 2024;7(8):5268-5278. doi:10.1021/acsabm.4c00475
25. Cam ME, Ertas B, Alenezi H, et al. Accelerated diabetic wound healing by topical application of combination oral antidiabetic agents-loaded nanofibrous scaffolds: An in vitro and in vivo evaluation study. Mater Sci Eng C Mater Biol Appl. Feb 2021;119:111586. doi:10.1016/j.msec.2020.111586
26. Baldassarro VA, Giraldi V, Giuliani A, et al. Poly(l-lactic acid) Scaffold Releasing an α(4)β(1) Integrin Agonist Promotes Nonfibrotic Skin Wound Healing in Diabetic Mice. ACS Appl Bio Mater. Jan 16 2023;6(1):296-308. doi:10.1021/acsabm.2c00890
27. Choi JS, Leong KW, Yoo HS. In vivo wound healing of diabetic ulcers using electrospun nanofibers immobilized with human epidermal growth factor (EGF). Biomaterials. Feb 2008;29(5):587-96. doi:10.1016/j.biomaterials.2007.10.012
28. Gao S, Chen T, Wang Z, et al. Immuno-activated mesenchymal stem cell living electrospun nanofibers for promoting diabetic wound repair. J Nanobiotechnology. Jun 21 2022;20(1):294. doi:10.1186/s12951-022-01503-9
29. Chen S, Wang H, Su Y, et al. Mesenchymal stem cell-laden, personalized 3D scaffolds with controlled structure and fiber alignment promote diabetic wound healing. Acta Biomater. May 2020;108:153-167. doi:10.1016/j.actbio.2020.03.035
30. Singh A, Rath G, Singh R, Goyal AK. Nanofibers: An Effective Tool for Controlled and Sustained Drug Delivery. Curr Drug Deliv. Feb 14 2018;15(2):155-166. doi:10.2174/1567201814666171002115230
31. Everett E, Mathioudakis N. Update on management of diabetic foot ulcers. Ann N Y Acad Sci. Jan 2018;1411(1):153-165. doi:10.1111/nyas.13569
32. Dasari N, Jiang A, Skochdopole A, et al. Updates in Diabetic Wound Healing, Inflammation, and Scarring. Semin Plast Surg. Aug 2021;35(3):153-158. doi:10.1055/s-0041-1731460
33. Hingorani A, LaMuraglia GM, Henke P, et al. The management of diabetic foot: A clinical practice guideline by the Society for Vascular Surgery in collaboration with the American Podiatric Medical Association and the Society for Vascular Medicine. J Vasc Surg. Feb 2016;63(2 Suppl):3s-21s. doi:10.1016/j.jvs.2015.10.003
34. Lipsky BA, Berendt AR, Cornia PB, et al. 2012 Infectious Diseases Society of America clinical practice guideline for the diagnosis and treatment of diabetic foot infections. Clin Infect Dis. Jun 2012;54(12):e132-73. doi:10.1093/cid/cis346
35. Rice JB, Desai U, Cummings AK, Birnbaum HG, Skornicki M, Parsons NB. Burden of diabetic foot ulcers for medicare and private insurers. Diabetes Care. 2014;37(3):651-8. doi:10.2337/dc13-2176
36. Chen P, Vilorio NC, Dhatariya K, et al. Guidelines on interventions to enhance healing of foot ulcers in people with diabetes (IWGDF 2023 update). Diabetes Metab Res Rev. Mar 2024;40(3):e3644. doi:10.1002/dmrr.3644