Negative Pressure Wound Therapy-Assisted Granulation and Grafting Over Exposed Achilles Tendon in an Immunocompromised Burn Patient
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Wounds or HMP Global, their employees, and affiliates.
Abstract
Background. Management of full-thickness burns over the Achilles tendon is a significant challenge due to poor vascularity, which limits granulation tissue formation and successful grafting. This is even more difficult in patients undergoing chemotherapy, whose wound healing is further compromised due to delayed cell division, migration, and angiogenesis. Case report. A 44-year-old male undergoing chemotherapy for retrobulbar glioma sustained a full-thickness scald burn to the entire lower limb below the knee. Despite multiple tangential excisions and successful grafting over most areas, the Achilles tendon remained exposed and necrotic, with no granulation tissue formation. After debridement of the necrotic tendon followed by 2 longitudinal slit incisions until bleeding was noted, a negative pressure wound therapy device was applied at −125 mm Hg. Dressing changes were done every 3 days for 2 weeks until the tendon was fully covered by granulation tissue. A 10-cm × 5-cm split-thickness mesh skin graft was then applied over the Achilles region, which fully adhered within 1 week. Conclusion. The combination of longitudinal slit incisions of the Achilles tendon and negative pressure wound therapy can enhance adequate granulation over an exposed Achilles tendon, offering a practical and effective alternative to flap coverage in immunocompromised patients.
Accounting for nearly one-sixth of body weight, the skin represents the largest organ in humans.1 The skin is essential for physiological balance and provides a first line of defense against environmental factors.1 The skin is composed of different layers (epidermis, dermis, hypodermis), each with its own component and function. The top layer is the epidermis, which acts as a protective barrier and makes new skin. In contrast, the dermis is a relatively thick layer measuring 1 mm to 4 mm that is made up of an extracellular matrix abundant in collagen that serves to maintain the structural integrity of the epidermis and supplies nutrients to its viable layers.2 The primary functions of the dermis include thermoregulation, maintenance of hydration, and support of the overlying epidermis.2 The final layer is the hypodermis, a fatty layer of loose connective tissue that functions as a cushion for muscle and bone that provides protection during falls. The integrity of all the layers of skin is vital to overall health, and multilayer injuries such as burns, surgical procedures, and trauma can cause disablement and severe emotional distress.1 One injury that may affect skin integrity is burn injury. According to the World Health Organization, approximately 11 million people sustain burn injuries each year, with an estimated 180,000 deaths.3 Burns result from exposure to chemicals, electrical currents, heat, or other injurious agents that cause tissue damage. While the skin is most affected, deeper structures such as muscles and bones may also be involved,3 which increases susceptibility to infection—a major cause of mortality and morbidity in hospitalized burn patients.4
Burns are classified according to the depth of skin involvement as first degree (superficial), second degree (partial thickness), or third degree (full thickness). Management strategies differ for each degree. However, split-thickness skin grafting has traditionally been the standard treatment for extensive full-thickness burns.5 Although they are effective in achieving wound closure, these grafts are frequently associated with complications such as visible scarring, xerosis, pruritus, pain, pigmentary changes, and altered sensation. Therefore, the most suitable option for managing full-thickness skin defects is restoration using healthy, intact full-thickness skin.5
Management of full-thickness burn over a tendon, such as the Achilles tendon, presents a significant challenge for plastic surgeons, particularly when the tendon is exposed. Because the Achilles tendon lacks robust vascularity and spontaneous granulation, effective grafting over this area is unlikely without the use of advanced techniques such as negative pressure wound therapy (NWPT), in which an open cell sponge tailored to the wound dimensions is covered with an occlusive polyurethane membrane, and negative pressure is applied to promote perfusion and enhance granulation tissue formation.6
These challenges are further compounded in immunocompromised patients, such as those who receive chemotherapy that impairs the pathways involved in wound healing by inhibiting and delaying cell division, cell migration, and angiogenesis,7 all of which are essential to granulation and graft survival.
Several techniques have been developed to promote healing over exposed tendons, including local flap, cross-leg flap, free flap,8 and split-thickness flap with NPWT. The outcomes in oncology patients remain unpredictable, however. Despite their critical role in lower extremity reconstruction, free flaps are associated with several disadvantages, such as donor site morbidity, flap bulk requiring secondary contouring, and technical demands of microvascular anastomosis.
The authors present the case of an immunocompromised patient with full-thickness burn injury with exposed Achilles tendon who was treated with longitudinal slit incision of that tendon followed by NPWT to promote granulation tissue formation and enable grafting.
Case Report
The patient provided written informed consent to publish details and photographs of his case.
A 44-year-old male with known retrobulbar glioma tumor who was undergoing chemotherapy was admitted to the emergency department with a full-thickness scald burn caused by hot water thermal injury while bathing. The burn involved the entire left lower limb area below the knee and was managed as an emergency case requiring admission to the burn unit.
After 2 weeks of admission, the patient underwent a total of 4 tangential excision debridement procedures 1 week apart, until granulation tissue covered the whole lower limb except for the Achilles tendon area. That tendon was exposed and partially covered by necrotic tissue, with no granulation formation (Figure 1).
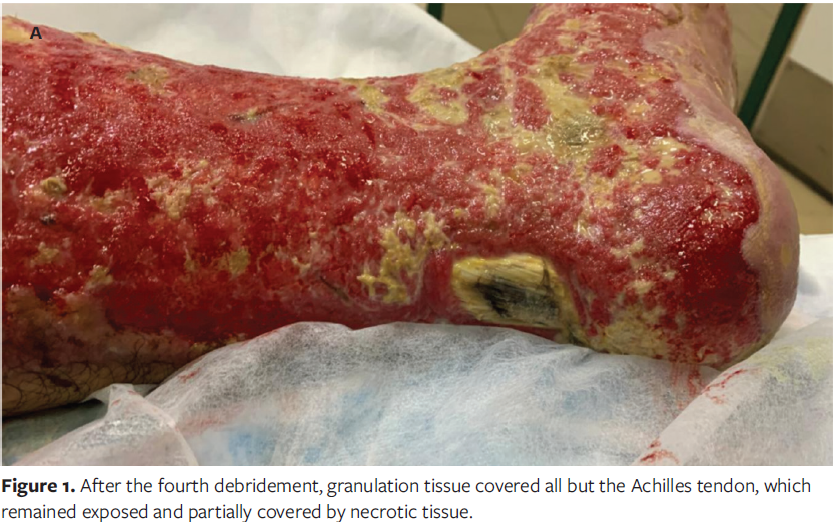
During the hospital admission period, the patient received intravenous ceftriaxone 500 mg twice daily until the day of grafting, omeprazole 20 mg orally once daily until full recovery, and pain reliever 1 g as needed until full recovery. For wound care, silver sulfadiazine 1% topical cream was applied and the dressing changed every 12 hours for 5 days, after which nitrofurazone was used until the NPWT device was applied.
Grafting was performed in 2 separate sessions for the whole granulation tissue area of the lower limb, except for the exposed Achilles tendon, to allow the area surrounding the Achilles tendon to heal, thus providing a good adherence surface for NPWT dressing. In a third, separate session, debridement of necrotic tendon was performed before making 2 longitudinal slit incisions of the Achilles tendon until bleeding from deeper layers was observed. An NPWT device was applied at negative pressure of −125 mm Hg and was maintained for 2 weeks with dressing changes every 3 days until the wound area was totally covered by granulation tissue (Figure 2).
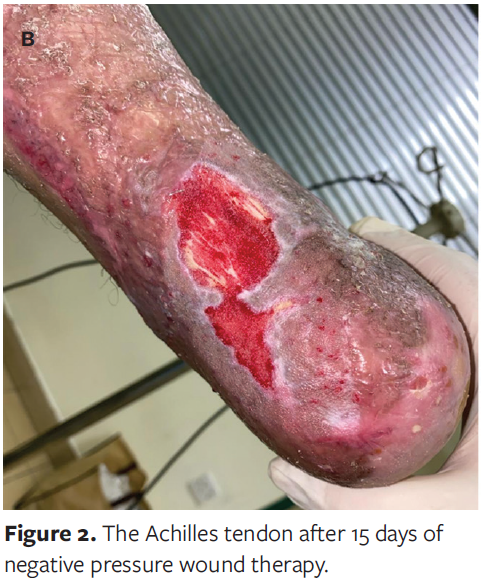
Following this intervention, a 10-cm × 5-cm split-thickness mesh skin graft harvested from the patient’s contralateral thigh was successfully applied over the Achilles region. After 1 week, the graft fully adhered and survived, and the patient was discharged from the hospital. The patient remained in the burn unit for a total of 4 months from admission until discharge. Six months after split-thickness mesh skin grafting, the patient was followed up in the clinic (Figure 3).
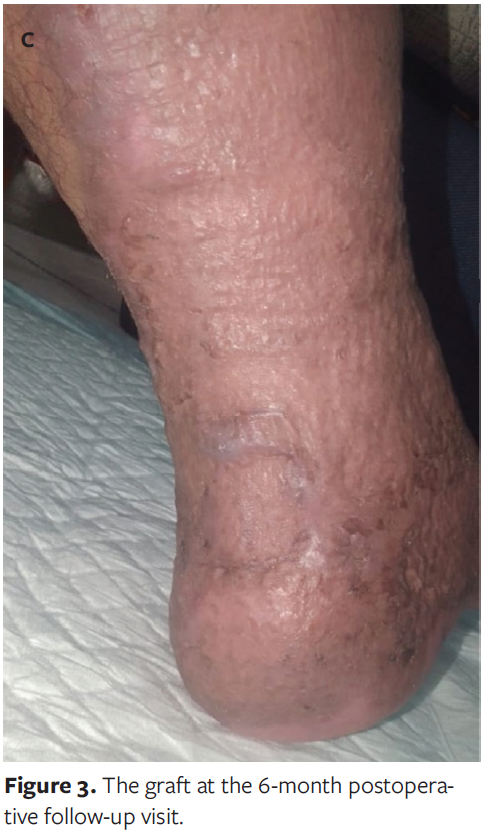
Discussion
The wound healing process has several phases: hemostasis and inflammation, proliferation, and remodeling.9 The hemostasis stage, which lasts for minutes, begins with endothelium injury of the vessel wall and terminates with formation and breakdown of a fibrin clot. The inflammation phase begins after hemostasis and lasts for 3 days to 5 days. The proliferation phase is triggered by growth factor signaling during the inflammatory phase and can last up to 2 weeks. This stage is characterized by wound surface epithelialization, formation of granulation tissue, and angiogenesis, which partially restore the defect created by the injury. The final stage, remodeling, may last 1 year to 2 years and results in scar formation composed of organized collagen. However, the scar achieves only about 50% to 80% of the tensile strength of normal tissue.9
The management of full-thickness burn over the Achilles tendon is particularly complex due to low vascularity, which limits the ability for granulation and graft acceptance.6 Several techniques have been developed to promote healing over exposed tendons, including local flap, cross-leg flap, and free flap,8 but NPWT has emerged as an effective alternative for promoting tissue over the exposed tendon by enhancing local perfusion, angiogenesis, and granulation.6
Skin grafting over exposed tendons is often challenging due to the tendon’s limited vascularity, particularly in the absence of paratenon. Without a well-
vascularized bed, the graft take will be poor, increasing the risk of graft failure. In such cases coverage with vascularized tissue such as muscle or fasciocutaneous flap is preferred to create a suitable environment for graft survival and wound healing.
The approach for the patient in the present case report, who underwent chemotherapy (which significantly impairs wound healing), consisted of performing a longitudinal tendon-slitting technique to allow internal bleeding and granulation on the avascular tendon surface, followed by 2 weeks of NPWT until healthy granulation tissue formed over the Achilles tendon, and finally, successful application of graft.
Whereas most other literature on NPWT focuses on immunocompetent patients, the present case demonstrates that, with proper technique and timing, successful granulation and grafting can also be achieved in immunocompromised patients, thus avoiding the need for complex procedures.
One notable case in the literature demonstrated successful split-thickness skin grafting for a 70-year-old male with type 2 diabetes who presented with necrosis of the Achilles tendon secondary to soft tissue infection. After debridement of necrotic tissue, a longitudinal slit incision of the Achilles tendon was performed. Then a mobile NPWT device set to continuous negative pressure at −80 mm Hg was used, with dressing changes twice a week. A complete granulation area appeared on the tendon within 6 weeks to 8 weeks.10
Limitations
This report describes the outcome of a single patient, which limits the generalizability of the findings. No comparison was made with other reconstructive options such as local or free flaps; thus, the relative efficacy of this approach remains uncertain. The follow-up period, although sufficient to confirm initial graft survival, is inadequate to assess long-term tendon integrity, function, or recurrence risk. Additionally, because of the patient’s immunocompromised status due to chemotherapy, wound healing outcomes in this case may differ from other populations. Finally, the technique described requires surgical expertise and access to NPWT, which may not be available in all burn care settings.
Conclusion
Management of full-thickness burns with exposed Achilles tendons remains a surgical challenge, particularly in immunocompromised patients. The present case demonstrates that combining longitudinal slit incisions of the tendon with NPWT can promote adequate granulation tissue formation and allow successful grafting without the need for flap coverage. This technique offers a practical and less invasive alternative in selected high-risk patients for whom traditional reconstructive options may be limited.
Author and Public Information
Authors: Mohamad Kharashgah, MBBS1; Qusai Nabeel Swedan, MD2; and Saleh Abualhaj, MD3,4
Affiliations: 1Department of General Surgery and Anesthesia, Faculty of Medicine, Yarmouk University, Irbid, Jordan; 2Ministry of Health, Amman, Jordan; 3General Surgery Department, Faculty of Medicine, Al-Balqa Applied University, Al-Salt, Jordan; 4Surgery Department, King Hussein Cancer Center, Amman, Jordan
Author Contributions: All authors contributed equally to conceptualization, data collection, drafting of the manuscript, and manuscript revision.
Acknowledgments: The authors wish to thank the nursing staff of the burn unit at Princess Basma Hospital, Irbid, Jordan.
Disclosures: The authors have no relevant financial or nonfinancial interests to disclose.
Data Availability: Data are available from the corresponding author upon reasonable request.
Ethical approval: Written informed consent was obtained from the patient.
Correspondence: Qusai Nabeel Swedan, MD; Faculty of Medicine, Yarmouk University, Shafiq Irshidat st., Irbid, Jordan Al-Huson, 21510, Irbid, Jordan; qusaii.swidan@gmail.com
Manuscript Accepted: December 15, 2025
References
1. Al Mamun A, Shao C, Geng P, Wang S, Xiao J. Recent advances in molecular mechanisms of skin wound healing and its treatments. Front Immunol. 2024;15:1395479. doi:10.3389/fimmu.2024.1395479
2. Bouwstra JA, Nădăban A, Bras W, McCabe C, Bunge A, Gooris GS. The skin barrier: an extraordinary interface with an exceptional lipid organization. Prog Lipid Res. 2023;92:101252. doi:10.1016/j.plipres.2023.101252
3. Radzikowska-Büchner E, Łopuszyńska I, Flieger W, Tobiasz M, Maciejewski R, Flieger J. An overview of recent developments in the management of burn injuries. Int J Mol Sci. 2023;24(22):16357. doi:10.3390/ijms242216357
4. Ladhani HA, Yowler CJ, Claridge JA. Burn wound colonization, infection, and sepsis. Surg Infect (Larchmt). 2021;22(1):44-48. doi:10.1089/sur.2020.346
5. Palmieri TL. Emerging therapies for full-thickness skin regeneration. J Burn Care Res. 2023;44(Suppl 1):S65-S67. doi:10.1093/jbcr/irac102
6. Heugel JR, Parks KS, Christie SS, Pulito JF, Zegzula DH, Kemalyan NA. Treatment of the exposed Achilles tendon using negative pressure wound therapy: a case report. J Burn Care Rehabil. 2002;23(3):167-171. doi:10.1097/00004630-200205000-00005
7. Słonimska P, Sachadyn P, Zieliński J, Skrzypski M, Pikuła M. Chemotherapy-mediated complications of wound healing: an understudied side effect. Adv Wound Care (New Rochelle). 2024;13(4):187-199. doi:10.1089/wound.2023.0097
8. Ohata E, Yuzuriha S, Mishima Y, Matsuo K. Longitudinal slit procedure in addition to negative pressure wound therapy for a refractory wound with exposed Achilles tendon. Eplasty. 2015;15:e9.
9. Sangha MS, Deroide F, Meys R. Wound healing, scarring and management. Clin Exp Dermatol. 2024;49(4):325-336. doi:10.1093/ced/llad410
10. Wetzig T, Kohn D. Longitudinal slit procedure combined with negative-pressure wound therapy for exposed Achilles tendons. J Dtsch Dermatol Ges. 2017;15(10):1050-1052. doi:10.1111/ddg.13334

















