Chronic Spontaneous Urticaria: Type 2 Inflammation and Mast Cell Hyperreactivity
Chronic spontaneous urticaria (CSU) represents a distinct expression of type 2 inflammation driven by mast cell activation and neuroimmune signaling. In this interview, Dr Raj Chovatiya examines how type 2 cytokines shape CSU’s episodic course.
The Dermatologist: How does type 2 inflammation contribute to mast cell activation in CSU?

Dr Chovatiya: CSU is a newer disease state in the type 2 inflammatory umbrella as it is not one we necessarily thought of with this lens. There has been a lot of recent research to better understand what cytokines like IL-4 and IL-13 are doing in this disease state to contribute to the mast cell activation we know drives a lot of the histaminergic itch that we think about in CSU. There are probably a couple different things happening. We know that IL-4 is a key driver of differentiating naive T lymphocytes to Th2 cells, so that is probably happening centrally, and we know Th2 cells produce a lot of cytokines like IL-4 and IL-13 that then perpetuate inflammation downstream. IL-4 and IL-13 promote B cell activation and class switching, which includes IgE production, and thus it probably enhances autoantibody-mediated mechanisms, as well as trafficking of the immune cells to the site of inflammation. That is probably an important part of this disease too, especially as it relates to where immunoglobulins are involved. At the immune axis, we know that IL-4 and IL-13 can activate and sensitize nerves to a whole diverse host of pruritogens, and so that is probably also enhancing and helping the itch process here. It is believed that all of these in totality are probably leading to mast cell hyperactivity and contributing to this continuous cycle of neuroimmune inflammation.
The Dermatologist: What roles do IL-4 and IL-13 play in IgE-dependent and IgE-independent pathways in CSU?
Dr Chovatiya: IL-4 and IL-13 are 2 cytokines among others that are able to bind directly to mast cells and influence their activity, as well as many of the peripheral and surrounding cells in the mast cell environment in individuals with CSU. More than likely, what is happening in this disease state is rather than IL-4 and IL-13 being singular triggers, they are probably highly influential on the different phenotypes of disease itself, both those that seem to depend on autoantibodies or antibodies like IgE and perhaps even routes that do not depend on that by altering not only mast cell activity, but also neuronal activity in addition to cellular trafficking.
The Dermatologist: How does IL-31 contribute to itch in CSU compared with atopic dermatitis and prurigo nodularis?
Dr Chovatiya: IL-31 seems to be important across most of our itchy type 2 and inflammatory diseases, but perhaps it is a little less important in CSU. This is largely related to the fact that in diseases like atopic dermatitis and prurigo nodularis, we are largely thinking about the activation of non-histaminergic itch pathways. In the case of CSU, a disease state where antihistamines are appropriate, histamine seems to be a major driver of itch. Thus, histaminergic pathways seem to be important here. Now, this does not mean that IL-31 does not still have a role to some degree, but it is a reason why we have seen therapeutic development for agents that block things like IL-4 and IL-13 and not so much IL-31 for CSU, in part because it is believed the predominant mechanism of itch in this disease is going to be mediated by histamine.
The Dermatologist: Why does itch in CSU fluctuate rather than become chronically fibrotic?
Dr Chovatiya: Rather than having low-level or even medium-level continuous activation of immune cells, in the case of CSU, the name implies that there is a spontaneous element to the disease itself. Mast cell degranulation is typically going to be driving bouts of hives, as well as itch and/or angioedema. And mast cell degranulation is not continuously happening all the time. If one were having continuous coordinated mast cell degranulation over the entire body, that would be more like anaphylaxis, with compromise of blood pressure and vascular tone across the entire body. In the case of CSU, you are having random bouts of activation, and so that is the reason why patients can have these unpredictable episodes but then also go through periods where there is not anything happening. This is different than atopic dermatitis, in which there is a little more stability of lesions, although it is waxing and waning to a degree, or prurigo nodularis, which we believe to not be as waxing and waning of a disease but to be rather much more stable.
The Dermatologist: How do neuropeptides and sensory nerves influence mast cell behavior in CSU?
Dr Chovatiya: We have learned a lot in type 2 inflammatory diseases about what is happening at the neuroimmune axis when thinking about peptides produced by cutaneous neurons that act back on immune cells. This is completely true in CSU too. We know that neuroinflammation has an important role here, and there are a variety of receptors directly on the mast cell that can bind to the myriad neuropeptides produced by cutaneous afferents in the skin. Thus, nerves have a really important role to play as being modulators and drivers of mast cell activation, which is a reason why you can think about a variety of different loops causing continued itch and inflammation in this disease.
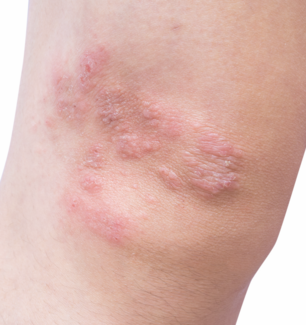
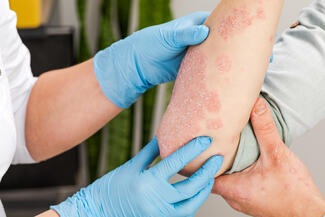
The Dermatologist: What distinguishes CSU as a type 2 disease despite its transient skin lesions?
Dr Chovatiya: Type 2 inflammation as a process can have so many different manifestations and appearances, and if one were to show you a clinical image of an individual with a wheal or prurigo nodule or eczematous plaque, you might be hard pressed to find the similarity. But we know that the pattern with which immune cells, as well as neurons, seem to be involved and activated in these disease states means that there is a lot of shared pathogenesis. In particular, cytokines like IL-4, IL-13, and IL-31 seem to play an important organizing and modulatory role that is driving dysregulation across multiple axes. So even though CSU tends to have episodes of clearance and episodes of involvement and a very different appearance in terms of the rash itself, it belongs in the type 2 inflammatory disease family.
The Dermatologist: Are there any tips or insights you would like to share regarding type 2 inflammation and urticaria?
Dr Chovatiya: When it comes to CSU, we have spent a long time thinking that antihistamines are probably sufficient and if they are not, there must be some other deeper cause or driver of disease that needs to be found. I think the most important point is that about half of our patients with CSU are going to do okay on antihistamines but for the other half, this is going to be the population for whom we think about our many targeted therapies in the type 2 inflammatory umbrella and beyond. As there truly is not going to be an easily ascertainable cause as to why the individual has CSU, searching for the etiology is often going to be fruitless. In this case, if you can diagnose it and you have treatment failure, you can definitely treat your patients and get them on a targeted therapy.