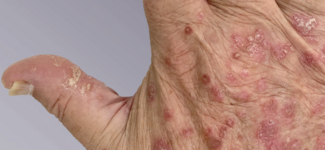
Biosimilars in Dermatology: What Clinicians Need to Know in 2026
 Biologics have reshaped patient care for psoriasis, atopic dermatitis, hidradenitis suppurativa, and chronic urticaria. Now, biosimilars are beginning to emerge as a viable alternative to originator biologics. As biosimilars enter dermatologic practice, they are reshaping prescribing patterns, insurance navigation, and patient conversations by offering highly similar, clinically equivalent alternatives to originator biologics, requiring dermatologists to understand their regulatory framework, safety data, and practical implications for access and care.
Biologics have reshaped patient care for psoriasis, atopic dermatitis, hidradenitis suppurativa, and chronic urticaria. Now, biosimilars are beginning to emerge as a viable alternative to originator biologics. As biosimilars enter dermatologic practice, they are reshaping prescribing patterns, insurance navigation, and patient conversations by offering highly similar, clinically equivalent alternatives to originator biologics, requiring dermatologists to understand their regulatory framework, safety data, and practical implications for access and care.
In this article, we answer common questions dermatologists face about biosimilars, from their scientific and regulatory foundations to their real-world impact on prescribing decisions, payer policies, and patient conversations.
What Is a Biosimilar?
A biosimilar is defined as a biologic that is nearly identical to an already-approved biologic drug and has no clinically meaningful differences in safety, purity, or potency. In practice, that means:
-
The same target and mechanism of action
-
The same route of administration and strength
-
Comparable pharmacokinetics, immunogenicity, and clinical outcomes in focused trials
Biologics used in dermatology are very large, complex glycoproteins. Unlike generics of small molecule drugs, biosimilars are not atom-for-atom copies. While the amino acid sequence of a biosimilar is the same as the reference product, glycosylation and other post-translational modifications may slightly differ, as biologics and their biosimilars are made in living cells. Fundamental to understanding biosimilars is to understand that biologic drugs are so large and complex they cannot be duplicated. These differences are unavoidable and occur even between batches of the original, brand name biologic product. However, different batches of the innovator, although not exactly the same, can be very similar, as are biosimilars. The regulatory standard for biosimilars focuses on high similarity plus absence of clinically meaningful differences, creating a product that is functionally identical to a batch of the reference biologic.
What Does Interchangeable Mean?
Interchangeable is a regulatory label in the United States. While there are multiple biosimilars for some biologic drugs, not all are interchangeable. A biosimilar is highly similar to the reference product, with no clinically meaningful differences in safety or efficacy. An interchangeable biosimilar meets additional US Food and Drug Administration requirements so that, depending on state law, a pharmacist may substitute it for the reference product without contacting the prescriber.
Interchangeable status requires data comparing patients who alternated between the reference biologic and biosimilar compared to patients who continued the reference biologic. Clinically, interchangeable does not mean safer or more effective than a non-interchangeable biosimilar. This definition mainly affects pharmacy-level substitution and state law.
Where Do Biosimilars Touch Dermatology Today?
Biologic drugs that now have US biosimilars include:
-
Adalimumab
-
Infliximab
-
Ustekinumab
-
Omalizumab
Several psoriasis biologics still do not have approved biosimilars, including secukinumab, ixekizumab, and risankizumab, although candidates are moving through development. Etanercept biosimilars exist internationally, but US market entry has been delayed by patent issues.
What About Safety, Immunogenicity, and Switching?
Regulators require evidence that includes detailed comparability, nonclinical data, pharmacokinetics, immunogenicity, and at least one clinical study for each indication.
For TNF biosimilars (adalimumab, infliximab, etanercept), randomized and real-world data support:
-
Comparable efficacy scores, such as Psoriasis Area and Severity Index and Physician Global Assessment
-
Similar immunogenicity profiles and anti-drug antibody rates
-
No new safety signals when switching from the original biologic to the biosimilar, or between biosimilars
Meta-analyses across biosimilars have not shown increased risk of death, serious adverse events, or treatment discontinuation in patients who switched compared with those who did not.1 For dermatology, high-quality psoriasis-specific data exist for adalimumab and infliximab,2,3 and more data are emerging for ustekinumab and omalizumab biosimilars as they reach the market.4,5
Are Side Effects or Monitoring Different?
Regulators license biosimilars with the same core safety information and monitoring recommendations as their reference products. In practice:
-
Screening (tuberculosis, hepatitis B), vaccination, and infection counseling are the same.
-
Contraindications and boxed warnings are the same.
-
Needle, syringe, or autoinjector design may differ, which can change patient preference and usability but not core safety requirements.
Formulation differences, such as high vs low concentration or citrate free, may affect tolerability at the injection site or adherence, but these differences also exist between different presentations of the reference biologics.
My Patient’s Insurer Will Only Cover a Biosimilar. What Do I Need to Know?
Biologics account for a large share of specialty drug spending. Biosimilars may (or may not) be more affordable to patients, and several biosimilar manufacturers have payment assistance programs to help improve drug access. As more competition arrives in the market, costs may continue to decrease, reducing the health care resources spent on biologic treatment and possibly having some modest effect on premiums. It seems unlikely that costs will drop so much that coverage policies will increase accessibility or reduce prior authorization requirements. Each insurer may have a preferred biologic drug, depending on their contracting, which may change over time, resulting in burden to both the physician’s practice and the patient who must access the resulting support program.
Patients may be concerned that their “new” biologic may not work as well as the old one and may ascribe any adverse event that occurs to the change. Explaining that even the innovator varies from batch to batch may help.
Conclusion
Biosimilars are a growing reality in dermatology that influences daily clinical decision-making. Regulatory standards and clinical data support their safety, efficacy, and interchangeability with reference biologics, including during treatment switching. While biosimilars may help moderate health care spending, they also introduce new complexities related to insurance coverage, pharmacy substitution, and patient perception. By understanding how biosimilars are developed, regulated, and implemented, dermatologists can confidently guide patients through transitions in therapy, address concerns about safety and effectiveness, and continue to deliver high-quality, evidence-based care in an evolving biologic landscape.
References
- Herndon TM, Ausin C, Brahme NN, et al. Safety outcomes when switching between biosimilars and reference biologics: a systematic review and meta-analysis. PLoS ONE. 2023;18(10):e0292231. doi:10.1371/journal.pone.0292231
- Phan DB, Bewley AP, Laws P, et al. Effectiveness of adalimumab biosimilars and originator for psoriasis. JAMA Dermatol. 2025;161(4):358-366. doi:10.1001/jamadermatol.2025.0055
- Morita A, Nishikawa K, Yamada F, Yamanaka K, Nakajima H, Ohtsuki M. Safety, efficacy, and drug survival of the infliximab biosimilar CT-P13 in post-marketing surveillance of Japanese patients with psoriasis. J Dermatol. 2022;49(10):957-969. doi:10.1111/1346-8138.16508
- Feldman SR, Narbutt J, Girolomoni G, et al. A randomized, double-blind, phase III study assessing clinical similarity of SB17 (proposed ustekinumab biosimilar) to reference ustekinumab in subjects with moderate-to-severe plaque psoriasis. J Am Acad Dermatol. 2024;91(3):440-447. doi:10.1016/j.jaad.2024.04.045
- Saini SS, Maurer M, Dytyatkovska Y, et al. CT-P39 compared with reference omalizumab in chronic spontaneous urticaria: results from a double-blind, randomized, active-controlled, phase 3 study. Allergy. 2025;80(8):2167-2177. doi:10.1111/all.16446