Pregnancy Dermatoses: The Itchy Patient, the Dangerous Diagnosis, and the Referral That Can’t Wait
At the 2026 Masterclasses in Dermatology Annual Meeting, Katherine Economy, MD, MPH, delivered a clinically focused session on dermatologic disease in pregnancy, highlighting the balance between reassurance and urgent referral. Her framework was straightforward: recognize normal changes, treat benign dermatoses appropriately, and identify high-risk conditions early.
Dr Economy began by reviewing physiologic skin changes in pregnancy, including melasma, striae gravidarum, linea nigra, hyperhidrosis, spider angiomas, and postpartum hair shedding. Nevi may expand over the abdomen and breasts, and nipple discharge should be “clear/milky,” with any bloody discharge warranting evaluation.
Pruritus is common: “40% pregnant patients experience itching,” and notably, “60% have no rash.” While social media cures are plentiful, systematic assessment is essential.
Atopic eruption of pregnancy is the most common dermatosis in pregnancy. It presents as an “eczematous or papular eruption,” typically in the first or second trimester, and is managed symptomatically with low- to mid-potency topical corticosteroids and antihistamines. Recurrence rates are high.
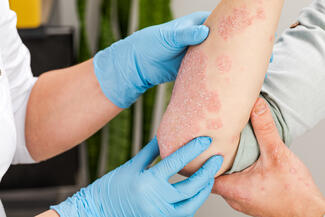
Polymorphic eruption of pregnancy (PEP), affecting approximately 1 in 160 pregnancies, arises late in pregnancy or immediately postpartum. Lesions often begin in striae and “typically spare the umbilical region.” Importantly, PEP is “not associated with adverse maternal or fetal outcomes” and can be treated with mid- to high-potency topical steroids.
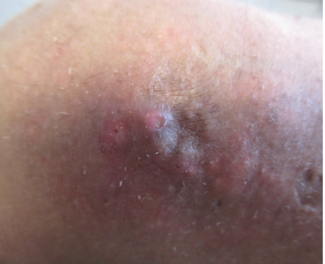
More concerning is pemphigoid gestationis, described as an “intensely itchy urticaria-like rash during mid to late pregnancy.” Direct immunofluorescence shows linear C3 deposition along the dermoepidermal junction. Fetal risks include growth restriction, preterm birth, and stillbirth, and “flares are likely postpartum.” A biopsy is critical when suspected.
Pustular psoriasis of pregnancy, a rare variant of generalized pustular psoriasis, may mimic acute drug reactions and requires systemic therapy, such as corticosteroids, cyclosporine, or infliximab, with close maternal-fetal monitoring and potential early delivery.
Intrahepatic cholestasis of pregnancy represents a dermatologic emergency masquerading as itch. It presents as “pruritus without rash,” often with elevated bile acids. Early delivery is recommended for the highest-risk patients, particularly when bile acids exceed 40 mmol/L. Treatment includes ursodeoxycholic acid 600 mg twice daily.
Dr Economy concluded with clear guidance: “Pregnant patients with new eruptions/ pruritus require urgent evaluation. For pruritic patients without lesions, check bile acids.”
For more meeting coverage, visit the Masterclasses in Dermatology newsroom.
Reference
Economy K. Dermatologic considerations in pregnancy: when to relax, when to refer. Presented at: Masterclasses in Dermatology; February 19–22, 2026; Sarasota, FL.