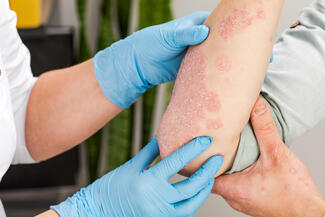
Plaque Psoriasis Treatment Therapeutics: Oral IL-23 Inhibitors
At the 2026 Masterclasses in Dermatology Annual Meeting, Andrew Blauvelt, MD, MBA, reframed psoriasis care through a patient-centered lens, stating that undertreatment remains a persistent barrier despite an expanding biologic armamentarium.
Dr Blauvelt started with the impact of psoriasis in quality of life. “When you see a patient with psoriasis, assume that their life is impaired, assume that they’re struggling.” Dr Blauvelt encouraged to warn patients about comorbidities like heart disease. “Increasing evidence supports the recognition of psoriasis as a multisystem chronic inflammatory disorder with multiple associated co-morbidities.”
“Don’t undertreat psoriasis; treat to clearance (Psoriasis Area and Severity Index [PASI] 100) or near clearance,” he emphasized, noting that approximately 25% of patients have untreated or undertreated moderate-to-severe psoriasis. Traditional severity definitions based solely on body surface area (BSA) underestimate disease involving high-impact sites, such as the scalp, face, palms/soles, nails, and genitalia. Under updated National Psoriasis Foundation and International Psoriasis Council reclassification statements, patients with special-area disease or failure of topical therapy are candidates for systemic therapy, even with BSA 1% to 4%, not just BSA >10%. Dr Blauvelt defined the failure of topical therapy as “inability to achieve clear/nearly clear skin (BSA 1%, Physician’s Global Assessment 0/1) after 2 consecutive 4-week topical therapy courses, per guidelines.”
Dr Blauvelt emphasized the clinical importance of complete skin clearance in psoriasis. “Improvements in mental health have been reported following treatment of psoriais with systemic therapy.”
As for the biologics, IL-23 inhibitors have emerged as a leading biologic class. “Current biologic choices are excellent, especially IL-23 inhibitors,” Dr Blauvelt stated. “IL-23i deliver in all 3 areas—efficacy, safety, and convenience.” Unlike TNF inhibitors and JAK inhibitors, “IL-23 and IL-17 inhibitors do not impair granuloma formation, do not affect Th1 immunity, and are not involve in control of latent tuberculosis.”
The next frontier is oral IL-23 blockade. “Emerging oral IL-23 inhibitors provide excellent efficacy, safety, and convenience for patients.” TYK2 inhibitors are advancing. Zasocitinib and envudeucitinib demonstrated short-term efficacy in phase 2 trials exceeding that seen with earlier TYK2 agents. Long-term data for envudeucitinib show maintained responses, positioning TYK2 inhibition as a competitive oral strategy. “They are novel TYK2 inhibitors, better than deucravacitinib, and are also being studied in psoriatic arthritis and lupus.”
Icotrokinra, a small-molecule drug, is a targeted peptide that “blocks IL-23 from binding to its receptor,” demonstrating robust phase 3 efficacy. In 2 pivotal trials, icotrokinra achieved statistically superior Investigator Global Assessment 0/1 and PASI 90 responses compared with deucravacitinib. Efficacy was also demonstrated in high-impact sites, addressing a key unmet need. Once-daily dosing on an empty stomach enhances convenience.
Emerging oral IL-23 inhibitors “provide excellent efficacy, safety, and convenience for patients,” concluded Dr Blauvelt. “Benefits of treating psoriasis go beyond the skin,”
For more meeting coverage, visit the Masterclasses in Dermatology newsroom.
Reference
Blauvelt A. Transforming psoriasis care: oral IL-23 therapy and the next frontier in patient-centered treatment. Presented at: Masterclasses in Dermatology; February 19–22, 2026; Sarasota, FL.