Ocular Red Flags in Dermatology: Uveitis, Cicatrizing Conjunctivitis, and Hydroxychloroquine Toxicity
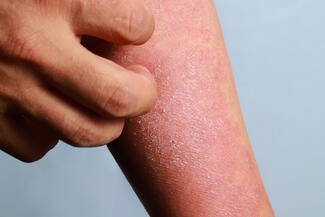
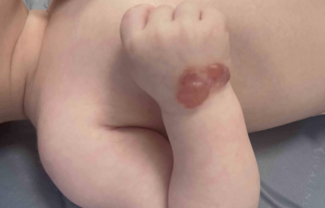
Jennifer Cao, MD, delivered a focused review of high-yield ocular manifestations that dermatologists cannot afford to miss during her Masterclasses in Dermatology session, “Ocular Signs of Systemic Disease.” Her objectives included identifying dermatologic and systemic diseases associated with uveitis, recognizing ocular findings in autoimmune bullous disease and Stevens-Johnson syndrome/toxic epidermal necrolysis (SJS/TEN), and reviewing updated 2026 hydroxychloroquine toxicity screening recommendations.
Uveitis, defined as inflammation of the iris, ciliary body, or choroid, can be classified by etiology or anatomic location (anterior, intermediate, posterior, panuveitis) under Standardization of Uveitis Nomenclature, or SUN, criteria. Although up to 90% of cases are isolated to the eye, dermatologists should recognize associations with HLA-B27 disease, psoriasis, inflammatory bowel disease, sarcoidosis, juvenile idiopathic arthritis, and Behçet syndrome.
Patients may present with redness, pain, photophobia, floaters, or decreased vision. Clinical signs include anterior chamber “cell and flare,” keratic precipitates, posterior synechiae, and retinal vasculitis. Treatment goals are to relieve discomfort, control inflammation, treat the underlying disease, and prevent irreversible damage.
Topical corticosteroids are first line for anterior uveitis, with oral or periocular steroids serving as a bridge to immunomodulatory therapy in chronic or posterior disease. Dr Cao emphasized steroid stewardship: “Patients should be completely quiet, completely off steroids, within 2 to 3 months.” Adalimumab remains the only US Food and Drug Administration approved steroid-sparing agent for noninfectious intermediate, posterior, and panuveitis.
Autoimmune bullous diseases and SJS/TEN can cause severe cicatrizing conjunctivitis. Dry eye is common in both pemphigus and pemphigoid, but conjunctival scarring typically occurs in pemphigoid. The Foster grading system progresses from subepithelial fibrosis (stage 1) to limbal stem cell deficiency and blindness (stage 4). Conjunctival biopsy may worsen staging; as Dr Cao stated, “I stopped doing them 10 years ago.”
Hydroxychloroquine retinal toxicity is irreversible, making early detection critical. Updated 2026 guidance recommends baseline screening at initiation, no annual screening during the first 5 years unless high risk, and annual screening after 5 years of therapy. Primary tests include spectral-domain optical coherence tomography, fundus autofluorescence, and 10-2 visual field testing, with expanded fields in high-risk populations. High-risk factors include daily dose >5 mg/kg actual body weight, renal dysfunction, tamoxifen use, older age, and East Asian race.
Dr Cao closed with a principle that extends across inflammatory eye disease management: “The quest for steroid-free remission buys ‘vision time.’”
For more meeting coverage, visit the Masterclasses in Dermatology newsroom.
Reference
Cao J. Ocular signs of systemic disease. Presented at: Masterclasses in Dermatology; February 19–22, 2026; Sarasota, FL.