Adventist Health Tulare Medical Center
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of EP Lab Digest or HMP Global, their employees, and affiliates.
EP LAB DIGEST. 2026;26(3).
Marilyn Benitez, BS RT(R)(ARRT), CRT, Manager, Cardiac Catheterization
Adventist Health, Tulare, California
When was the cardiac electrophysiology (EP) program started at your institution, and by whom?
Adventist Health Tulare is an acute-care hospital with approximately 101 licensed beds. The EP program was launched in September 2024 with the arrival of electrophysiologist Sukhvinder Bhajal, MD.

What drove the need to implement an EP program?
Before establishment of the EP program, residents of Tulare County had limited access to specialized cardiac care. Patients often faced long travel times to receive treatment, resulting in delays and increased health care costs. The EP program was developed to provide local access to advanced EP services, thereby reducing travel burdens and improving timely care delivery.

Describe your city or general regional area. How is it unique?
Tulare, California, is a vibrant city situated in the heart of the San Joaquin Valley—one of the world’s most fertile and productive agricultural regions. Its uniqueness stems from a deep connection to agriculture and a strong community spirit. Tulare serves as a key hub for dairy farming, citrus orchards, and various crops, significantly contributing to both California’s and the nation’s food supply. As of 2025, Tulare has an estimated population of approximately 72,264 residents, with steady annual growth of around 0.82%, reflecting a close-knit and culturally diverse community with economic opportunity and natural beauty.
Who manages your EP lab?
Patrick Hoffman serves as the director of cardiopulmonary services. The day-to-day operations are coordinated and managed by Marilyn Benitez, manager of the cardiac catheterization lab.
What is the number of staff members? What is the mix of credentials?
Our dedicated EP team consists of approximately 11 expert members, all cross-trained in EP, cardiac catheterization, and interventional radiology (IR). Staff credentials include registered nurses (RNs) and radiologic technologists.
What types of procedures are performed at your facility?
We provide a comprehensive range of EP services, including cardioversions, device implantations, and catheter ablations. Device implantations cover implantable loop recorders, transvenous pacemakers, implantable cardioverter-defibrillators (ICDs), biventricular ICDs, traditional cardiac resynchronization therapy devices, subcutaneous ICDs, and leadless pacemakers. Ablation procedures performed include supraventricular tachycardia, right and left atrial flutter, biatrial flutter, atrial fibrillation (AF), and atrioventricular node ablation.
What types of EP equipment are most commonly used in the lab?
Our lab uses the CardioLab EP Recording System (GE HealthCare) with Micropace EP stimulators. For 3-dimensional (3D) mapping, we utilize the Carto System (Johnson & Johnson MedTech). Diagnostic EP catheters from Abbott and Johnson & Johnson MedTech are standard. For complex ablations, we employ intracardiac echocardiography (ICE) using CartoSound (Johnson & Johnson MedTech) and AcuNav (Vivid, GE HealthCare) mapping.

What are some new technologies and techniques recently introduced in your lab?
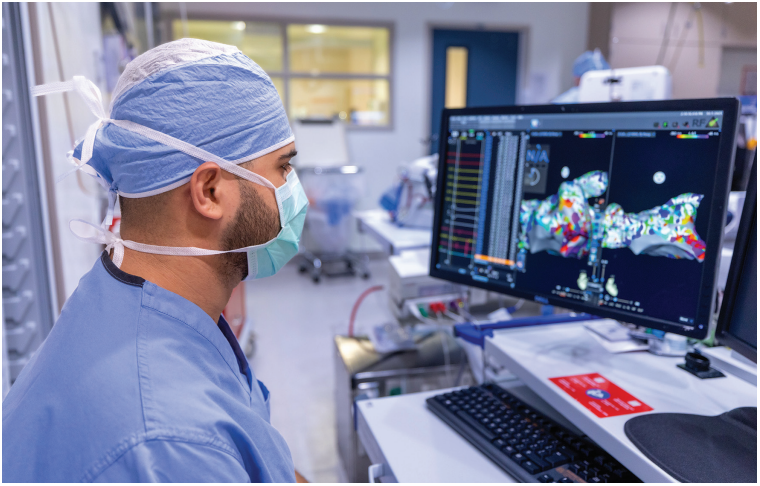
We recently introduced pulsed field ablation (PFA) technology to treat AF. PFA enables selective ablation of myocardial tissue while minimizing damage to surrounding structures such as the esophagus and phrenic nerve. We utilize the Varipulse catheter (Johnson & Johnson MedTech), which supports both focal and multipolar ablation and is compatible with our 3D mapping systems. This technology has enhanced procedural efficiency and patient safety by reducing procedure times, minimizing sedation needs, and providing particular advantages in the management of persistent AF. Our team has enthusiastically embraced this transition and is already witnessing excellent patient outcomes.
Can you describe the extent and use of vascular closure devices in your lab?
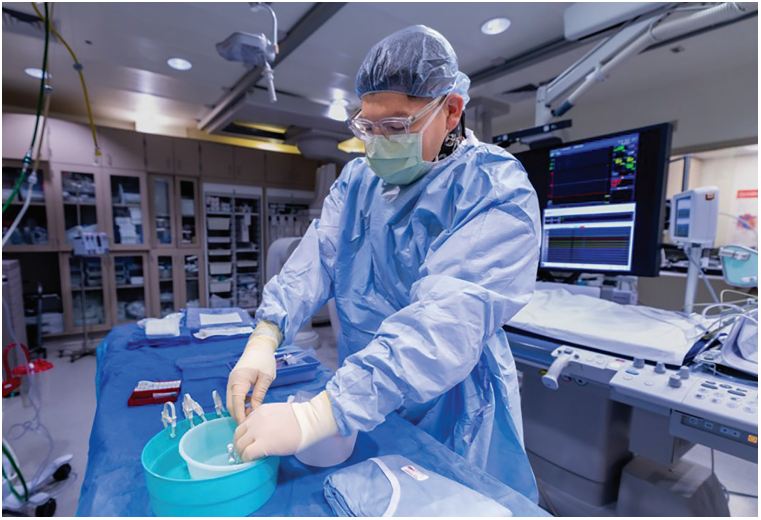
Patients undergoing AF ablation are discharged on the same day. We routinely use vascular closure devices to promote efficient and safe hemostasis after arterial and venous access. For arterial punctures, Mynx Control Vascular Closure Device (Cordis) and Perclose ProGlide Suture-Mediated Closure System (Abbott) devices are most commonly used, depending on the clinical context. We recently introduced the Vascade Vascular Closure System (Haemonetics) for use in AF procedures. Its use has improved recovery time and patient comfort, reflecting our commitment to enhancing clinical outcomes and patient experience.

How are new employees oriented and trained at your facility?
New team members undergo a 5-week preceptorship, working alongside experienced staff and rotating through various lab roles. This hands-on training ensures comprehensive exposure to procedures and protocols. Afterward, team members work more independently but remain under close supervision to support their continued growth. The EP lab is integrated with the cath lab, so staff are cross-trained to assist in EP, coronary, and IR procedures, fostering versatility and teamwork.
What approaches has your lab taken to reduce fluoroscopy time?
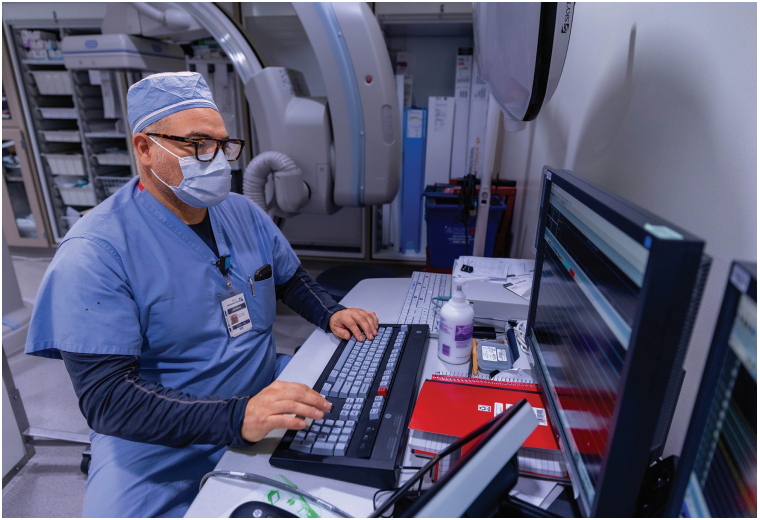
We minimize fluoroscopy by routinely using 3D electroanatomical mapping systems, often eliminating the need for fluoroscopy during procedures. When fluoroscopy is necessary, we use low-dose settings to reduce radiation exposure for both patients and staff.
In what ways have you cut or contained costs in the lab or device clinic?
We actively collaborate with industry partners to negotiate competitive pricing on equipment and supplies. Additionally, we use third-party reprocessing services for ICE and certain diagnostic EP catheters, helping reduce disposable costs without compromising quality or safety.
How is inventory managed?
Inventory management is handled by our lead RNs, who track supply levels, monitor expiration dates, and ensure availability of essential equipment. This hands-on management minimizes waste and maintains efficient stock rotation.
What are some of the dominant trends you see emerging in the practice of EP?
Two key trends shaping EP today include:
- Remote monitoring and digital health: The rise of remote device monitoring and telehealth enables real-time data sharing and proactive patient management, improving outcomes while reducing hospital visits.
- Personalized medicine and artificial intelligence (AI) integration: AI and machine learning tools are increasingly used to predict arrhythmia risk, tailor treatments, and optimize procedural success, leading to more personalized and effective care.
Please tell our readers what you consider special about your EP lab and staff.
Our EP lab is unique due to the diversity and dedication of our team members who reflect the multicultural community we serve. This diversity enhances our ability to deliver culturally sensitive, compassionate care. Our EP program was introduced as a new service line within the cath lab without an onsite cardiac surgery program. With the dedication of our skilled team and strong institutional support, we provide safe, advanced EP procedures that deliver consistent, high-quality results. Most importantly, we are proud to provide advanced EP services locally—care that was previously unavailable close to home—bringing significant benefits to our community and overall regional health.










