Building a High-Performance Electrophysiology Program in an Ambulatory Surgery Center: Lessons From a 3-Year Journey at an Independent Cardiovascular Group
Lessons From a 3-Year Journey at an Independent Cardiovascular Group
Lessons From a 3-Year Journey at an Independent Cardiovascular Group
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of EP Lab Digest or HMP Global, their employees, and affiliates.
EP LAB DIGEST. 2026;26(3).
Vivak Master, MD, cardiac electrophysiologist
Virginia Cardiovascular Specialists, Richmond, Virginia
Why Move Cardiac Electrophysiology (EP) Into an Ambulatory Surgery Center (ASC)?
Nationally, more than 80% of surgeries now occur in outpatient settings.1 ASCs are playing an increasingly central role in this shift. Their growth has been supported by advances in technology, stricter regulatory oversight, maturation of the ASC operating models, and consistent demonstration of procedural safety.2-4 In addition to these factors, independent ASCs offer several advantages over hospitals, including:
- Streamlined alignment between clinical and administrative teams.
- Reduced bureaucracy and faster decision-making, which can lead to faster implementation of new technology.
- ASCs are 35% to 50% less costly than hospital outpatient departments (HOPDs) for many cardiovascular procedures, lowering the overall cost to both patients and insurers.5,6
Cardiology is amongst the fastest-growing specialties in the ASC setting, driven by cost pressures, challenges in patient access, and the ability to deliver high-quality care in an efficient and safe manner.7 Virginia Cardiovascular Specialists (VCS), an independent cardiovascular group, recognized this trend early. Delays in non-emergent hospital cases due to inconsistent scheduling and frequent pushback due to emergent patient procedures were a significant challenge for both patients and providers. The ASC model was envisioned as a way to mitigate these issues by enabling treatment of patients appropriate for outpatient care, independent of hospital pressures.
The vision was clear: to build an EP-capable ASC that improved access, alleviated pressure on hospital EP labs, and created a predictable, patient-centered experience. With this vision in mind, VCS opened the first Medicare-certified cardiovascular ASC in Virginia in 2023, followed by the state’s first freestanding cardiac catheterization lab in 2024.

Designing the VCS ASC: Intentionality From Day One
From the outset, VCS sought to design an ASC that would evolve with the increasing complexity of outpatient cardiovascular care. Planning began years before opening, by creating a physician-led VCS ASC Governing Board that would make decisions around policies, equipment, staffing, and safety.
The search also centered on identifying a location with key design attributes for patient safety and convenience, as well as logistical flexibility, including:
- Proximity to a hospital, ensuring prompt transfer and intervention in a hospital setting in the event of a procedural complication. The ASC is located 0.7 miles from Henrico Doctors’ Hospital, allowing transfers to occur within a few minutes.
- Direct ambulance access at the rear entrance for transfers that preserve patient privacy.
- First-floor location with direct parking access, minimizing patient navigation challenges.
- Pre- and postoperative areas configured for visibility and efficient circulation, 2 procedure suites, and family waiting area.
- Physician involvement in the design process to ensure that the facility and lab design matched clinical workflow.
- Flexible architectural and electrical design, anticipating equipment expansion, anesthesia needs, and EP workflow adaptations (eg, lighting needs, mapping system placement, and room size).
- Hiring staff experienced in ASC and EP workflows significantly reduced the startup learning curve, allowing a rapid increase in the number of procedures performed over time. Most of the staff came from cardiac catheterization and EP labs at hospitals in the area. Those who were hired were seeking a different work environment—one that enabled more predictable scheduling and a better work/life balance than the hospital setting could adequately provide.
The facility was engineered with stringent certification requirements in mind, ensuring compliance with all applicable local, state, and federal rules and regulations. The ASC is a Centers for Medicare & Medicaid Services (CMS)-certified facility and accredited by the American Association for Accreditation of Ambulatory Surgery Facilities (Quad A).
Initially, the ASC was limited to cardiac implantable electronic device (CIED) implantation and peripheral vascular procedures. Anticipating which additional cardiovascular procedures might receive future approval—and determining which of them could be performed safely in the ASC—was essential. Infrastructure decisions were made to support the performance of future procedures, including coronary interventions and, eventually, cardiac ablation. These decisions included having an appropriate power supply, shielding, gas connections, and heating, ventilation, and air conditioning system.
The benefit of early planning was seen once approval for more types of procedures was obtained. Retrofitting was greatly minimized, which reduced the overall expense and disruption to daily operations. One major cost was the fluoroscopy system. The ASC initially started with the OEC Elite portable C-arm fluoroscopy system (GE HealthCare). This saved on the initial cost of opening the ASC and was an adequate system for CIED implantation and peripheral vascular procedures. The laboratory was designed to easily upgrade to a fixed fluoroscopy system, so once coronary procedures were approved, the ASC upgraded to the Azurion 7 fixed fluoroscopy system (Philips) with minimal delay. The portable C-arm was then moved to the procedure room.
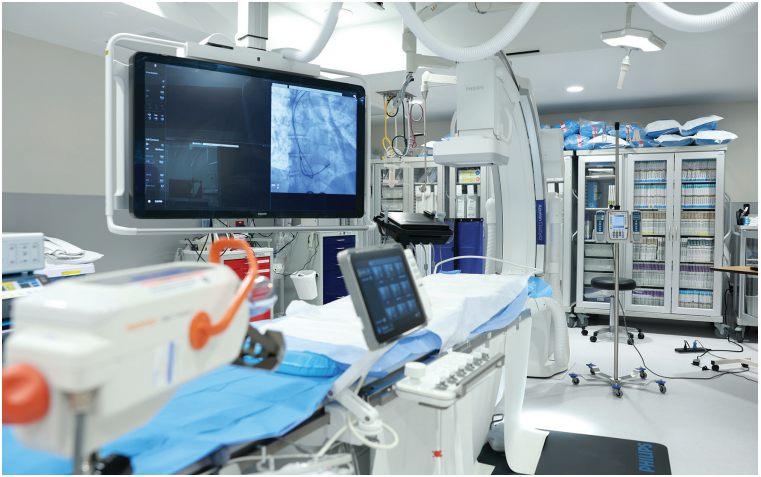
Operational Performance After 3 Years
Now approaching the 3-year mark, the ASC has produced measurable impacts on safety, efficiency, throughput, and patient experience.
- Safety and outcome. Only patients suited for outpatient care are treated, aligning with the Ambulatory Surgery Center Association’s national guidance that ASCs safely serve appropriate patient populations through rigorous screening, regulatory review, and strong safety protocols. Along with clinical judgement, physicians agreed on certain factors to be considered in patient selection, including: the presence of pulmonary disease and requirement of home supplemental oxygen, NYHA class, body mass index, and other chronic illnesses that would make sedation in the non-hospital setting difficult. Patients with an increased risk of respiratory decompensation, those likely to require closer monitoring or anesthesia services, or those expected to require overnight observation did not undergo procedures in the ASC. For coronary and peripheral vascular patients, preoperative imaging is performed with computed tomography angiography. Using these selection criteria, more than 99% of EP patients were safely discharged home in 2024. One patient required transfer to the hospital for pericardial effusion, and 2 were transferred for pneumothorax, resulting in a hospital transfer rate of 0.2% for EP patients in 2025. The patient with pericardial effusion underwent pericardiocentesis safely at the ASC before being transferred to the hospital for further management. The patients with pneumothoraces were managed conservatively with supplemental oxygen. All transferred patients were discharged home in stable condition after a few days.
- Efficiency and workflow. Clinical efficiency was identified as one of the most critical, and most challenging, operational components. Having a dedicated scheduling team for the ASC, reviewing procedural times and workflows for different operators, and adjusting non-ASC clinical coverage responsibilities for physicians very quickly allowed staff to maintain highly predictable start times and allow late add-ons when clinically needed. These factors enabled results such as the room turnover time averaging 12.6 minutes, significantly outperforming the national hospital average of 18.4 minutes.8
- Case volume. Through improvement in operational efficiencies, annual case volume has more than tripled. In 2023, approximately 450 cases were performed. The expected volume for 2025 is greater than 1400. This includes EP, coronary, and peripheral vascular procedures. Approximately 70% of all VCS outpatient EP device procedures now occur at the ASC. All procedures were performed in either the cardiac catheterization or procedure lab between 7:30 AM and 5:00 PM.
- Patient experience. Initially, paper surveys were given to patients, but these were difficult to compare to standardized metrics. In 2025, this was transitioned to Press Ganey, which provided standardized metrics and top-box performance reporting. Patients consistently reported satisfaction in ease of parking and building navigation, shorter wait times, more predictable scheduling, clearer communication, and a calmer, less intimidating environment than large hospitals. Patient comments highlighted consistent themes of professionalism, comfort, clarity of communication, and perceived safety, with comments such as “Beyond excellent…I was extremely impressed with the entire experience,” “The entire team was friendly, competent, and reassuring,” and “Communication from start to finish was exemplary.”
The ASC as a Platform for Growth
The ASC was intentionally designed as a scalable platform—structurally, operationally, and strategically. One of the major uncertainties, until recently, involved cardiac ablations. For 2026, CMS approved the performance of key cardiac catheter ablation procedures in the ASC setting. Although the facility was designed with this capability in mind, VCS is currently completing feasibility assessments (ie, clinical, reimbursement, safety, and equipment) to incorporate ablations in the next phase of ASC development. Ablation procedures bring certain challenges that ASCs must address in advance to ensure successful program implementation. For example:
- Mapping systems and catheters can be costly, and with a wide range of available options, partnership with industry is key. Success will depend on selecting a cost-effective system that all operators are comfortable using that supports high procedural efficacy and efficiency.
- Appropriate anesthesia capabilities are essential, as anesthesia resources can limit growth. An early decision was made to use conscious sedation in the ASC. A dedicated nurse was hired to administer sedation under physician supervision, allowing procedures to begin without the additional complexity and overhead associated with certified registered nurse anesthetist or anesthesiologist staffing. This approach aligned with current practice in many hospitals, where CIED implants are safely performed with moderate sedation under physician supervision. Patient selection for the ASC was guided by this planned level of sedation. Anesthesia staffing is a challenge, and innovative strategies will be required to address issues such as reimbursement and scheduling. These considerations will become increasingly important with the introduction of ablation procedures, particularly pulsed field ablation (PFA). Requirements for general anesthesia availability are being addressed, while PFA systems that may be suitable to moderate sedation are also being evaluated.
- Emergency protocols will need to be clearly defined to address the added complexity associated with general anesthesia and left atrial procedures.
- Scheduling blocks and throughput modeling will need to be refined to accommodate the specific demands of an ablation workflow.
- Training tailored to ablation workflows will be necessary for all involved staff.
Impact on Hospital Partners
Although VCS Heart and Vascular Center is wholly owned by VCS, the transition to an ASC setting was not made in isolation, as it was expected to affect hospital procedural volume and coverage. By shifting lower-acuity, non-urgent cases to the ASC, partner hospitals have been able to prioritize higher-acuity patients in a timelier manner.
Lessons Learned: What Other Programs Should Know
Performing procedures in an ASC setting has provided substantial benefits for both patients and VCS physicians. Early experience in this environment has identified several key components that should be prioritized by those seeking to develop a similar program.
Design
- Plan with the future state in mind.
- Build flexible rooms and infrastructure to accommodate growth and new procedures.
- Consider proximity to a hospital; nearby access enhances safety and provides peace of mind.
Staffing
- Employ ASC-experienced nurses and technologists, as they are essential to early success.
- Prioritize effective scheduling by continually optimizing preoperative, procedural, and postoperative workflows without compromising patient safety.
Operations
- Anticipate a brief honeymoon period for the first few months, followed by the need for meaningful adjustments.
- Maintain strong vendor partnerships to ensure equipment support, pricing stability, and consistent uptime.
- Establish a physician-driven governance structure early.
- Review accreditation requirements carefully to ensure compliance with nationally accepted standards
Clinical
- Develop clear patient-selection criteria; outpatient appropriateness is central to safety.
- Use preoperative diagnostic tools to improve triage and minimize patient risk.
Strategic
- Leverage the ASC setting to amplify the strengths of an independent group—nimbleness, alignment, and rapid iteration.
- Understand that costs escalate quickly; model procedural volume, staffing needs, and reimbursement scenarios well in advance.
Summary
EP is currently undergoing a significant and exciting transition. Financial pressures, evolving regulations, and the emergence of new ablation techniques—such as PFA—have positioned the ASC as the clear future for many EP procedures, and the field is still in its early stages of this shift. At VCS, the practice has emphasized forward-thinking innovation. With strong clinical leadership and intentional planning, as outlined above, the organization has positioned itself to expand its ASC presence safely and efficiently while navigating new challenges that will arise as CMS continues to broaden the list of approved procedures.
Disclosures: The author has completed and returned the ICMJE Form for Disclosure of Potential Conflicts of Interest. Abhi S Grewal reports no disclosures. Dr Master reports consulting fees from Abbott regarding proctorship for a conduction system pacing training program.
References
- Munnich EL, Parente ST. Returns to specialization: evidence from the outpatient surgery market. J Health Econ. 2018;57:147-167. doi:10.1016/j.jhealeco.2017.11.004
- Goldfarb CA, Bansal A, Brophy RH. Ambulatory surgical centers: a review of complications and adverse events. J Am Acad Orthop Surg. 2017;25(1):12-22. doi:10.5435/JAAOS-D-15-00632
- Qin C, Lee C, Ho S, Koh J, Athiviraham A. Complication rates following hip arthroscopy in the ambulatory surgical center. J Orthop. 2019;20:28-31. doi:10.1016/j.jor.2019.12.009
- MedPAC. Chapter 10: ambulatory surgical center services: status report (March 2024 report). Published March 15, 2025. Accessed December 10, 2025. https://www.medpac.gov/document/chapter-10-ambulatory-surgical-center-services-status-report-march-2024-report/
- Aryana A, Thihalolipavan S, Willcox ME, et al. Safety and feasibility of cardiac electrophysiology procedures in ambulatory surgery centers. Heart Rhythm. 2025;22(3):717-724. doi:10.1016/j.hrthm.2024.07.123
- Marshall S, Barrington A, Yih S, Kwao S. Cardiac ablations in ambulatory surgical centers: estimated costs, utilization, and projected savings. Milliman. Published May 16, 2025. Accessed December 10, 2025. https://www.milliman.com/en/insight/cardiac-ablations-ambulatory-surgical-centers-costs-savings
- Li K, Kalwani NM, Heidenreich PA, Fearon WF. Elective percutaneous coronary intervention in ambulatory surgery centers. JACC Cardiovasc Interv. 2021;14(3):292-300. doi:10.1016/j.jcin.2020.10.015
- State of the industry report: best practices and industry benchmarks for optimizing ASC operations. HST Pathways. Published September 2024. Accessed January 20, 2026. https://www.hstpathways.com/wp-content/uploads/2024/10/HST-Pathways-2024-State-of-the-Industry-Report.pdf










